Welcome to HB BodyLab
Physical Therapy
Physical therapy (PT) is a healthcare specialty focused on preventing, treating, and managing movement disorders and physical impairments. At HB BodyLab, our physical therapists are musculoskeletal experts who utilize various techniques and exercises to enhance patients’ physical function and mobility, alleviate pain, and prevent injury or disability.
As Featured IN:
How Can Physical Therapy Help Your Recovery?
Physical therapy (PT) is a specialized healthcare field dedicated to the prevention, treatment, and management of movement disorders and physical impairments. At HB BodyLab, our expert physical therapists specialize in musculoskeletal health, employing a variety of techniques and exercises to enhance physical function and mobility, alleviate pain, and prevent injuries or disabilities.
PT is frequently recommended for numerous conditions, including musculoskeletal injuries, neurological disorders, sports injuries, chronic pain, and recovery after surgery. Depending on individual needs and circumstances, PT sessions might include manual therapy, strength training, mobility exercises, and modalities such as ultrasound, electrical stimulation, and thermal therapies.
In Huntington Beach, our physical therapists utilize advanced methods to help patients regain independence and improve their quality of life by restoring physical capabilities, reducing pain, and boosting overall health. Each therapy session is tailored to meet your specific needs and goals.
We adopt patient care practices backed by research, focusing on comprehensive approaches that effectively address all aspects of function. Rather than merely treating symptoms, we aim to identify and resolve the root causes of your issues, ensuring lasting results.
Conditions Treated With Physical Therapy
At HB BodyLab, we recognize the unique paths our patients take and the challenges they encounter with various conditions and disorders. In outpatient physical therapy, we see a wide array of common issues that can affect one’s mobility and quality of life. Our dedicated and experienced team is committed to helping you achieve optimal recovery through a results-oriented approach.
Our physical therapists in Huntington Beach treat a variety of conditions, including:
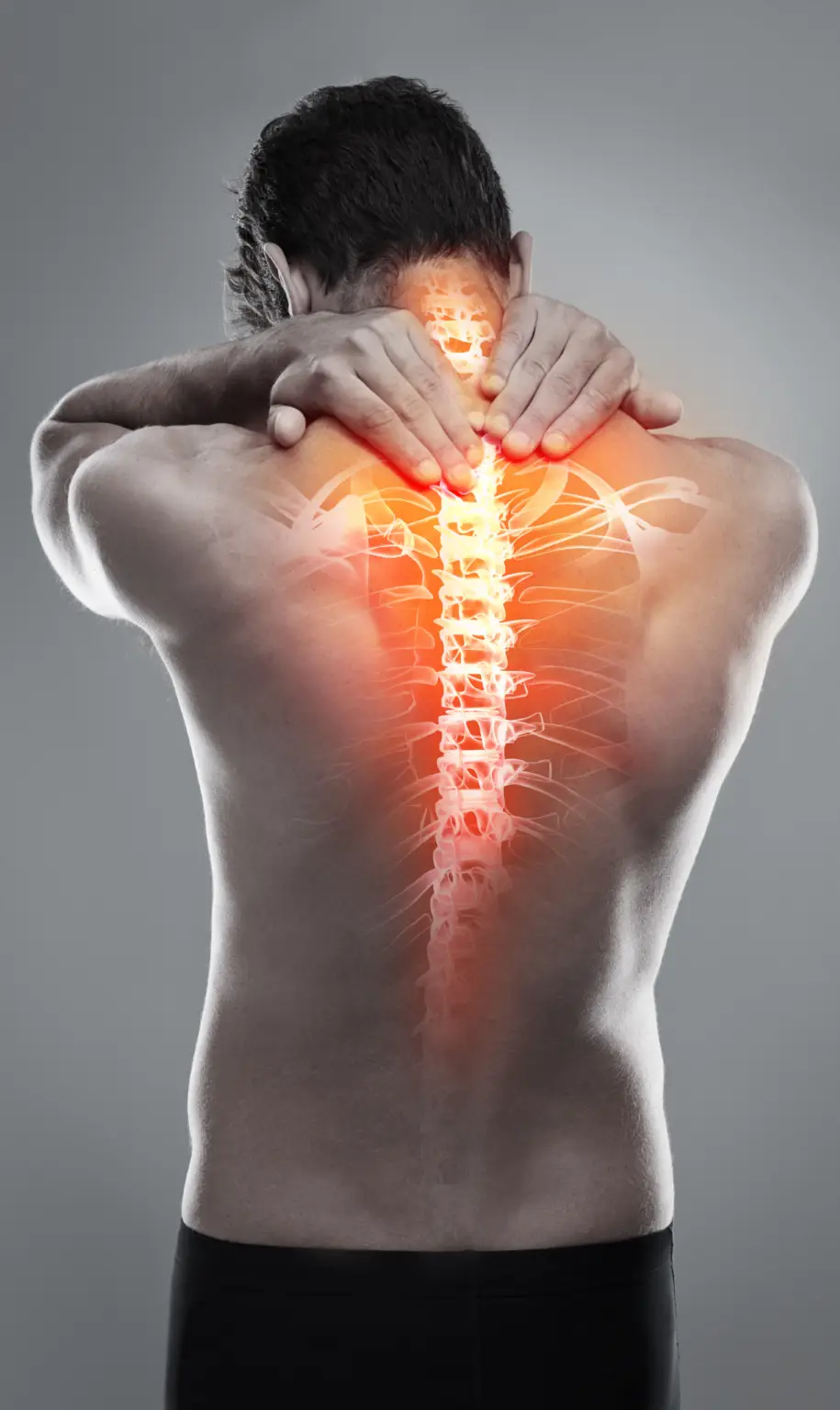
Head + Neck
The head and neck are common stress points influenced by how we carry weight, our posture, and walking habits. These factors strain the cervical spine, a delicate area prone to injuries from accidents or awkward sleeping positions. Pain here often links to the cervical vertebrae, C1-C8.
The C1 vertebra, known as the atlas, sits at the skull base, connecting to the foramen magnum, allowing the head to nod. The C2 vertebra, or the axis, features a protrusion that enables head rotation. These vertebrae facilitate full motion while protecting crucial spinal cord areas that manage breathing and bowel and bladder functions. Multiple muscle groups layered around the neck support the head and neck, ensuring mobility.
Common Ailments Treated at HB BodyLab:
Have you been experiencing pain or discomfort while yawning or eating certain foods? Perhaps you’ve dealt with jaw popping for years and have been diagnosed with temporomandibular joint (TMJ) disorder. You’re not alone. Up to 10 million Americans are affected by TMJ disorder.
In this guide, we’ll cover everything you need to know about TMJ disorder and how to find relief.
What is TMJ? The temporomandibular joint (TMJ) connects your lower jaw to your skull, enabling you to open and close your mouth, eat, and speak. TMJ disorder refers to pain and compromised movement in this joint and the surrounding muscles.
What Causes TMJ? The exact cause of TMJ disorder is often unknown, but several factors can contribute, including:
- Trauma to the jaw joint
- Arthritis
- Habitual grinding or clenching of teeth
- Structural issues from birth
- Genetics
Diagnosing TMJ disorder can be challenging, as there is no definitive test. However, doctors consider various factors to determine its presence.
TMJ Symptoms Symptoms of TMJ disorder vary in severity and cause. Common symptoms include:
- Jaw pain and muscle stiffness
- Limited jaw movement
- Jaw locking
- Clicking or popping sounds when opening and closing the mouth
- Misalignment of the teeth (malocclusion)
- Ear pain or aching
- Difficulty or pain while chewing
- Facial pain
Facial pain can indicate various conditions, so it’s important to consult your doctor to rule out other issues like sinus infections or facial neuralgias.
For those suffering from TMJ disorder, HB BodyLab offers comprehensive treatment plans to alleviate pain and improve jaw function.
Have you been experiencing pain or discomfort while yawning or eating certain foods? Perhaps you’ve dealt with jaw popping for years and have been diagnosed with temporomandibular joint (TMJ) disorder. You’re not alone. Up to 10 million Americans are affected by TMJ disorder.
In this guide, we’ll cover everything you need to know about TMJ disorder and how to find relief.
What is TMJ? The temporomandibular joint (TMJ) connects your lower jaw to your skull, enabling you to open and close your mouth, eat, and speak. TMJ disorder refers to pain and compromised movement in this joint and the surrounding muscles.
What Causes TMJ? The exact cause of TMJ disorder is often unknown, but several factors can contribute, including:
- Trauma to the jaw joint
- Arthritis
- Habitual grinding or clenching of teeth
- Structural issues from birth
- Genetics
Diagnosing TMJ disorder can be challenging, as there is no definitive test. However, doctors consider various factors to determine its presence.
TMJ Symptoms Symptoms of TMJ disorder vary in severity and cause. Common symptoms include:
- Jaw pain and muscle stiffness
- Limited jaw movement
- Jaw locking
- Clicking or popping sounds when opening and closing the mouth
- Misalignment of the teeth (malocclusion)
- Ear pain or aching
- Difficulty or pain while chewing
- Facial pain
Facial pain can indicate various conditions, so it’s important to consult your doctor to rule out other issues like sinus infections or facial neuralgias.
For those suffering from TMJ disorder, HB BodyLab offers comprehensive treatment plans to alleviate pain and improve jaw function.
Are you feeling dizzy? Maybe the room is spinning, or perhaps you feel like you are. You can’t focus and just want to lie down. It’s enough to make you feel miserable.
Vertigo can be challenging to manage, but it doesn’t have to be a regular part of your life. Let us help you understand the condition and how to cope with and overcome vertigo symptoms.
What is Vertigo? Vertigo attacks can occur suddenly and last from a few seconds to several days. It leaves you feeling dizzy and off-balance and comes in two main forms:
- Peripheral Vertigo: Issues with the inner ear.
- Central Vertigo: Problems in the brain, such as infections, tumors, brain injuries, or strokes.
Causes of Vertigo Vertigo can be caused by various factors, including:
- Toxin Exposure: Alcohol and some drugs can affect the vestibular system.
- Benign Paroxysmal Positional Vertigo (BPPV): Sudden head movements trigger spinning or dizziness.
- Meniere’s Disease: Fluid buildup in the inner ear causing vertigo, tinnitus, ear fullness, and hearing loss.
- Labyrinthitis: Inflammation of the inner ear labyrinth leading to headaches, dizziness, and trouble focusing.
- Migraines: Vestibular migraines can cause vertigo, poor balance, disorientation, and speech challenges.
- Brain Injury or Trauma: Injuries affecting the vestibular or central nervous systems, such as concussions or strokes.
Symptoms of Vertigo Vertigo symptoms can vary but often include:
- Dizziness: The most common symptom, ranging from mild to severe.
- Nausea: Caused by the imbalance and spinning sensation.
- Vomiting: Persistent dizziness can lead to motion sickness and vomiting.
- Headaches: Often accompanied by dizziness and may worsen with ear fullness or eye focus issues.
At HB BodyLab, we offer comprehensive treatment plans to help manage and alleviate vertigo symptoms, improving your quality of life.
Thoracic outlet syndrome (TOS) can significantly impact your life, causing pain, numbness, tingling, and discoloration in your arms and hands. Fortunately, TOS is treatable, and you don’t have to endure these symptoms forever. This guide will explain how physical therapy exercises for thoracic outlet syndrome can reduce your symptoms and improve your quality of life.
What is Thoracic Outlet Syndrome? Thoracic outlet syndrome occurs when the nerves, veins, or arteries in the neck and chest area are compressed. This compression leads to the symptoms you’re experiencing. TOS encompasses three disorders:
- Neurogenic thoracic outlet syndrome (nerve compression)
- Venous thoracic outlet syndrome (vein compression)
- Arterial thoracic outlet syndrome (artery compression)
Over 90% of TOS cases are Neurogenic, less than 6% are Venous, and Arterial TOS is the least common, affecting only 1% of patients.
What Causes Thoracic Outlet Syndrome? Thoracic outlet syndrome can affect anyone and has several potential causes, including:
- Physical Injury or Trauma: Auto accidents, especially those causing whiplash, can lead to TOS.
- Repetitive Movement: Activities like typing, swimming, pitching, stocking shelves, or assembly line work can cause TOS due to repetitive arm movements.
- Poor Posture: Improper alignment while sitting at a desk can compress nerves and lead to TOS.
- Anatomical Abnormality: Some individuals have an extra rib (cervical rib) that can cause nerve compression.
Thoracic Outlet Syndrome Symptoms Symptoms vary depending on the type of TOS and can range from mild to severe. Common symptoms include:
- Paresthesia in Extremities: Numbness or tingling in your hands and arms.
- Pain and Weakness: Discomfort and reduced strength in the arm, difficulty moving the arm, or turning the head.
- Occipital Headaches: Headaches stemming from nerve pain in the neck and back of the head.
Paresthesia in Extremities This “pins and needles” sensation results from prolonged pressure on nerves, leading to numbness or tingling in the arms and hands. Proper treatment can significantly reduce or eliminate these sensations.
Pain and Weakness Compression of nerves, veins, or arteries can cause pain and limit movement, making it difficult or painful to move your arm or turn your head. Patients often report pain in the back of the head, neck, and shoulders.
Occipital Headaches These headaches are caused by pain in the occipital nerves, which run from the neck up the back of the head. Occipital headaches due to TOS can be debilitating and last for hours.
At HB BodyLab, we offer comprehensive treatment plans for thoracic outlet syndrome to help you manage and overcome these symptoms, enhancing your overall quality of life.
Are you experiencing neck pain, headaches, and muscle spasms in your neck and back? Searching for relief from neck arthritis discomfort? You’re not alone.
Neck arthritis, or cervical spondylosis, is one of the most common forms of arthritis among adults. Many people are looking for ways to find relief, just like you.
In this guide, we’ll review the causes and symptoms of neck arthritis and share common treatment options and exercises to help you find relief.
What Is Neck Arthritis? More than 85% of people over 60 experience neck arthritis, also known as cervical spondylosis. It affects the spinal discs in your neck, where cartilage breaks down over time, often causing no symptoms initially. Like other forms of arthritis, neck arthritis is the age-related degeneration of bones, joints, and discs in your neck.
What Causes Neck Arthritis? The human head weighs about as much as a ten-pound bowling ball, causing stress on the neck’s discs and joints. This wear and tear occur in almost everyone, even without symptoms. Nearly half of all middle-aged and older people have worn discs and joints without any painful symptoms. Here’s how it happens:
- Dehydrated Discs: By age 40, most people’s spinal discs start drying out and shrinking, causing more bone-to-bone contact between vertebrae and thickening of bones and ligaments.
- Herniated Discs: Cracks in the spinal discs allow the soft interior to slip through, often due to occupation, hobby, or genetics.
- Bone Spurs: As discs break down, the body may produce extra bone (bone spurs) to strengthen the spine, which can pinch the spinal cord and nerve roots.
- Stiff Ligaments: Age or genetics can cause spinal ligaments to stiffen, reducing neck flexibility.
Neck Arthritis Symptoms Neck arthritis can be symptomatic or asymptomatic. Common symptoms include:
- Neck stiffness
- Pain in the shoulder or arms
- Neck pain
- Headaches starting in the neck
- Trouble sleeping
- Irritability
- Fatigue
- Myelopathy
- Numbness in the arm or hand
- Limited head or neck movement
- Radiculopathy
- Grinding noise or sensation when turning the neck
When cervical spondylosis leads to myelopathy, additional symptoms may include:
- Lack of coordination
- Difficulty walking
- Muscle spasms
- Loss of bowel and bladder control
- Abnormal reflexes
- Tingling, numbness, or weakness in the arms, hands, legs, or feet
Dealing with neck arthritis symptoms can be frustrating and, in severe cases, debilitating. Fortunately, several treatment options are available to help manage these symptoms and improve your quality of life.
Receiving a Parkinson’s disease diagnosis can be daunting. You might feel frustrated with your symptoms and worry about losing your abilities. Fortunately, various treatment options can significantly improve Parkinson’s symptoms.
In this guide, we’ll explore the signs and symptoms of Parkinson’s disease and discuss the available treatment options.
What is Parkinson’s Disease? Parkinson’s disease is a progressive neurodegenerative disorder that affects movement. It results from the gradual breakdown or death of dopamine-producing neurons, leading to abnormal brain activity and Parkinson’s symptoms.
Early symptoms of Parkinson’s often include:
- Reduced or loss of facial expressions
- Soft or slurred speech
- Stiffness or slow movement
- A slight tremor in one hand
As the disease progresses, it gradually affects the entire body. Parkinson’s is the second most common neurodegenerative disorder in adults in America.
Causes of Parkinson’s Disease The exact cause of Parkinson’s is unknown, but several factors may contribute:
- Genetics: Specific gene mutations are linked to Parkinson’s, though these are rare except in families with multiple affected members.
- Environmental Factors: Exposure to certain toxins or environmental factors can slightly increase the risk.
- Lewy Bodies: Clumps of specific substances in brain cells, known as Lewy bodies, are markers for Parkinson’s and may help identify its cause in the future.
Risk Factors for Parkinson’s Disease Several factors can increase your risk of developing Parkinson’s:
- Age: Advanced age is a significant risk factor, with most cases occurring in individuals 60 or older.
- Heredity: Having a close relative with Parkinson’s can increase your risk, though this is generally low unless many family members are affected.
- Gender: Males are more likely to develop Parkinson’s than females.
- Exposure to Toxins: Continuous exposure to toxins like pesticides can raise the risk.
Symptoms of Parkinson’s Disease Early Parkinson’s symptoms can be mild and become more noticeable as the disease progresses. Common symptoms include:
- Shaking or tremors
- Slowed movements
- Stiff muscles
- Impaired posture and balance
- Loss of unconscious movements, such as blinking or smiling
- Changes in speech, including slurring, speaking softly or quickly, or loss of inflection
- Difficulties with writing
It’s essential to discuss your symptoms with a doctor to rule out other conditions. With proper diagnosis and treatment, managing Parkinson’s disease and improving your quality of life is possible.
If you have a herniated disc in your neck, you know how painful it can be. The pain can be unbearable, affecting your neck and shoulder blade, making it difficult to turn or bend, and causing muscle spasms. If you’re seeking relief from disc herniation, you’re not alone. Many people have found relief through physical therapy and exercise.
Read on as we delve into the common causes, symptoms, and treatments for disc herniation.
What is Disc Herniation? Pain in your neck, shoulder blades, or upper back may indicate a disc herniation (also called a herniated cervical disc). This condition occurs when a spinal disc weakens and protrudes onto the spinal cord. Spinal discs are rubbery cushions between the vertebrae in your spine. The top seven vertebrae are the cervical (neck) vertebrae, which connect to nerves serving your arms, hands, and upper body. A weakened or bulging disc can result in pain, numbness, or weakness, depending on its location.
What Causes Disc Herniation? Disc herniation is often due to gradual, age-related wear and tear. As you age, your discs become less flexible and more prone to tearing or rupturing, sometimes due to minor strains or twists. Common causes include:
- Using back muscles to lift
- Twisting and turning while lifting
- Traumatic falls or impacts
- Intervertebral disc disease
Risk Factors for Disc Herniation Several factors can increase your risk of experiencing a herniated disc, including:
- Weight: Excess body weight adds stress to your discs.
- Occupation: Physically demanding jobs involving lifting, pulling, bending, and twisting.
- Genetics: A family history of herniated discs.
- Smoking: Reduces oxygen supply to the disc, causing it to deteriorate more quickly.
Disc Herniation Symptoms Herniated discs most commonly occur in the lower back but can also affect the neck, usually impacting one side of the body. Symptoms depend on the disc’s location and whether it’s pressing on a nerve. Common symptoms include:
Arm or Leg Pain If the herniated disc is in your lower back, you’ll likely feel pain in your buttocks, thigh, and calf. If it’s in your neck, the pain will be in your shoulder and arm, often described as sharp or burning.
Numbness or Tingling Radiating numbness or tingling can occur due to affected nerves serving the body part.
Weakness Affected nerves can cause muscle weakness, leading to stumbling or difficulty lifting and holding items.
Diagnosis of Disc Herniation If you have neck or back pain that radiates to your arms or legs, or if you experience numbness, tingling, or weakness, it’s time to see your doctor. A physical exam is usually sufficient for diagnosing disc herniation. Sometimes, additional tests like x-rays, CT scans, MRI, or myelograms are needed to rule out other sources of pain such as fractures or tumors.
At HB BodyLab, we offer comprehensive treatment plans to help manage and alleviate the symptoms of disc herniation, improving your quality of life.
If you’ve recently been in a car accident or suffered a neck injury and think you might have whiplash, you may feel unsure about what whiplash is, how to confirm if you have it, and what can be done to treat it. It can literally be a pain in the neck.
We understand how overwhelming it can be to find the information you need about your health and well-being, and we’re here to help. In this guide, we’ll cover essential information about whiplash, how to manage the injury, and the resources available to you. Keep reading to learn more.
What is Whiplash? Whiplash is a common neck injury that occurs when your head and neck are suddenly forced backward and then forward in a whip-like motion, overstretching the ligaments, joints, and muscles in your neck and back. This rapid movement puts extreme stress on the cervical spine. Whiplash is also known as a neck strain or whiplash-associated disorder (WAD). Symptoms vary based on which neck tissues are injured and the severity of the injury.
What Causes Whiplash? While car accidents are the most common cause, whiplash can occur anytime your head is thrust forward and backward sharply. Other causes include:
- Blows to the head
- Bicycle accidents
- Physical incidents such as assault, abuse, or shaking a baby
- Sports accidents
- Roller coaster rides
- Bungee jumping
- Horseback riding accidents
- High-impact activities where the cervical spine experiences extreme acceleration-deceleration forces
Whiplash occurs when the neck muscles and ligaments extend beyond their normal range of motion, potentially causing them to stretch or tear. Though often considered mild, whiplash can sometimes lead to long-term pain and discomfort.
Whiplash Symptoms Symptoms of whiplash may not appear immediately after an injury, so it’s important to monitor any physical changes for several days. Common symptoms include:
- Neck pain and stiffness
- Pain with neck movement
- Muscle spasms
- Reduced range of motion in the neck
- Headaches
- Trouble sleeping
- Shoulder or upper back pain
- Radiating numbness, tingling, or weakness in the shoulder, arm, hand, or fingers (cervical radiculopathy)
Less common but more severe symptoms may include:
- Vision problems
- Memory or concentration issues
- Difficulty chewing or swallowing
Whiplash-associated disorders (WAD) are often classified by severity:
- Grade 1: Neck pain, tenderness, or stiffness
- Grade 2: Neck pain, loss of range of motion, and tenderness
- Grade 3: Neck pain, loss of motion, and neurological symptoms like tingling or numbness in the arm, hand, or fingers
- Grade 4: Neck pain with dislocation or fracture
Consult your doctor if you experience any of these symptoms following a head or neck injury.
Diagnosing Whiplash If you have symptoms associated with whiplash after an injury, your doctor will likely conduct a physical exam. To rule out other potential causes of pain, your doctor may order imaging tests such as:
- MRI
- CT scan
- X-ray
These tests can help identify underlying issues, although whiplash itself may not be visible on imaging. Your exam may also include a neurological assessment to check nerve sensation and responsiveness.
Recently, you’ve noticed a small protrusion at the base of your neck when you catch a side glimpse of yourself in the mirror. You’re concerned about its appearance and wondering if it might lead to physical problems.
This condition might be dowager’s hump, also known as kyphosis.
What is dowager’s hump, and what happens if it’s left untreated? Keep reading to learn about its causes, symptoms, and the best treatment options.
What Is Dowager’s Hump? Dowager’s hump, or kyphosis, is a rounded hunch at the base of the neck where it meets the upper back. It’s an excessive curvature of the upper spine. It’s called dowager’s hump because it often affects older women with osteoporosis, but it can occur in anyone. A recent study found that 35% of healthy women aged 20 to 64 suffer from this condition.
What Causes Dowager’s Hump? Several factors can lead to dowager’s hump:
- Poor Posture: Constant slouching or hunching over can cause mild forms of the condition.
- Degenerative Disc Disease: Compressed or smaller discs in the neck can’t support the spine’s natural curve.
- Weak Muscles: Insufficiently strong back muscles fail to hold the spine properly.
- Spinal Injuries: Vertebral fractures increase the risk of kyphosis.
- Osteoporosis: Brittle bones lead to the stooped posture associated with dowager’s hump.
- Aging: The spine’s curve naturally increases with age.
- Congenital Defects: Conditions like Scheuermann’s kyphosis cause triangular-shaped vertebrae, leading to increased spinal curvature.
Symptoms of Dowager’s Hump Kyphosis can affect various body systems. Here’s how it might impact you:
Musculoskeletal Symptoms Dowager’s hump can significantly limit physical activity and bodily functions. Symptoms include:
- Postural changes
- Increased muscle fatigue
- Chronic neck, shoulder, and back pain
- Vertebral compression fractures
- Loss of height
- Protruding abdomen
- Back stiffness
- Hip pain
- Numbness in the chest area
- Poorer balance
- Slower gait
- Increased risk of falls
These symptoms can make everyday activities like walking, driving, or getting up from a chair difficult.
Digestive Symptoms As dowager’s hump progresses, it can compress the digestive tract, leading to acid reflux or difficulty swallowing.
Respiratory Symptoms Kyphosis can cause breathing difficulties due to added pressure on the lungs.
Psychological Symptoms Mild kyphosis may not be very noticeable, but as it advances, it can become disfiguring. Younger individuals with the condition may experience body image issues, leading to feelings of shame and anxiety. Seniors with dowager’s hump may feel isolated and depressed because of their appearance.
Understanding dowager’s hump is the first step towards managing it. Consult a healthcare provider for personalized advice and treatment options.

Shoulder
The shoulder is one of the most versatile parts of the body, enabling us to lift, reach, push, pull, and carry. Its wide range of motion is essential for many daily activities, but this complexity also makes the shoulder prone to injuries and pain. At HB BodyLab, we focus on educating our clients about the origins of their shoulder pain, proper shoulder mechanics, and strategies to improve their overall functionality and well-being.
Understanding shoulder pain begins with a basic knowledge of shoulder anatomy. The shoulder’s intricate design and its connection to the musculoskeletal system can often lead to discomfort and injury. We work with our clients to recognize the sources of their pain and how to address them effectively.
Common Ailments Treated at HB BodyLab:
If you’ve recently injured your acromioclavicular (AC) joint—or suspect you might have—you’re likely experiencing pain, swelling, and a loss of strength in your shoulder. You might be wondering if surgery is necessary.
Fortunately, AC joint rehabilitation typically involves physical therapy alone, often avoiding the need for surgery. The key is to get your injury diagnosed promptly once you feel pain.
In this article, we’ll cover everything you need to know about AC joint physical therapy and what to expect during your recovery.
What is AC Joint Separation? The clavicle (collarbone) and the acromion (shoulder blade) are connected by four ligaments. AC joint separation occurs when these ligaments are stressed, leading to a partial or complete separation.
These injuries range from mild to severe, depending on the level of trauma and detachment. AC joint injuries can be classified into two types:
- Traumatic: Resulting from a specific injury
- Overuse: Due to repetitive stress
Men under 35, particularly those involved in contact sports and high-risk activities, are most commonly affected by AC joint injuries.
What Causes AC Joint Separation? Shoulder pain affects about 13 million Americans annually, with 31% experiencing AC joint pain due to trauma or overuse.
Traumatic AC Joint Injury This type of injury is common in individuals who suffer a hard fall, landing on their hand or shoulder. Examples include:
- Football players tackled to the ground
- Downhill skiers taking a tumble
- Cyclists falling off their bikes
- Painters falling from ladders
Overuse AC Joint Injury Excessive and prolonged demand on the AC joint can stress the protective cartilage, leading to arthritis. This often occurs in people engaged in repetitive overhead activities, such as:
- Weightlifters
- Painters
- Manual laborers
AC Joint Separation Symptoms Symptoms of an AC joint injury may include:
- Pain and swelling
- Tenderness over the AC joint
- Loss of strength and motion in the shoulder
- A popping sound or catching sensation when moving the shoulder
- A noticeable bump on top of the shoulder
- Discomfort when lifting, reaching, or carrying objects
A physical therapist can diagnose and treat AC joint injuries. Diagnostic imaging tests like X-rays, MRIs, or ultrasounds may be needed to determine the injury’s extent. Your physical therapist will conduct various tests and ask you to demonstrate movements that cause discomfort. The examination will also include surrounding areas like the neck and back to understand their contribution to the injury.
After enduring a throbbing shoulder, struggling through your weekly tennis matches, and having countless sleepless nights, you finally have a diagnosis: a rotator cuff injury.
It sounds serious, and while surgery might be an option, your doctor recommends trying physical therapy first.
You might think physical therapy is only for serious athletes or those recovering from major surgery, but it can benefit everyone, including those with rotator cuff pain.
This article will guide you through specific rotator cuff injuries and the types of exercises you can expect during physical therapy for rotator cuff strain.
What Is the Rotator Cuff? The rotator cuff is a group of four muscles and tendons that stabilize your shoulder joint, allowing you to lift and rotate your arms. It keeps the top of the humerus bone securely in the shoulder socket.
Rotator cuff injuries are common, and the likelihood increases with age. If you have a rotator cuff injury, you’ll experience pain in your shoulder.
What Causes Rotator Cuff Pain? There are two primary causes of rotator cuff pain:
- Traumatic Shoulder Injury: Often caused by a fall directly on the shoulder or a direct blow to the area.
- Degeneration/Overuse/Repetitive Actions: Most rotator cuff tears result from wear and tear over time.
Common Rotator Cuff Injuries Rotator cuff injuries are quite prevalent. About 2 million people in the U.S. visit their doctors annually due to rotator cuff issues. Common injuries include:
- Rotator cuff strain
- Rotator cuff tear
- Tendinitis (inflammation of the shoulder tendons)
- Bursitis (inflammation of the bursae, small fluid-filled sacs cushioning the muscles and tendons near the shoulder joint)
Rotator Cuff Injury Symptoms Symptoms of a rotator cuff injury can include:
- A dull ache deep in the shoulder
- Pain that disrupts sleep, especially when lying on the injured shoulder
- Difficulty raising your arms or decreased range of motion
- Arm weakness
- Problems with everyday activities such as combing your hair or fastening your bra
If you’re experiencing shoulder pain, don’t self-diagnose or wait for the pain to go away on its own. Continuing to use an injured rotator cuff can cause further damage. Seeking treatment from a medical professional is the best course of action.
Reaching to bring down a box, hanging a picture, getting dressed—these simple, everyday tasks can become inconvenient, difficult, or even impossible when you have a frozen shoulder.
The gradual onset of immobility in the arm and shoulder can be frustrating and alarming, especially when undiagnosed. While a frozen shoulder will eventually heal on its own, this process can take up to three years, leaving you to deal with pain and stiffness in the meantime.
If waiting that long sounds unbearable, read on to learn how you can alleviate your pain and speed up recovery from a frozen shoulder.
What is Frozen Shoulder? Frozen shoulder, also known as adhesive capsulitis, is a common disorder that causes pain, stiffness, and a loss of normal range of motion in the shoulder. Your shoulder consists of three bones that form a ball-and-socket joint:
- Humerus (upper arm)
- Scapula (shoulder blade)
- Clavicle (collarbone)
These bones are surrounded by tissue called the shoulder capsule, which holds everything together. In a frozen shoulder, this capsule becomes so thick and tight that movement is restricted. The condition can be seriously debilitating and often worsens over time if left untreated.
What Causes Frozen Shoulder? The exact cause of frozen shoulder is unknown, but certain groups are more at risk. You’re more likely to develop frozen shoulder if you’re:
- Between the ages of 40 and 60
- A woman (it occurs more often in women)
- Recovering from a stroke, broken arm, or surgery that limits arm movement (e.g., mastectomy, rotator cuff surgery)
- Diabetic
- Living with Parkinson’s disease
Experts believe frozen shoulder develops when the joint becomes inflamed and scar tissue forms, causing the tissue inside the joint to shrink and harden, which restricts movement.
Frozen Shoulder Symptoms Frozen shoulder typically develops slowly in three stages, each lasting several months.
Freezing Stage In this stage, any shoulder movement causes pain, sometimes severe. The pain worsens over time and may be more noticeable at night. The shoulder gradually loses its range of motion. This stage can last 2-9 months.
Frozen Stage During this stage, pain may decrease, but stiffness increases, making everyday activities very challenging. This stage can last 4-12 months.
Thawing Stage In the thawing stage, the shoulder and arm slowly regain their range of motion over a period of 5-26 months. While it’s a slow process, strength and mobility gradually return to normal or near-normal levels.
Once a frozen shoulder heals, it rarely returns in the same shoulder, but it can sometimes occur in the opposite shoulder.
Understanding frozen shoulder and its stages can help you seek appropriate treatment to alleviate symptoms and accelerate recovery.
Your life has been consumed with shoulder pain and discomfort.
After being diagnosed with shoulder bursitis, you’re seeking ways to manage the symptoms.
At HB BodyLab, we understand how life-altering daily pain can be. No one should have to give up the activities they love due to an injury.
In this guide, we’ll provide everything you need to know about shoulder bursitis, including its causes, treatments, and how physical therapy can help.
What is Shoulder Bursitis? Shoulder bursitis is a painful inflammation and swelling of the shoulder joint, where the bursae become inflamed and irritated. Bursae are small fluid-filled sacs that cushion the joints, preventing bones, tendons, and muscles from rubbing together. When these bursae become inflamed, they thicken, leaving little room for shoulder movement. Shoulder bursitis is the most common cause of shoulder pain in adults. The subacromial bursa, located below the shoulder blade, is particularly susceptible to bursitis.
What Causes Shoulder Bursitis? Shoulder bursitis is usually caused by excessive pressure or stress on the bursa, often triggered by repetitive movements. It is categorized into three types:
- Chronic Bursitis: Develops over time due to repetitive irritation. It may have no known cause but can occur due to pre-existing conditions like gout, pseudogout, diabetes, or uremia.
- Infected Bursitis: Also known as septic bursitis, it occurs when bacteria infect the bursa through a puncture, cut, or insect bite. This serious condition requires immediate medical attention.
- Traumatic Bursitis: The least common type, typically found in athletes, caused by repetitive rubbing or excessive bending of a joint. People who frequently use their shoulders in overhead motions, such as baseball players, carpenters, and musicians, are more prone to this type of bursitis.
Shoulder Bursitis Symptoms Symptoms of shoulder bursitis vary but commonly include:
- Localized pain
- Tenderness
- Pain with movement of affected tissues
- Redness around the shoulder
- Sensitivity to pressure near the affected tissues
- Swelling (rare)
- Fever (associated with infected bursitis)
If you experience shoulder pain, don’t ignore it. Consult with a medical professional to properly diagnose and treat shoulder bursitis. Physical therapy can be an effective way to manage symptoms and improve your quality of life.
The shoulder is the most mobile joint in the body and, unfortunately, also the most prone to dislocation.
Whether you’re a contact sports athlete or have suffered a bad fall, you may have had your shoulder reset by a doctor and now wonder, “Will this happen again?”
If you’ve experienced a shoulder dislocation, physical therapy can help rehabilitate your shoulder and prevent reinjury.
Here’s everything you need to know about shoulder dislocation, its treatment, and how to prevent it from happening again.
What is Shoulder Dislocation? Shoulder dislocation can occur during aggressive contact sports or even from an awkward fall, depending on how loose the shoulder is. The humerus (upper arm bone) fits into the scapula (shoulder blade) like a ball in a socket, but when forced out of its normal range of motion, it can pop out of place. However, it’s not always as simple as “popping it back in.” A dislocated shoulder can damage surrounding structures such as:
- Bones
- Ligaments
- Muscles
- Tendons
- Cartilage
If you suspect a shoulder dislocation, seek immediate medical attention.
What Causes Shoulder Dislocation? Shoulder dislocation is a common trauma that can happen to anyone. Common causes include:
Contact Sports Athletes in contact sports like hockey or football are at higher risk due to traumatic impacts. Gymnasts, cheerleaders, and other athletes involved in falls are also high-risk.
Accidents Traffic accidents can dislocate the shoulder by pushing the humerus out of the socket. Work-related accidents, especially in labor-intensive or physically dangerous jobs, can also cause dislocations.
Falls A dislocation can happen to anyone, particularly older individuals at risk of falling. Falling on an outstretched arm or directly on the shoulder can cause dislocation.
Shoulder Dislocation Symptoms You may feel your arm dislocate from the shoulder upon impact, but this isn’t always the case. It’s easy to ignore the pain and attribute it to bruising or soreness after a rough game or a fall. However, if you experience lasting pain, see a doctor immediately. Symptoms of a dislocated shoulder include:
- Swelling or bruising on the upper arm
- Severe shoulder pain
- Difficulty moving the arm
- Muscle spasms in the upper arm or shoulder
- An arm that appears out of place or crooked
- Numbness or tingling in the neck, arm, hand, or fingers
Shoulder dislocation can cause serious nerve or blood vessel damage. If your arm and hand feel cold or look discolored, seek immediate treatment.
Understanding the causes and symptoms of shoulder dislocation can help you seek the right treatment and prevent future injuries. Physical therapy plays a crucial role in recovery and in reducing the risk of recurrence.
Shoulder pain is a common issue for athletes, manual laborers, or anyone who performs repetitive overhead arm movements.
If you’re dealing with the pain and discomfort of shoulder impingement, you might wonder if physical therapy can help. Untreated shoulder impingement can lead to more serious conditions, but the good news is that most people can rehabilitate quickly and effectively with prompt treatment.
This article covers everything you need to know about shoulder impingement and how to treat it.
What is Shoulder Impingement? The rotator cuff is a group of muscles and tendons that attach your upper arm bone to your shoulder. It sits beneath the top of the shoulder, called the acromion. Shoulder impingement syndrome occurs when the rotator cuff rubs or catches on the acromion.
When you lift your arm, the narrowing of the space (bursa) between the rotator cuff and acromion causes pain. This pressure irritates the rotator cuff, leading to impingement.
What Causes Shoulder Impingement? Shoulder impingement is primarily caused by overuse. Repeated use of the shoulder, as seen in baseball players, weightlifters, and similar activities, can cause tendon swelling. You are at a higher risk if your activities or occupation require forceful or repetitive overhead motion. Activities that may increase your risk include:
- Swimming
- Baseball
- Weight lifting
- Moving boxes
- Painting
- Construction work
Previous shoulder injuries, an abnormally shaped acromion, or age can also increase your risk for shoulder impingement.
Shoulder Impingement Symptoms Many people experience sudden pain when lifting their arm backward or overhead. Other symptoms include:
- Constant (but mild) shoulder pain
- Weakness in the shoulder or arm
- Pain that worsens at night
- Pain radiating from the front of the shoulder to the arm
If you have these symptoms, visiting one of our physical therapists can help determine if you have shoulder impingement syndrome. Your doctor may order an X-ray to rule out other issues and possibly an MRI to ensure there isn’t a more serious rotator cuff injury.
Once diagnosed, our therapists will develop a plan to treat your shoulder quickly and effectively.
The pain and inflammation in your shoulder are becoming unbearable. You wake up stiff and sore, getting ready for the day worsens the pain, and even normal household tasks are becoming difficult.
Instead of letting shoulder arthritis control your life, you want to take control of the condition.
While there is no cure for shoulder arthritis, you’re wondering if physical therapy can help alleviate the pain.
In this guide, you’ll learn about shoulder arthritis, including:
- What shoulder arthritis is
- Its causes
- Its symptoms
- How physical therapy can help
- And more
What Is Shoulder Arthritis? Shoulder arthritis occurs when the cartilage on the ball or socket of the shoulder joint is damaged or worn. The shoulder has two joints:
- Glenohumeral joint: Regular shoulder arthritis usually refers to this joint.
- Acromioclavicular joint: When arthritis affects this joint, it’s referred to as AC joint arthritis.
In both cases, shoulder arthritis causes inflammation, pain, and stiffness, making daily tasks difficult.
What Causes Shoulder Arthritis? There are five common causes of shoulder arthritis that make natural arm movements painful and difficult:
1. Osteoarthritis Most common in people over 50, osteoarthritis is known as the “wear-and-tear” arthritis. It develops from overuse but can also be influenced by obesity, previous joint injuries, or family history. This type often affects the acromioclavicular joint and is sometimes called “bone on bone” arthritis.
2. Rheumatoid Arthritis Rheumatoid arthritis (RA) is a chronic autoimmune disease where the body’s defenses mistakenly damage normal tissue. RA can affect many joints, including both shoulder joints, causing swelling, stiffness, and pain. It can develop at any age and some people are more susceptible than others.
3. Post-Traumatic Arthritis This type of arthritis develops quickly after a shoulder injury. Unlike other forms, post-traumatic arthritis is usually temporary and can heal over time.
4. Rotator Cuff Tear Arthropathy Nearly 2 million people in the U.S. suffer from rotator cuff tears each year, leading to shoulder pain and arthritis. A rotator cuff tear weakens the shoulder, causing the head of the shoulder to rub against the outer edge of the shoulder blade, leading to arthritis.
5. Avascular Necrosis Avascular necrosis (AVN) is a condition where the blood supply to the shoulder joint is disrupted, often due to high-dose steroid use, heavy alcohol consumption, sickle cell disease, or traumatic shoulder injuries. This can destroy the shoulder joint over time, leading to arthritis.
Shoulder Arthritis Symptoms Although the types of shoulder arthritis vary, they present similar symptoms. Some symptoms appear quickly, others over time, and some are manageable with treatment.
Pain Pain is the most common symptom of shoulder arthritis. It can vary in intensity, be aggravated by certain movements, or progressively worsen. The location of the pain can depend on the type of arthritis:
- Glenohumeral arthritis typically causes pain in the side or back of the shoulder.
- AC arthritis usually causes pain at the top of the shoulder, sometimes radiating into the neck.
- RA can cause pain throughout the entire shoulder, affecting both joints.
Limited Range of Motion As shoulder arthritis progresses, you might notice a limited range of motion, making it difficult to reach above your head or lift objects.
Crepitus Crepitus is the grinding, clicking, or snapping sound in the shoulder. It is common for joints to make sounds, but if crepitus is accompanied by pain, swelling, or limited range of motion, it may indicate shoulder arthritis.
Understanding shoulder arthritis and its symptoms can help you seek the right treatment and manage the condition effectively. Physical therapy can play a crucial role in alleviating pain and improving your shoulder function.
Whether you participate in sports like tennis, swimming, or baseball that involve repetitive motions, or your body is simply reacting to everyday movements, you may develop biceps tendonitis. This condition can cause pain in the front of the shoulder and weaken the bicep muscle.
If you’re experiencing this type of discomfort, relief may be within reach. We’ll discuss biceps tendonitis, its causes and symptoms, and how physical therapy can help.
What Is Biceps Tendonitis? Biceps tendonitis occurs when the tendons that attach the bicep to the shoulder blade (the short head tendon and the long head tendon) or the tendon that attaches the bicep muscle to the elbow become inflamed due to overuse. These tendons can develop microtears in the fibers, leading to inflammation and pain.
What Causes Biceps Tendonitis? Biceps tendonitis can occur at both the shoulder and elbow insertion points, typically due to overuse or sudden injury. The repetitive movements involved in sports like:
- Tennis
- Golf
- Swimming
- Baseball
…can cause this condition. Additionally, everyday activities that involve regular overhead motions, especially as we age and our tendons naturally weaken, can also lead to biceps tendonitis. It’s important to note that while you can experience biceps tendonitis in both the shoulder and elbow, it’s uncommon to have it in both locations simultaneously.
Biceps Tendonitis Symptoms Common symptoms of biceps tendonitis include:
- Pain in the front of the shoulder that worsens with overhead movement or lifting
- Pain in the shoulder or elbow when moving the upper arm
- Achiness or tenderness that radiates down the upper arm bone
- Weakness
- A snapping sound or sensation in the shoulder
- Pain when rotating the wrist from palm-up to palm-down
Understanding the symptoms and causes of biceps tendonitis can help you seek the right treatment. Physical therapy can be an effective way to manage and alleviate the pain, helping you regain strength and function in your shoulder and arm.

Back
Back pain is a common issue among many of our clients who seek physical therapy and personal training at HB BodyLab. The back is a complex structure composed of vertebrae, cushioned by discs, threaded with nerves, and supported by ligaments and muscles. Considering the spine’s crucial role, it’s no wonder back pain is a frequent concern. At HB BodyLab, we emphasize the importance of understanding your body. By providing detailed information about the back and related pain, we aim to help you listen to your body and use it effectively for optimal health. Educating yourself on body mechanics is essential for achieving wellness.
Our expert team is dedicated to offering personalized care and treatment plans tailored to each individual’s needs, ensuring a comprehensive approach to back pain management. Whether you’re dealing with chronic discomfort or a recent injury, we are here to support you on your journey to recovery and improved health.
Common Ailments Treated at HB BodyLab:
Is sharp pain shooting down your leg throughout the day? Wondering what could be causing it?
You’re not alone.
Nearly 40% of people will experience sciatica at some point in their lifetime.
The good news is that there are ways to find relief from sciatic pain.
In this post, we’ll discuss sciatica, its causes and symptoms, and exercises to help alleviate the pain and discomfort. Keep reading to learn more.
What is Sciatica? Sciatica is often considered a symptom rather than a diagnosis. The sciatic nerve, the longest nerve in the body, starts in the lower back, splits, and runs through your hips, buttocks, legs, and feet. Sciatica refers to pain that radiates along the path of the sciatic nerve, which can extend from your lower back down one or both legs.
What Causes Sciatica? 90% of sciatica cases are caused by a herniated (or slipped) disc with nerve root compression. Other causes include:
- Spinal Stenosis: Narrowing of the spine that compresses part of the sciatic nerve
- Bone Spurs: Often a result of osteoarthritis
- Cauda Equina Syndrome: A rare disorder affecting the nerve roots in the lumbar spine
- Spondylolisthesis: When a spinal disc slips forward over the vertebra below it
- Spinal Tumors: Tumors compressing the root of the sciatic nerve
- Infections
- Degenerative Disc Disease
- Broken Bones: Such as the pelvis or thighbone
- Pregnancy: Can cause ligament loosening, spine instability, and added pressure from the baby’s weight or position
Sciatica is more common in people who:
- Are overweight
- Suffer from acute back pain
- Live a sedentary lifestyle
- Are over 40 years old
Sciatica Symptoms Symptoms of sciatica typically occur in the lower back, hip, leg, and feet. Common symptoms include:
- Numbness
- Pain
- Tingling
- Burning
In severe cases, especially with Cauda Equina Syndrome, loss of bowel control may occur. Sciatica pain can be constant or intermittent, often described as an electric shock through the affected area. The pain can range from mild to severe, with some people experiencing excruciating pain while moving when symptoms occur.
Understanding the causes and symptoms of sciatica can help you seek the right treatment and manage the condition effectively. Physical therapy and specific exercises can play a crucial role in alleviating pain and improving your quality of life.
If you’ve recently been diagnosed with spinal stenosis, you might be wondering about your therapy and recovery options, especially if you’re experiencing pain or muscle weakness.
Not everyone with spinal stenosis will have symptoms, but if you do, you might think surgery is your only option.
We have good news. Most patients who undergo physical therapy for stenosis recover well and can lead active, pain-free lives.
This article will cover everything you need to know about physical therapy for spinal stenosis and how it can help you.
What is Stenosis? Spinal stenosis, most common in the lower back or neck, is a narrowing of the spaces in your spine. This narrowing puts pressure on the nerves traveling through the spine, leading to symptoms such as:
- Pain
- Numbness
- Tingling
The two most common types of stenosis are:
- Cervical stenosis
- Lumbar stenosis
Osteoarthritis can cause wear-and-tear changes to the spine, which can also lead to stenosis.
What Causes Stenosis? The spinal cord is protected by the vertebrae, which run from your lower back to your neck. While some people are born with a small spinal canal, spinal stenosis occurs when the open spaces in the spine narrow due to various reasons.
Common causes of spinal stenosis include:
Spinal Injuries Trauma, such as from a car accident, can cause fractures or dislocations of vertebrae, damaging the spinal canal.
Overgrowth of Bones Bone spurs from osteoarthritis can grow into the spinal cord, or in conditions like Paget’s disease, bone overgrowth can compress nerves.
Herniated Discs As the soft discs cushioning the spine dry out with age, their hard exterior may crack, allowing the inner material to escape and press on the spinal canal.
Tumors Although rare, abnormal growths can develop inside the spinal cord, in the space between the spinal cord and the vertebrae, or within the membranes covering the spinal cord.
Thickened Ligaments Hypertrophy occurs when the ligaments holding the spinal bones in place thicken. Over time, they can bulge into the spinal canal and cause nerve-related pain.
Stenosis Symptoms Even if spinal stenosis is detected on a CT scan or MRI, not everyone will experience symptoms. However, symptoms can gradually worsen and vary depending on the location of the stenosis.
Cervical Spine (Neck) Symptoms of cervical stenosis include:
- Neck pain
- Balance issues
- Weakness in a hand, foot, arm, or leg
- Tingling or numbness in a hand, foot, arm, or leg
Lumbar Spine (Lower Back) Symptoms of lumbar stenosis include:
- Back pain
- Weakness in a foot or leg
- Tingling or numbness in a foot or leg
- Painful cramping in the legs when standing or sitting
Understanding spinal stenosis and its symptoms can help you explore non-surgical treatment options, such as physical therapy, to manage and alleviate pain effectively.
You’ve been diagnosed with scoliosis. Back pain, leg weakness, and lack of flexibility are just a few of the daily challenges you face.
Dealing with the discomforts of scoliosis can be exhausting and life-altering in a negative way. But how can you manage scoliosis effectively?
Physical therapy is a valuable option for scoliosis management, offering relief to countless individuals. We hope this guide helps you understand scoliosis better and find ways to alleviate your symptoms.
When you think of scoliosis, you might recall the spine checks from elementary and middle school PE classes. While scoliosis is most commonly diagnosed in adolescents, especially girls, adults can also suffer from it or be diagnosed later in life.
The Mayo Clinic defines scoliosis as a sideways curvature of the spine, typically occurring during the growth spurt before puberty. This abnormal lateral curvature can be noticeable in some cases, while in others, it might not be visible at all.
What Causes Scoliosis? For about 80% of cases, the cause is idiopathic, meaning it’s undefined. However, scoliosis can also result from conditions like:
- Cerebral palsy
- Muscular dystrophy
- Birth defects
- Tumors
- Infections
- Genetic conditions (such as Down syndrome and Marfan syndrome)
Doctors classify scoliosis into two main types:
- Structural Scoliosis: A rigid sideways curve of the spine that cannot be reversed. This type is most common in children and adolescents and can progress with growth, leading to pain, poor posture, and difficulty with physical activities. It is considered permanent without treatment.
- Nonstructural Scoliosis (Functional Scoliosis): The spine works normally but appears curved, often due to underlying conditions like neuromuscular disorders, leg length discrepancy, postural habits, muscle spasms, or inflammation. Treating these underlying issues often resolves the scoliosis.
Scoliosis Symptoms Symptoms of scoliosis vary depending on the severity of the curve. Common symptoms include:
- Back pain
- A rotating spine
- Breathing difficulties
- One shoulder blade higher or more protruding than the other
While most cases are mild, some can become severe and disabling as children grow.
Diagnosing Scoliosis Scoliosis is typically diagnosed through a physical examination, where a healthcare provider looks for signs like spinal curves, uneven shoulders or hips, and rib humps. They may also ask you to perform certain movements to check flexibility and range of motion.
Diagnostic imaging, such as X-rays, MRIs, CT scans, and bone scans, can also be used to measure the degree of the curve and identify the type of scoliosis. These tests provide different insights:
- X-ray: Creates an image of the spine.
- MRI scan: Provides detailed pictures of bones and tissues.
- CT scan: Offers a 3-D image of the body.
- Bone scan: Highlights spinal abnormalities.
A combination of physical examinations and imaging tests helps to diagnose scoliosis accurately and determine the best treatment plan.
By understanding scoliosis and its symptoms, you can take the right steps to manage the condition effectively. Physical therapy can play a crucial role in alleviating pain and improving your quality of life.
Every year, nearly 65 million Americans experience back pain. It is not only one of the most commonly reported physical complaints but also a leading cause of lost workdays.
If you’re among those suffering from back pain, you may be searching for relief.
Physical therapy for back pain can:
- Improve mobility
- Increase strength
- Eliminate back pain
What is Back Pain? Back pain encompasses acute or chronic pain and discomfort in any part of the back, including:
- Lower back
- Middle back
- Upper back
- Back muscles
- Nerves
- Arthritis
- Disc pain
If your back pain isn’t alleviated by hot and cold therapy or over-the-counter medications, it may be time to see a Doctor of Physical Therapy for treatment.
What Causes Back Pain? Back pain can result from various causes, including:
- Sports injuries
- Accidents
- Bad habits
- Muscle strains
- Degenerative diseases
Whether chronic or acute, back pain may require an examination by a physical therapist, who might order additional tests such as an MRI or X-rays to determine the cause and appropriate treatment.
Back Pain Symptoms Back pain can lead to reduced mobility, flexibility, and function, potentially resulting in further complications. It’s important to book an appointment with your doctor or physical therapist to determine the cause of your pain.
Symptoms can range from mild to severe, depending on the underlying cause. Common symptoms include:
- Stiffness or aching along the spine
- Chronic aching in the lower or mid-back
- Pain radiating from the lower back down the back of the thigh and calf
- Sharp pains in the back or neck from lifting heavy objects
- Muscle spasms in the lower back from prolonged standing
Seek immediate medical attention if:
- Pain increases when bending at the waist or coughing
- You feel numbness in your groin, legs, or arms
- You experience burning, frequent urination, or loss of bladder control
- You have a fever
Understanding back pain and its symptoms can help you take the right steps to manage the condition effectively. Physical therapy can be an essential part of your treatment plan, helping you regain mobility and live pain-free.
You can’t move like you used to. The pain in your back has gone from uncomfortable to debilitating. Perhaps you’re also dealing with tingling and numbness in your arms and legs, wishing for relief.
Starting each day shouldn’t be this hard. Is your stiff back keeping you from activities you love?
Physical therapy and fitness coaching can help you regain motion and manage the symptoms of back arthritis. Keep reading to discover how physical therapy for back arthritis can help you return to enjoying life.
Contents:
- What Is Back Arthritis?
- Causes of Back Arthritis
- Back Arthritis Symptoms
- Treatment Methods for Back Arthritis
- Can Physical Therapy Help Arthritis in the Back?
- Top Physical Therapy Exercises for Back Arthritis
- How HB BodyLab Can Help You
What is Back Arthritis? Arthritis can affect any joint, causing inflammation (osteoarthritis) or degeneration (rheumatoid arthritis). When it affects the spine, it’s called spinal osteoarthritis. More than 45% of people will experience back arthritis in their lifetime. While arthritis can’t be reversed, treatment can improve your symptoms.
Causes of Back Arthritis
- Aging Process: As you age, the synovial fluid that lubricates your joints can become inflamed, causing stiffness. Repetitive use of joints over the years also contributes to arthritis.
- Injury or Trauma: Injuries from sports or accidents can create scar tissue, leading to arthritis over time.
- Degenerative Diseases: Conditions like rheumatoid arthritis, diabetes, degenerative disc disease, and autoimmune disorders can increase the risk of developing arthritis.
Back Arthritis Symptoms Back arthritis typically affects the lower back (lumbar region) and can cause:
- Back pain
- Stiffness
- Loss of range of motion
- Swelling around the affected vertebrae
- Tenderness
- Weakness or fatigue
- Nerve pain or numbness
Back Pain and Stiffness Back pain and stiffness are common symptoms. Stiffness can hinder activities like gardening or getting dressed. Physical therapy exercises can increase flexibility and range of motion, reducing pain and improving function.
Swelling and Tenderness Swelling and tenderness around the arthritic vertebrae, though less common, can cause significant discomfort. Inflammation can lead to swelling, putting pressure on the spine and causing tenderness.
Nerve Pain or Numbness Arthritis can lead to bone spurs that press on spinal nerves, causing pain, tingling, and numbness. These sensations can interfere with basic activities like bending or reaching.
Physical therapy offers targeted exercises that strengthen muscles and relieve joint pressure, helping you manage symptoms and improve your quality of life.
Experiencing a pinched nerve can be highly uncomfortable, causing shooting pain and significant discomfort. Radiculopathy, the medical term for this condition, can affect any part of your spinal cord, making it difficult to manage daily activities.
Being diagnosed with radiculopathy can be overwhelming, but there are many ways to manage and alleviate the symptoms.
This guide covers the causes, symptoms, treatments, and how physical therapy can help with radiculopathy.
What is Radiculopathy? Radiculopathy refers to the irritation or compression of nerve roots in the spinal cord. There are three main types:
- Cervical Radiculopathy: Affects the neck, shoulders, and upper back.
- Thoracic Radiculopathy: Occurs in the upper and middle back.
- Lumbar Radiculopathy: Affects the lower back.
What Causes Radiculopathy? Radiculopathy is caused by changes in the tissues surrounding the nerve roots, leading to compression, inflammation, or injury. Common causes include:
- Herniated spinal discs
- Bone spurs
- Ossification of spinal ligaments
- Trauma (common in patients under 50)
- Aging-related arthritis or bone degeneration
Radiculopathy most frequently occurs in the neck or lower back.
Radiculopathy Symptoms To diagnose radiculopathy, your doctor will likely start with a physical exam, followed by imaging tests such as X-rays or MRIs to assess bone alignment and scan affected areas.
Symptoms vary depending on the type of radiculopathy and can affect the neck, back, arms, or shoulders.
Cervical Radiculopathy Symptoms Symptoms typically start in the neck and radiate down the arm, including:
- Sharp or burning pain in the neck, arm, chest, and upper back
- Numbness or loss of sensation in the hands and fingers
- Pain that worsens with neck movement
Thoracic Radiculopathy Symptoms Thoracic radiculopathy is rare and affects the upper/mid-back. Symptoms include:
- Burning or shooting pain in the ribs, abdomen, and middle back
- Band-like chest pain
- Pain or tingling radiating from the middle back to the chest
- Muscle weakness or stiffness in the legs
Lumbar Radiculopathy Symptoms Lumbar radiculopathy symptoms are primarily felt in the leg and foot, such as:
- Sharp pain starting in the back and shooting down to the foot
- Pain while sitting or coughing
- Numbness or tingling in the back and legs
- Weakness in the buttocks or legs
In severe cases, lumbar radiculopathy can lead to poor coordination, difficulty walking, and even paralysis. Sciatica is another term for lumbar radiculopathy, and physical therapy is known to help alleviate sciatic nerve pain.
Treating Radiculopathy Managing radiculopathy often involves a combination of treatments, including physical therapy, medications, and lifestyle adjustments. Physical therapy plays a crucial role in reducing pain, improving mobility, and preventing further nerve compression.
Living with back pain is challenging, and you’ve endured it for too long. You suspect your SI joint might be the issue and want to understand more about this condition and how to relieve your symptoms.
We’ve got you covered.
In this guide, we’ll provide comprehensive information about the SI joint, its associated pain, exercises, and more to help you return to a pain-free life.
What Is the SI Joint? The sacroiliac (SI) joint connects your spine to your pelvis. It’s formed by the sacrum (the bone above your tailbone) and the ilium (the upper part of your pelvis).
Located on both sides of your lower back, these joints support your body weight and absorb shock during activities like walking, running, and lifting. For many, the SI joint is the primary source of lower back pain.
What Causes SI Joint Pain? The SI joint is responsible for symptoms in 15-30% of people with back pain. Pain can radiate from your hips and pelvis to your lower back and legs. When the ligaments of the SI joint become too tight or too loose, it can result in discomfort. Other causes include:
- Arthritis (ankylosing spondylitis, osteoarthritis)
- Sacroiliitis (inflammation of the SI joint)
- Pregnancy or childbirth
- Trauma to the lower back, hips, or buttocks
- Infection of the SI joint
- Urinary tract infections
- Endocarditis (inflammation of the heart’s inner layers)
- Abnormal gait
- Previous lumbar spine surgery
SI Joint Pain Symptoms Symptoms of SI joint pain vary in intensity but commonly include:
- Sharp pain in the lower back, buttocks, hips, pelvis, or groin
- Pain on one side of the body
- Increased pain when standing up
- Burning sensation in the pelvis
- Numbness or tingling in the lower back, buttocks, hips, pelvis, or groin
- Pain radiating down the thighs
If you experience a fever, pain on both sides of the lower back and buttocks, deep thigh pain, and difficulty walking, contact your physician. These could be signs of an SI joint infection, which requires prompt treatment.
It’s crucial to be assessed by a medical professional because SI joint pain symptoms can mimic other back injuries. Proper diagnosis ensures you receive the correct treatment for the underlying cause of your symptoms.
By understanding the SI joint and its related issues, you can take steps towards effective treatment and recovery.
Facet arthropathy can be both painful and debilitating.
Fortunately, there are treatments available that can help alleviate your symptoms, including physical therapy.
In this guide, we’ll explore the treatment options for facet arthropathy and how physical therapy can enhance your quality of life.
What is Facet Arthropathy? The spine consists of three types of joints per vertebra:
- An intervertebral disc joint connecting the vertebral bodies.
- Two facet joints on either side of the vertebrae that connect adjacent vertebrae.
Facet joints provide stability and mobility to the spine and limit excessive movements that could damage the spine.
Facet arthropathy occurs when arthritis affects these joints. It can happen anywhere along the spine but is most common in the lumbar region, affecting about 37% of cases.
What Causes Facet Arthropathy? Facet joints, like other joints in the body, are susceptible to wear and tear, degeneration, and arthritic changes. This can result in pain, reduced range of motion, and pinched nerves.
Common causes of facet arthropathy include:
- Joint degeneration from wear and tear or aging
- Disc degeneration
- Compression of the facet joints from spinal extension
- Traumatic injuries
- Stress injuries
- Poor posture
- Muscle weakness
- Sedentary lifestyle
Facet Arthropathy Symptoms Symptoms of facet arthropathy can range from mild to severe and may mimic other conditions like disc injuries. Common symptoms include:
- Neck pain radiating to the shoulder or arms
- Localized pain and tenderness
- Muscle spasms and changes in posture
- Limited range of motion in the neck if cervical vertebrae are affected
- “Crunching” sounds during spine movement
Facet arthropathy can significantly impact your daily life, but with the right treatment, you can manage the symptoms effectively. Physical therapy, in particular, can play a crucial role in improving your mobility and reducing pain, helping you regain your quality of life.
Intense discomfort. Tingling sensations. Poor alignment.
Compression fractures can strike unexpectedly, turning simple tasks into significant challenges. Although these fractures are common among older adults, effective treatments exist to help you regain your quality of life.
This guide explores compression fractures, available treatments, and how physical therapy can assist in your recovery.
Contents
- What Is a Compression Fracture?
- Causes of Compression Fractures
- Risk Factors for Compression Fractures
- Prevalence of Compression Fractures
- Symptoms of Compression Fractures
- Diagnosing a Compression Fracture
- Treatment Options
- Physical Therapy Benefits
- Key Exercises for Recovery
- How HB BodyLab Can Assist
What Is a Compression Fracture? A compression fracture occurs when a vertebra in your spine cracks or collapses. These fractures are most often found in the middle section of the spine (thoracic region) and can cause the vertebrae to become shorter.
When vertebrae collapse, fragments can press against the spinal cord and nerves, reducing blood flow and oxygen, and potentially causing a hunched posture.
Causes of Compression Fractures The leading cause of compression fractures is osteoporosis, a condition that weakens bones, making them more susceptible to breaks. Moderate osteoporosis can lead to fractures from minor falls or injuries, while severe osteoporosis can result in fractures from everyday movements like bending over or sneezing.
Younger individuals without osteoporosis can also suffer from compression fractures due to high-impact trauma from car accidents, sports injuries, or spinal tumors. Tumors, whether originating in the spine or metastasized from another area, can weaken vertebrae and cause fractures.
Risk Factors for Compression Fractures While men can experience compression fractures, women over 50 are at higher risk due to osteoporosis. Menopause significantly reduces estrogen levels, accelerating bone loss. Additionally, those who have already experienced a compression fracture are more likely to have another.
Prevalence of Compression Fractures Compression fractures are common, with around 1.5 million cases reported annually in the U.S. Nearly 50% of individuals over 80 have experienced a compression fracture.
Symptoms of Compression Fractures Early stages of compression fractures might be asymptomatic and often discovered incidentally during X-rays for other issues. As the condition progresses, symptoms can range from mild to severe, including:
- Sudden, chronic back pain
- Tingling or numbness from nerve compression
- Muscle weakness due to nerve damage
- Difficulty walking or standing due to nerve issues
- Loss of bladder or bowel control in severe cases
- Reduced spinal mobility, making it hard to bend or twist
- A stooped posture due to vertebral compression
- Height loss as the vertebrae compress
Diagnosing a Compression Fracture To diagnose a compression fracture, your healthcare provider will review your medical history, recent injuries, and symptoms, and conduct a physical examination. During the exam, they may:
- Assess your posture and spinal alignment
- Press on different parts of your back to locate pain
- Check for nerve damage (numbness or muscle weakness)
- Order imaging tests like X-rays, CT scans, or MRIs to confirm fractures and other spinal issues
Treatment Options Treating a compression fracture often involves pain management, physical therapy, and lifestyle changes. In some cases, surgical interventions like vertebroplasty or kyphoplasty might be necessary to stabilize the spine.
Physical Therapy Benefits Physical therapy is crucial in the recovery process, helping to:
- Improve mobility and flexibility
- Strengthen supporting muscles
- Reduce pain and discomfort
- Enhance overall spinal function
Key Exercises for Recovery Specific exercises can aid in the recovery from a compression fracture. These include:
- Gentle stretching to improve flexibility
- Strengthening exercises for the back and core muscles
- Low-impact aerobic activities to enhance cardiovascular health
How HB BodyLab Can Assist At HB BodyLab, our experts provide personalized physical therapy plans tailored to your needs, ensuring a comprehensive approach to managing and recovering from compression fractures. Our goal is to help you regain your strength and enjoy life without pain.

Elbow
At HB BodyLab, we cater to clients with diverse lifestyles and physical goals. To maximize your quality of life, it’s essential to ensure your body functions optimally. When pain takes over, it distracts us from life’s possibilities. Limited mobility and weakness in our bones, ligaments, and muscles can diminish our confidence and willingness to try new things. Depending on your activities, age, and current physical condition, we develop a customized physical therapy and personal training plan tailored just for you. Our aim is to help you realize your potential, grow stronger, and enhance your range of motion with the support of our expert physical therapy team.
Common Ailments Treated at HB BodyLab:
Discomfort or irritation on the inner side of your arm and elbow might be a sign of golfer’s elbow, even if you’ve never set foot on a golf course.
Being diagnosed with golfer’s elbow means you’re familiar with the pain that can disrupt your daily activities.
You don’t have to live with this discomfort. Physical therapy offers effective treatments and exercises to help alleviate the pain and get you back to your routine.
This guide will cover:
- Symptoms
- Physical therapy exercises for golfer’s elbow
- Stretches for golfer’s elbow
- And more
What Is Golfer’s Elbow? Known medically as medial epicondylitis, golfer’s elbow causes pain where the tendons of your forearm muscles attach to the bony bump on the inside of your elbow.
Similar to tennis elbow (which affects the outside of the joint), golfer’s elbow is a form of tendinitis caused by overuse or injury. Small tears in the tendon connecting the elbow to the wrist lead to inflammation and pain in the:
- Elbow
- Forearm
- Wrist
What Causes Golfer’s Elbow? Golfer’s elbow results from damage to the muscles and tendons that control your wrist and fingers. The primary cause is overuse, involving repeated stress and forceful wrist and finger movements.
While swinging a golf club can lead to this condition, many other activities can cause it as well, including:
- Weight lifting: Improper technique can strain elbow muscles and tendons.
- Racket sports: Using a racket that’s too small or too heavy, or improper technique can be problematic.
- Throwing sports: Poor form in activities like baseball, football, archery, and javelin can contribute.
Additionally, certain jobs that involve repetitive motions can lead to golfer’s elbow, such as:
- Butchers
- Plumbers
- Construction workers
- Assembly line workers
- Cooks
- Painters
- Meat processors
Engaging in these activities for more than an hour daily over several days can lead to joint strain and pain.
Risk Factors Associated with Golfer’s Elbow You might be at higher risk for golfer’s elbow if you:
- Are 40 years old or older
- Perform repetitive activities for at least two hours a day
- Are obese
- Are a smoker
Prevention of Golfer’s Elbow If you think you’re at risk or engage in activities that could lead to golfer’s elbow, there are preventative steps you can take:
- Strengthen forearm muscles: Use light weights or squeeze a tennis ball.
- Prepare for activities: Warm up with walking or jogging, then do gentle stretches.
- Correct your form: Get guidance from an instructor to avoid muscle and joint overload.
- Use proper equipment: Consider upgrading to lighter graphite clubs if your current ones are heavy.
- Lift properly: Use correct techniques when lifting, including weights.
- Rest appropriately: Avoid overuse of your elbow and take breaks at the first sign of pain.
Golfer’s Elbow Symptoms Symptoms of golfer’s elbow can vary and may include:
- Pain and tenderness: Usually on the inner side of the elbow, worsening with certain movements.
- Stiffness
- Weakness: Typically in the hands and wrists.
- Numbness and tingling: May radiate into the ring and pinky fingers.
Symptoms can develop suddenly or gradually and may worsen with activities like swinging a golf club.
By understanding and addressing golfer’s elbow, you can take steps towards managing the pain and returning to your regular activities with the help of physical therapy.
You’ve been diagnosed with radial tunnel syndrome and you’re desperate for relief. Your doctor may have prescribed a splint, the typical treatment for this condition, but you feel there must be more you can do to alleviate your pain.
The good news is that many people with radial tunnel syndrome have found significant relief through physical therapy and specific exercises.
Read on to learn all about radial tunnel syndrome — what it is, why it causes pain, and effective ways to manage it.
What is Radial Tunnel Syndrome? Radial tunnel syndrome happens when the radial nerve in your arm gets compressed. This nerve runs through a narrow passageway called the radial tunnel, which is surrounded by muscles, tendons, and ligaments near your elbow and forearm.
We’ll delve into the causes below, but some reasons for this compression include:
- Injury
- Repetitive movements
- Ganglia (cysts)
- Bone tumors
- Inflammation
Pain and weakness in your forearm often occur when you try to straighten your wrist and fingers.
What Causes Radial Tunnel Syndrome? Radial tunnel syndrome is often caused by repetitive, forceful motions like pushing, pulling, or twisting with your hand. However, direct injury to the outer elbow can also lead to this condition.
Understanding Your Anatomy The radial nerve travels down the underside of your arm, controlling the movement of the triceps muscle at the back of your upper arm. This nerve is essential for extending the wrist and fingers and also provides sensation to part of the hand.
When the radial nerve gets compressed, radial tunnel syndrome can develop, which is also known as radial nerve entrapment.
Common Causes Any compression along the radial nerve can lead to pain, with the elbow tunnel being a common pinch point. Overuse is the most frequent cause, leading to inflammation from repeated motions like:
- Twisting the arm
- Twisting the wrist
- Bending the wrist
- Gripping with the hand
Activities that can contribute to this condition include sports, repetitive work tasks, and even typing. Jobs that often lead to radial tunnel syndrome include:
- Sewers or knitters
- Bakers
- Cashiers
- Hair stylists
- Musicians
- Industrial workers
- Assembly line workers
Less common causes are:
- Injury
- Ganglia
- Bone tumors
Symptoms of Radial Tunnel Syndrome Many people describe radial tunnel syndrome as a “dull aching pain,” though some experience a cutting, piercing, or stabbing sensation. This pain typically affects the:
- Top of the forearm
- Outside of the elbow
- Back of the hand
The pain usually intensifies when you straighten your wrist or fingers.
Finding Relief Physical therapy can be highly effective in treating radial tunnel syndrome. It can help reduce pain, improve mobility, and strengthen the muscles around the affected area. Your physical therapist may recommend exercises and stretches specifically designed to alleviate your symptoms and prevent future occurrences.
By understanding radial tunnel syndrome and its causes, you can take proactive steps toward managing your pain and regaining your quality of life.
If you’ve been diagnosed with tennis elbow (lateral epicondylitis), you might wonder how you got it without ever picking up a tennis racket.
Rest assured, you’re not unknowingly hitting the courts at night.
You likely have a repetitive strain injury from a job or activity that involves repetitive motions, putting stress on the tendons in your elbow.
So, how can you address this issue?
In this guide, we’ll cover everything you need to know about tennis elbow and what to expect during your recovery.
What is Tennis Elbow? Tennis elbow is the inflammation of the tendon that attaches your lower arm muscles to the bony area of your elbow (the epicondyle). This condition is typically caused by repetitive motion and overuse.
Pain is usually felt where the tendon connects to the bone but can also spread through the forearm to the wrist.
What Causes Tennis Elbow? Tennis elbow can affect anyone who performs activities requiring extensive use of the wrist and hand.
Examples include:
- Using a computer
- Playing racket sports with improper technique
- Operating machinery
- Using hand tools like screwdrivers
While nearly half of all racket sports players may experience tennis elbow, it can also affect:
- Men
- Women
- Children
- Athletes and non-athletes
- Dentists
- Carpenters
- Gardeners
This condition is most common in people aged 30 to 50 and occurs more frequently in men.
Tennis Elbow Symptoms Symptoms of tennis elbow can develop suddenly or gradually, depending on the activity.
Activities involving forceful or repetitive wrist and hand use can cause a sudden onset of symptoms. These activities include:
- Excessive pulling
- Heavy lifting
- Twisting
However, tennis elbow symptoms typically develop over weeks or months and may include:
- Pain radiating from the elbow through the forearm and wrist
- Difficulty or pain when gripping objects, like holding a pen or opening a jar
- Weakness in the hand, wrist, or forearm
- Stiffness in the elbow
If you experience any of these symptoms, a physical therapist can assist you. They will examine your elbow and surrounding areas that might be contributing to the pain and perform manual tests to pinpoint the problem’s cause and location.
Diagnostic imaging tests are rarely needed to diagnose tennis elbow.
Cubital tunnel syndrome, also known as ulnar neuropathy, often brings severe pain and discomfort that can feel overwhelming.
Wondering if there are treatments like physical therapy or exercises that can help?
You’re in luck.
At HB BodyLab, we understand the importance of living a pain-free life, and we’re here to help you find relief.
In this guide, we’ll cover everything you need to know about cubital tunnel syndrome and ways to alleviate the associated pain and discomfort.
What is Cubital Tunnel Syndrome? Cubital tunnel syndrome occurs when your ulnar nerve, one of the three primary nerves in your arm, gets compressed. This nerve runs from your neck down to your hand.
The ulnar nerve can become:
- Stretched
- Inflamed
- Injured
- Swollen
- Irritated
The pain from cubital tunnel syndrome is similar to the sensation you feel when you hit your “funny bone,” as it involves the same nerve at the elbow. However, unlike the fleeting discomfort of hitting your funny bone, cubital tunnel syndrome can cause persistent pain.
Often confused with carpal tunnel syndrome, which affects the wrist and typically impacts the thumb, index finger, and middle finger, cubital tunnel syndrome specifically affects the area around the elbow.
What Causes Cubital Tunnel Syndrome? Several factors can lead to cubital tunnel syndrome, including:
- Keeping the elbow bent beyond 90 degrees for long periods
- Prolonged leaning on the elbow
- Diabetes
- Joint damage from arthritis (though less common in the elbow)
- Bone spurs
- Previous fractures or dislocations of the elbow
- Fluid retention during pregnancy
To diagnose cubital tunnel syndrome, your doctor will likely start with a physical exam and may follow up with a nerve conduction study or electromyogram to pinpoint where the nerve compression is occurring. X-rays might also be ordered to look for visible signs of compression.
Cubital Tunnel Syndrome Symptoms Symptoms of cubital tunnel syndrome can vary from person to person. Common symptoms include:
- Numbness in the hand, particularly in the ring finger and little finger, especially when the elbow is bent
- Hand pain
- Weak grip
- Loss of sensation
- Clumsiness due to muscle weakness
- Aches on the inside of the elbow
- Difficulty bending or straightening the fingers
If you experience any of these symptoms, HB BodyLab can help you with a tailored physical therapy program designed to alleviate your pain and improve your quality of life.
You might not realize how crucial your elbow is for daily activities until it’s injured.
Perhaps you’ve dislocated your elbow from a fall, car accident, or a hard tackle while playing football.
Regardless of whether you need surgery, physical therapy is key to relieving pain and restoring your range of motion.
This guide provides comprehensive information about:
- Elbow dislocation
- Treatment options
- Effective exercises for improving elbow strength and mobility
What is Elbow Dislocation? An elbow dislocation happens when the bones forming the elbow joint are forced out of alignment, typically due to landing on an outstretched hand during a fall. The elbow joint connects the forearm (radius and ulna) with the upper arm (humerus).
Elbow dislocations are categorized into three types based on severity:
- Simple
- Complex
- Severe
Simple Elbow Dislocation A simple elbow dislocation involves only soft tissue injuries without major bone damage. This type accounts for over half of all elbow dislocations.
Complex Elbow Dislocation A complex elbow dislocation includes severe injuries to the bones and ligaments, such as fractures. These make up 5-20% of elbow dislocations.
Severe Elbow Dislocation Severe elbow dislocations involve damage to the nerves and blood vessels around the elbow, in addition to bone and ligament injuries.
What Causes Elbow Dislocation? An elbow dislocation occurs when one of the three bones in the elbow joint gets separated or pushed out of place, usually due to significant force.
Falling Down Most elbow dislocations are caused by falls, especially when you instinctively try to break your fall with an outstretched arm. This can pop the upper arm bone out of alignment with the elbow joint. Older adults are particularly prone to falls.
Accidents Car accidents can lead to elbow dislocations, often when individuals brace for impact, causing the elbow to pop out of position.
Sports Injuries Approximately half of elbow dislocations in teens and young adults result from sports activities. Significant force, such as a hit during contact sports (football, hockey, soccer) or a fall (basketball, pole vaulting), can dislocate the elbow. Other sports where elbow dislocations occur include:
- Gymnastics
- Cheerleading
- Wrestling
- Rollerblading
- Skateboarding
- Skiing
- Snowboarding
- Ice skating
Elbow Dislocation Symptoms Symptoms of an elbow dislocation often appear immediately after a trauma or fall, including:
- Severe pain
- Bruising
- Swelling
- Weakness in the joint
- Inability to bend the arm
- Obvious distortion of the elbow joint
- Loss of feeling in the hand
- No pulse in the wrist
If you suspect an elbow dislocation, seek medical attention promptly. Physical therapy at HB BodyLab can then help you manage pain, regain strength, and restore the range of motion in your elbow.
There are various types of humerus bone fractures, each with its own level of pain and potential need for surgery. The good news is that full recovery is possible, and physical therapy plays a vital role in regaining strength and mobility.
This guide covers the causes, symptoms, and treatment of humerus fractures, and explains how physical therapy can aid in recovery.
What Is a Humerus Fracture? The humerus is the sole bone in your upper arm and one of the body’s strongest bones. Fractures typically result from high-impact trauma, such as car accidents or significant falls.
A humerus fracture refers to a break in the upper arm bone, categorized based on the fracture’s location:
- Proximal: Upper part of the humerus
- Mid-shaft: Middle section of the humerus
- Distal: Near the elbow
Other specific types of humerus fractures include:
- Oblique fracture
- Transverse fracture
- Segmental fracture
- Spiral fracture
- Comminuted fracture
- Impacted fracture
- Hairline fracture
- Buckle fracture
What Causes Humerus Fractures? Humerus fractures occur due to a significant impact to the upper arm, such as:
- Car Accidents: High-impact collisions can break the humerus.
- Sports Injuries: Contact sports and activities like football, javelin throwing, or baseball pitching can cause fractures.
- Falls: Falling onto an outstretched arm can lead to a break.
Bone Weakness and Humerus Fractures Conditions that weaken bones can increase the risk of humerus fractures. Osteoporosis is a primary cause of bone fragility, often undetected until a fracture occurs. Women and individuals over 50 are particularly at risk, making bone density screenings crucial for early detection.
Other conditions that can weaken bones and lead to fractures include:
- Bone cancer
- Bone infections
- Bone tumors or cysts
Humerus Fracture Symptoms Symptoms of a humerus fracture can include:
- Pain
- Tenderness
- Swelling
- Inability to move the arm or shoulder
- Bruising
- Deformity (visible bump or bulge)
- Grinding sensation when moving the shoulder
- Bleeding (in case of an open fracture)
Fractures can also cause damage to muscles, nerves, and blood vessels.
Treatment and Recovery Treatment for humerus fractures depends on the fracture type and severity. Options may include immobilization with a cast or splint, pain management, and possibly surgery for severe cases.
Physical Therapy for Humerus Fractures Physical therapy is crucial for a full recovery from a humerus fracture. It helps restore strength, flexibility, and range of motion. Therapists at HB BodyLab will design a personalized program to aid your recovery and ensure you return to your normal activities as quickly as possible.
By following a structured physical therapy plan, patients can significantly improve their outcomes and regain full function of their arm.
Pitcher’s elbow is a prevalent overuse injury among young baseball pitchers, caused by repetitive throwing motions.
The pain and reduced range of motion from this injury can sideline pitchers, requiring time off for recovery. Physical therapy is essential for healing, strengthening, and returning to play.
This guide will explain pitcher’s elbow, its causes, treatment options, and the benefits of physical therapy.
What Is Pitcher’s Elbow? Also known as epicondyle apophysitis, pitcher’s elbow commonly affects baseball players, particularly pitchers. The condition arises from repetitive throwing, leading to pain and swelling on the inner elbow.
Pain is typically felt during or after pitching due to the stress on ligaments and tendons. Besides pain, pitchers may experience limited range of motion.
Injuries can range from mild to severe. Medial epicondylitis involves tendon damage, while more severe cases may affect the ulnar collateral ligament (UCL), crucial for elbow stability during throws.
What Causes Pitcher’s Elbow? Pitcher’s elbow results from the repetitive strain on tendons and ligaments associated with pitching. The injury is more common in adolescents whose elbow structures are not fully developed, but it also affects many MLB players.
Factors influencing the incidence of pitcher’s elbow include:
- Number of pitches thrown
- Number of innings played
- Duration of the pitching season
The risk is highest when pitchers continue to throw despite pain or fatigue.
Although most common in baseball, pitcher’s elbow can also occur in:
- Football
- Softball
- Gymnastics
- Wrestling
- Tennis
- Javelin throwing
Rarely, the condition can result from trauma.
Risk Factors Associated with Pitcher’s Elbow Certain factors increase the likelihood of pitcher’s elbow, including:
- Age: Young players (ages 9-14) are more vulnerable due to underdeveloped elbow joints.
- Number of pitches: Excessive pitching per game, season, or year raises injury risk. Adhering to pitch count rules is crucial.
- Improper mechanics: Incorrect pitching techniques can stress the elbow joint. Coaches should ensure proper technique.
- Types of pitches thrown: Curveballs and breaking pitches stress the growth plates in younger players.
Pitcher’s Elbow Symptoms The primary symptom of pitcher’s elbow is pain on the inside of the elbow during and after throwing. Other signs include:
- Decreased pitching velocity
- Pitches sailing high
- Numbness or tingling in the elbow, forearm, or hand
- Limited range of motion
Symptoms usually develop gradually, but severe injuries might cause a popping or tearing sensation, with the elbow feeling locked.
Treatment and Recovery Treatment for pitcher’s elbow often involves rest, ice, and anti-inflammatory medications. In severe cases, surgery might be necessary. Physical therapy is a key component of recovery, helping to:
- Reduce pain and inflammation
- Restore range of motion
- Strengthen muscles around the elbow
- Improve pitching mechanics
Physical Therapy for Pitcher’s Elbow At HB BodyLab, we offer personalized physical therapy programs to help athletes recover from pitcher’s elbow. Our therapists focus on exercises that enhance strength and flexibility, ensuring a safe return to the sport.
By understanding and addressing pitcher’s elbow, players can effectively manage their symptoms and get back to doing what they love.

Hand + Wrist
At HB BodyLab, we understand that bones, joints, ligaments, and muscles endure strain and injury throughout our lives. The hand and wrist are particularly vulnerable due to the repetitive motions we perform and the extensive range of movement in the wrist. Consider how often we use our hands and wrists for tasks like opening doors, pushing and pulling objects, lifting, typing, and driving. This constant activity can lead to significant wear and tear where the hand and wrist meet.
Our clients frequently experience various types of pain in their hands and wrists. This discomfort often leads them to limit the use of their hands and wrists, which isn’t always practical or beneficial. During our physical therapy sessions at HB BodyLab, we focus on understanding and alleviating this pain through appropriate movements, increasing range of motion, and preventing further injury. We rejuvenate muscles, tendons, and joint function to enhance performance, allowing you to engage in activities you may have previously avoided. Physical therapy and fitness training at HB BodyLab are not just about pain management; they’re about improving lives and enhancing the quality of life for every client.
As we address pain types, causes, and pain reduction options, we’ll explore the structure of the hand and wrist. Understanding this structure helps you relate to the activities you perform and identify the source of discomfort. Your therapist will assess your symptoms and determine if additional therapeutic exercises are needed to regain flexibility and function once the pain’s cause is identified.
Common Ailments Treated at HB BodyLab:
You might notice a persistent tingling sensation in your hand, like the tips of your fingers are being shocked or parts of your hand are going numb. These could be signs of carpal tunnel syndrome.
In this guide, we’ll explore the signs and symptoms of carpal tunnel syndrome and the treatment options available, including physical therapy.
What is Carpal Tunnel Syndrome? Carpal tunnel syndrome occurs when the median nerve, which runs through the carpal tunnel — a narrow passage in the wrist made of ligaments and bones — becomes compressed and inflamed. This nerve controls movement and sensation in the thumb and all fingers except the pinky.
When compressed, the median nerve can cause numbness, tingling, and weakness in the hand and arm.
What Causes Carpal Tunnel Syndrome? Anything that increases pressure on the median nerve can lead to carpal tunnel syndrome. Common causes include:
- Wrist fractures that narrow the carpal tunnel or irritate the median nerve
- Repetitive hand and wrist movements, such as typing, using a computer mouse, or playing an instrument
- Swelling from rheumatoid arthritis that compresses the median nerve
- Inflammation of surrounding tendons putting pressure on the median nerve
Risk Factors for Carpal Tunnel Syndrome Carpal tunnel syndrome often develops due to a combination of risk factors rather than a single cause. These risk factors include:
- Anatomical Issues: Wrist deformities, smaller carpal tunnels, arthritis, and wrist fractures or dislocations can all compress the median nerve.
- Inflammatory Conditions: Conditions like rheumatoid arthritis can cause tendon inflammation, leading to nerve compression.
- Nerve-Damaging Conditions: Diabetes and other conditions that increase the risk of nerve damage can also increase the risk of carpal tunnel syndrome.
- Medical Conditions: Obesity, menopause, thyroid disorders, kidney failure, and lymphedema can increase the risk of developing carpal tunnel syndrome.
- Gender: Women are twice as likely to develop carpal tunnel syndrome, likely due to having smaller carpal tunnels.
- Medications: Some drugs, such as the breast cancer treatment anastrozole, have been linked to carpal tunnel syndrome.
- Fluid Retention: Conditions that cause fluid retention can increase pressure in the carpal tunnel, such as pregnancy.
- Occupational Factors: Jobs requiring repetitive wrist motions or strong vibrations from tools can aggravate the median nerve.
Symptoms of Carpal Tunnel Syndrome Symptoms of carpal tunnel syndrome typically develop gradually and may include:
- Tingling or Numbness: The most common symptom, often described as a “pins and needles” sensation, especially in the thumb, index, and middle fingers.
- Pain or Discomfort: Pain can be felt in the hand, wrist, or forearm and may radiate up the arm.
- Weakness: Difficulty gripping objects or performing fine motor tasks, such as buttoning a shirt or holding a pencil.
- Swelling: Swelling in the fingers or hand can make it difficult to wear rings or jewelry.
- Worsening Symptoms at Night: Many people experience increased symptoms at night, disrupting sleep.
- Reduced Range of Motion: In some cases, a reduced range of motion in the wrist or hand can occur.
If you experience these symptoms, consult your doctor to rule out other hand injuries and confirm a diagnosis. Physical therapy can be an effective treatment to help alleviate symptoms and improve function. At HB BodyLab, our tailored physical therapy programs aim to reduce pain, restore function, and improve the quality of life for those suffering from carpal tunnel syndrome.
If you’ve had a sudden fall or taken a hit to your wrist and now experience pain or swelling, you might be dealing with a wrist sprain.
Wrist sprains are common injuries among athletes, but they can happen to anyone. This injury can be quite uncomfortable and restrict your ability to perform daily activities, which can be very frustrating.
The silver lining is that mild to moderate wrist sprains can heal relatively quickly with appropriate treatment.
In this guide, we’ll explain everything you need to know about wrist sprains and how to get back to your normal activities.
What is a Wrist Sprain? Your wrist comprises eight small bones arranged in two rows. These bones are held together by ligaments, as they lack direct muscle or tendon attachments. The stability of your wrist relies entirely on these ligaments.
A wrist sprain happens when an impact causes the wrist to bend in a way that overstretches the ligaments connecting the wrist and hand bones. If these ligaments are stretched too far, they can tear or break, classifying the sprain as Grade I, II, or III.
What Causes a Wrist Sprain? Wrist sprains frequently result from trauma, such as trying to break a fall with your hand. This action can stretch the ligaments beyond their normal range of motion.
While falls are a common cause, wrist sprains can also occur from extreme twisting or pressure on the wrist.
Wrist sprains are categorized into three grades:
Grade I (Mild):
- Ligaments are stretched or have microscopic tears.
- Pain with minor ligament damage.
Grade II (Moderate):
- More severe ligament damage, possibly torn.
- Pain, loss of function, and joint looseness.
Grade III (Severe):
- One or more ligaments are completely torn from their attachment to the bone.
- Intense pain and significant joint looseness.
Wrist Sprain Symptoms If you’ve experienced a fall, hit, twist, or pressure on your wrist, you might notice symptoms indicating a sprain:
- Pain
- Swelling or bruising
- Warmth and tenderness around the injury
- Loss of motion
- Joint looseness
- Weakness
- Popping or clicking sound when moving the wrist
If you experience any of these symptoms, it’s important to consult a physician or a doctor of physical therapy for an accurate diagnosis.
Diagnosis and Treatment Your doctor will perform a thorough examination and may order additional tests such as:
- X-ray or CT scan
- MRI (magnetic resonance imaging)
- Arthrogram (dye injection followed by x-ray or MRI)
- Arthroscopy (surgical insertion of a small camera into the wrist)
Seeking medical attention promptly can help prevent further wrist damage.
Recovery and Physical Therapy Mild-to-moderate wrist sprains typically heal well with rest, ice, compression, and elevation (RICE). Severe sprains might require immobilization with a brace or even surgery.
Physical therapy is crucial for recovery, focusing on restoring strength and range of motion. At HB BodyLab, our experienced therapists will develop a personalized treatment plan to help you regain full wrist function and return to your normal activities as quickly as possible.
You may notice a catching sensation when you bend your finger, accompanied by pain and difficulty moving it. These could be signs of trigger finger.
In this guide, we’ll cover the signs and symptoms of trigger finger and explore treatment options to alleviate your discomfort.
What is Trigger Finger? Trigger finger is a painful condition where one of your fingers gets stuck in a bent position. It feels like your finger is catching when you bend or straighten it, much like pulling and releasing a trigger. In severe cases, the finger may become locked in a bent position.
What Causes Trigger Finger? Trigger finger is typically caused by repetitive movements or forceful use of the fingers. Inflammation of the tendon sheath in the finger disrupts the smooth gliding motion of the tendon through the sheath, leading to trigger finger. Prolonged irritation can cause scarring, thickening, and bumps, further impeding the tendon’s motion.
Trigger Finger Risk Factors Several risk factors can increase the likelihood of developing trigger finger, including:
- Repetitive Gripping: Activities or jobs that involve repetitive gripping or forceful finger use.
- Gender: Women are six times more likely to develop trigger finger than men.
- Medical Conditions: Individuals with diabetes and rheumatoid arthritis are at higher risk.
- Post-Surgery Complications: Trigger finger can sometimes occur as a complication of carpal tunnel syndrome surgery.
Trigger Finger Symptoms Trigger finger can affect any finger and may involve multiple fingers simultaneously. Symptoms vary in severity depending on the level of inflammation. You may experience:
- Stiffness: Particularly noticeable in the morning.
- Popping or Clicking Sensation: Felt when bending the finger.
- Bump or Tenderness: At the base of the affected finger.
- Catching Sensation: When the finger is bent and suddenly pops straight.
- Inability to Straighten the Finger: From a bent position.
If the finger joint is inflamed and hot to the touch, seek medical treatment immediately as this could indicate an infection.
Treatment Options It’s essential to speak with your doctor about your symptoms to rule out other hand injuries and confirm a diagnosis. Treatment options for trigger finger may include:
- Rest: Avoiding activities that exacerbate symptoms.
- Splinting: Wearing a splint to keep the finger in a straight position.
- Medications: Anti-inflammatory medications to reduce pain and swelling.
- Steroid Injections: To decrease inflammation in the tendon sheath.
- Physical Therapy: Exercises to improve flexibility and strength.
- Surgery: In severe cases, to release the affected tendon.
Early intervention and proper treatment can help you manage trigger finger effectively and return to your normal activities.
Are you dealing with wrist tendonitis?
The pain can be severe, making daily tasks like carrying groceries or driving nearly impossible, and you might worry that the pain will never subside.
Coping with wrist tendonitis is incredibly challenging.
Fortunately, there are various ways to manage wrist tendonitis and ease the discomfort.
In this guide, we’ll discuss the causes, common symptoms, and treatment options for wrist tendonitis, including the benefits of physical therapy.
What is wrist tendonitis?
Wrist tendonitis occurs when one or more of the tendons connecting the wrist to the forearm become inflamed. This condition can manifest in different forms, such as:
- Wrist tendonitis: Early stages of irritation and inflammation.
- Tendinopathy: When the condition becomes chronic.
- De Quervain’s tenosynovitis: Tendonitis on the thumb side of the wrist.
- Tenosynovitis: Inflammation when the synovial sheath thickens and restricts the tendon.
The pain and inflammation can hinder the movement of your hand, wrist, and fingers. Seeking early treatment can help reduce symptoms and prevent the condition from becoming chronic.
What causes wrist tendonitis?
Wrist tendonitis results from the excessive use or wear of the joints in the hand. Several factors contribute to this condition, including repetitive motions, age, and arthritis.
Repetitive motions
Repetitive motions of the hand, forearm, and wrist can lead to tendonitis. Those at risk include:
- Factory workers
- Construction workers
- Office workers
- Landscapers
A University of Michigan study indicates that people in these professions are 29 times more likely to develop wrist tendonitis.
Age
Wrist tendonitis is more common in individuals over 40. The repetitive motions that cause tendonitis take a toll on the body as we age, making it easier for the condition to develop.
Arthritis
Arthritis, which causes joint inflammation, can also lead to wrist tendonitis. It can damage tendons in the arms and hands, resulting in pain and stiffness.
Wrist tendonitis symptoms
Common symptoms of wrist tendonitis include:
- Pain where the hand meets the arm, often extending to the elbow
- Pain on the thumb or pinky side of the wrist
- Pain when applying pressure to the hand
- Pain with wrist movement
- Inflammation in the wrist
- Tenderness in the wrist and forearm muscles
- Stiffness in the wrist
- Decreased ability to extend or bend the wrist
- Loss of grip strength
Pain
Pain is a major symptom and can indicate worsening tendonitis or other conditions like arthritis or a torn tendon. It’s crucial to seek medical attention for an accurate diagnosis.
Swelling
Swelling can occur along the wrist, at the base of the fingers, or between the pinky and thumb due to tendon inflammation.
Stiffness
Stiffness or tightness in the wrist can make gripping objects and moving the hand difficult. If you experience these symptoms, consult a doctor for an evaluation.
How is wrist tendonitis diagnosed?
Diagnosing wrist tendonitis involves a comprehensive evaluation of your entire arm. Your physical therapist will ask about your daily activities and identify which ones cause pain.
They will assess your arm’s strength and range of motion and use manual techniques, such as applying gentle pressure, to pinpoint the affected tendons and check for swelling.
Early diagnosis and treatment can help manage symptoms effectively and prevent long-term issues.

Hip
At HB BodyLab, understanding the anatomy and physiology of your body helps identify common sources of pain. In our detailed sections on ailments we treat, we cover pain in the vertebrae of the neck, head, upper and lower back, as well as the sacroiliac joint, which connects the sacrum (the base of the spine) to the ilium. We explain the causes of hip pain and how you can alleviate it at home or through exercises recommended by our physical therapists. HB BodyLab provides valuable information on frequent pain areas and offers advice on pain reduction until you can attend a physical therapy consultation.
Common Ailments Treated at HB BodyLab:
You’re experiencing hip pain accompanied by a snapping or popping sensation when you walk, run, stand up, or sit down. This condition, known as snapping hip, is aptly named because the sensation is often audible. Fortunately, you don’t have to live with this discomfort; there are treatments available.
Read on to learn about:
- Types of snapping hip injuries
- Causes of snapping hip syndrome
- Treatment options for snapping hip
- How physical therapy can help
What is Snapping Hip?
Snapping hip syndrome, also known as coxa saltans or dancer’s hip, is a condition where you hear or feel a snapping sensation in the hip. It is common among athletes and dancers. There are three main types:
- Internal
- External
- Intra-articular
This condition can result from overuse of hip muscles, causing them to become fatigued, tight, or swollen. While often harmless, it can increase the risk of joint damage, particularly in athletes.
Internal Snapping Hip
The most common type, internal snapping hip, occurs when tendons slide over bone structures at the front of the hip joint, causing pain near the groin. This can potentially lead to a hip labrum tear.
External Snapping Hip
External snapping hip happens when a tendon or muscle slides over the top of the femur. The pain usually starts as a mild annoyance and worsens over time. It often feels like the hip is about to pop out of its socket during activities like walking or cycling. This type is often linked to trochanteric bursitis and a tight IT band.
Intra-Articular Snapping Hip
This least common type is due to a hip joint injury rather than a tendon or muscle issue. It can develop suddenly, often due to trauma, and may cause the hip to lock up, limiting the range of motion.
What Causes Snapping Hip?
Snapping hip occurs when a tendon or muscle slides over a bone, stretching and then snapping when tension is released. The underlying cause varies by type:
Internal Snapping Hip
Caused by repetitive flexion and external rotation of the hip, often seen in athletes with tight hip flexors and imbalanced strength in the pelvic, hip, and abdominal muscles.
External Snapping Hip
Associated with conditions like differing leg lengths (typically the longer leg is affected), tightness in the IT band, and weakness in the hip abductors. It often involves tenderness on the outside of the hip.
Intra-Articular Snapping Hip
Results from actual hip joint injuries such as cartilage damage, hip labral tears, or fragments of bone or tissue trapped in the hip joint, typically following trauma.
Snapping Hip Symptoms
The primary symptom is the snapping sensation in the hip, which can often be heard. Other symptoms include:
- Pain
- Inflammation
- Leg muscle weakness
- Swelling
- Difficulty with physical activity
- Feeling that the hip is popping out of place
If you’re experiencing these symptoms, seeking medical advice and considering physical therapy can help manage and alleviate your discomfort, allowing you to return to normal activities.
Hip bursitis is a painful condition resulting from inflammation of the bursa in the hip. These fluid-filled sacs cushion the tendons, ligaments, and muscles, allowing them to glide smoothly over the bone. However, when they become inflamed, they can cause significant discomfort.
What Causes Hip Bursitis?
When the bursae are inflamed, the surrounding area becomes tender and painful. This condition, also known as trochanteric bursitis, can be triggered by various factors, including:
- Repetitive overuse or stress on the hip
- Rheumatoid arthritis
- Gout
- Hip injuries
- Infections (such as a staph infection)
- Diabetes
- Uneven leg lengths
- Spine issues (such as scoliosis or spinal disease)
- Bone spurs on the hip
Two of the most common causes are:
Inactivity or Muscle Weakness: Periods of inactivity or illness can weaken the abductor muscles, increasing pressure on the bursa and leading to bursitis.
Pinched Nerves in the Lower Back: This can weaken the abductor muscles and contribute to hip bursitis.
Hip Bursitis Symptoms
The initial symptom of hip bursitis is typically joint pain and tenderness, often accompanied by swelling and warmth in the affected area. The pain may also radiate to the groin region.
Initially, the pain may be sharp, becoming dull and achy over time. Activities that can exacerbate the pain include:
- Rising from a chair
- Getting out of bed
- Lying on the affected side
Hip bursitis can be acute or chronic. Acute bursitis develops over hours or days, while chronic bursitis may last from a few days to several weeks and can recur. Chronic bursitis can lead to limited movement and muscle weakness if the inflammation worsens.
Diagnosing Hip Bursitis
To diagnose hip bursitis, your doctor will examine you and ask about your symptoms. Tenderness and swelling over the bursa usually confirm the diagnosis. To rule out other conditions or check for bone spurs, your doctor may order:
- X-ray: To look for bone spurs.
- MRI: To view soft tissues and structures not visible on an X-ray.
By understanding the causes, symptoms, and diagnostic methods for hip bursitis, you can take steps towards managing the condition and finding relief from the pain and discomfort it brings.
You’ve had or are planning to have a hip replacement and you’re wondering what to expect afterward.
After hip replacement surgery, physical therapy is often necessary to ensure proper healing and regain mobility.
In this guide, we’ll explore hip replacements, post-surgery exercises, and how physical therapy can aid your recovery.
What is a Hip Replacement?
A hip replacement involves surgically removing a damaged hip joint and replacing it with a prosthetic implant. This artificial joint functions similarly to a natural hip, aiming to reduce discomfort and improve mobility over time.
What Causes the Need for a Hip Replacement?
Several factors can lead to the need for a hip replacement:
- Arthritis: Many people develop arthritis in their hips over time, particularly the elderly and athletes.
- Genetic Disorders: Some individuals are born with conditions that affect their hip joints, leading to the need for replacement surgery later in life.
- Injury: Severe damage to the hip joint from accidents, such as car crashes, can necessitate a hip replacement.
Symptoms You May Experience After a Hip Replacement
Hip replacement surgery is major, but most patients are discharged the same day thanks to advancements in surgical technology. However, some side effects are common:
- Pain: Pain in the hip joints, nearby muscles, and around the incision is typical. Your surgeon may prescribe medication to manage this discomfort.
- Trouble Walking: Post-surgery, it’s essential to take it slow. While you may be able to walk soon after, regaining a normal gait will take time and the assistance of physical therapy.
Treatments After a Hip Replacement
Post-surgery treatments are crucial for a smooth recovery. These include:
- Physical Therapy: Essential for regaining mobility, physical therapy involves stretches, exercises, and massages, along with guidance on activities to avoid.
- Medications: Pain and anti-inflammatory medications may be prescribed or recommended to manage post-surgery discomfort.
Hip Replacement Physical Therapy – Will PT Help?
Physical therapy is critical in reducing pain and aiding recovery after hip replacement surgery. Your doctor will likely recommend starting physical therapy soon after surgery.
Physical Therapy Timeline
The duration of physical therapy varies from person to person. Some may need only a month, while others might require six months or more. The timeline depends on individual healing rates and adherence to home exercise routines prescribed by the therapist.
For effective recovery, it’s essential to follow your therapist’s instructions and maintain consistency with your exercises.
You’re dealing with pain from piriformis syndrome, and it might be severe enough to affect your daily life—socially, at home, and at work. If you’re seeking relief, you’re not alone. There are various treatments available, including physical therapy.
In this article, we’ll explore the causes of your pain and offer methods of relief to help you return to your normal activities.
What Is Piriformis Syndrome?
Piriformis syndrome is a neuromuscular condition where the sciatic nerve is irritated or compressed by the piriformis muscle. This syndrome can cause significant pain in the buttocks, hip, lower back, leg, and even the feet. The interaction between the piriformis muscle and the sciatic nerve is the primary source of this pain.
What Causes Piriformis Syndrome?
The piriformis muscle is a flat, band-like muscle located in the buttocks near the top of the hip joint. It connects the lowest vertebrae to the upper leg, traveling through the “sciatic notch,” an opening in the pelvic bone that allows the sciatic nerve to pass into the leg. This muscle is crucial for lower body movement, helping to stabilize the hip joint and facilitate walking, shifting weight, and maintaining balance.
Due to its proximity to the sciatic nerve, issues with the piriformis muscle can lead to pain and other symptoms when the nerve is irritated. About 5% of sciatica cases are attributed to piriformis syndrome.
Common causes include:
- Injury
- Abnormal development or placement of the piriformis muscle or sciatic nerve
- Leg-length discrepancy
- Previous hip surgery
- Excessive exercise
- Foot problems like Morton’s Neuroma
- In many cases, the cause remains unidentified.
Who’s at Risk for Developing Piriformis Syndrome?
Piriformis syndrome can affect anyone, regardless of age, but it is more common in females than males by a ratio of 6:1, possibly due to anatomical differences. Those at higher risk include:
- Athletes: Especially those who engage in repetitive motions such as lunging or running. Prevention includes practicing proper form and completing warm-up and cool-down exercises.
- Sedentary individuals: Those who sit for long periods, either due to lifestyle or occupation, are also at risk. It’s essential to take breaks, walk, stretch, and avoid sitting with bulky objects in your back pockets.
Piriformis Syndrome Symptoms
The primary symptom of piriformis syndrome is pain, typically felt in the lower back or buttocks, which can radiate down the leg to the foot. The pain may be sharp, severe, and radiating, accompanied by tingling and numbness.
A key distinction between piriformis syndrome and sciatica is that piriformis syndrome often affects both sides of the body equally, whereas sciatica usually affects one side more than the other. Pain can be triggered by activities such as climbing stairs, running, applying pressure directly over the piriformis muscle, or sitting for extended periods.
Typical symptoms include:
- Difficulty sitting or putting weight on one side of the buttock
- Muscle spasms in the piriformis muscle
- Pain during a rectal exam
- Sciatic-type pain when the hip is moved and rotated outward against resistance
If you suspect you have piriformis syndrome, consult a healthcare professional to discuss your symptoms and potential treatments.
You’ve been managing trochanteric bursitis on your own for a while now. Activities like climbing stairs, getting up after lying down, or leaning against a wall cause intense pain and discomfort in your hips.
You’re here looking for answers, and we’re here to help. We understand how frustrating it is to live with chronic pain. Keep reading to learn more about trochanteric bursitis and how you can find relief.
What Is Trochanteric Bursitis?
Your body has over 140 bursae—small, fluid-filled sacs that help tendons, ligaments, and muscles glide smoothly over bones. Bursitis occurs when the synovial membrane of a bursa becomes inflamed, leading to excess fluid production and swelling. This condition can occur anywhere bursae are present, but it most commonly affects the shoulder, elbow, and hip.
Trochanteric bursitis specifically refers to inflammation of the trochanteric bursa, a sac that covers the greater trochanter (a bony knob near the top of your thigh bone). This bursa reduces friction during hip and knee movements.
What Causes Trochanteric Bursitis?
Trochanteric bursitis is common in women and middle-aged to elderly individuals. While the exact cause is often unknown, several factors can contribute to its development:
- Direct Impact Injuries: A fall or direct blow to the hip can cause the bursa to fill with blood, leading to inflammation.
- Overuse: Repetitive activities like running, biking, or jumping can irritate the bursa.
- Bone Spurs: These can develop on the greater trochanter and rub against the bursa.
- Tendon Injuries: Conditions like abductor tendonitis are linked to trochanteric bursitis.
- Chronic Diseases: Rheumatoid arthritis, gout, psoriasis, and thyroid disease increase the risk.
- Excessive Pressure: Poor posture or sleeping on hard surfaces can put pressure on the hip bursa.
- Obesity: Extra weight adds pressure on the hips.
- Previous Surgery: Past hip surgeries, such as replacements, increase the risk.
- Septic Bursitis: Infections in the bursa can lead to inflammation.
Trochanteric Bursitis Symptoms
The primary symptom of trochanteric bursitis is pain on the outer part of the hip, which can radiate down the thigh. This pain usually starts sharp and then becomes a persistent ache. It worsens with activities like:
- Getting out of a car or up from a chair
- Walking
- Running
- Climbing stairs
You may also experience swelling and tenderness on the affected side.
If you’re experiencing these symptoms, it’s important to seek professional advice to confirm the diagnosis and discuss treatment options.
If you’re dealing with the pain of a hip labral tear, you know just how debilitating it can be.
You might be wondering if physical therapy can help manage your hip labral tear and aid in your recovery.
This guide will cover the causes, symptoms, and diagnosis of hip labral tears, and explain how physical therapy can help you find relief.
What Is a Hip Labral Tear?
The hip joint is like a ball and socket, with the femoral head (the ball) fitting into the acetabulum (the socket). The labrum is a ring of cartilage that lines the acetabulum, ensuring smooth movement and stability in the joint.
A hip labral tear occurs when this cartilage is damaged or torn, affecting the smooth operation of the joint and causing pain.
What Causes a Hip Labral Tear?
Several factors can lead to a hip labral tear. Here are some common causes:
Injury: Athletes are particularly susceptible due to the high-impact nature of sports like hockey, football, soccer, basketball, and running. Trauma from a fall, car accident, or direct impact can also result in a tear.
Repetitive Motion: Activities that involve repetitive hip movement, such as long-distance running, hiking, baseball, or golf, can wear down the labrum over time, leading to tears.
Structural Ailments: Some individuals are born with structural abnormalities like femoroacetabular impingement (FAI), where the femoral head doesn’t fit perfectly into the socket, causing wear and tear on the labrum.
Hip Labral Tear Symptoms
Symptoms of a hip labral tear can include:
- Pain in the groin or buttocks
- Stiffness or discomfort in the hip
- Feeling unsteady on your feet
- A clicking or locking sensation in the hip
If you notice these symptoms, especially during activities like bending, moving, rotating, or exercising, it’s important to seek medical advice. Some individuals may not experience symptoms but still have a tear, making a professional diagnosis crucial.
Diagnosing a Hip Labral Tear
Diagnosing a hip labral tear involves a combination of medical history, physical examination, and imaging studies:
Medical History and Physical Examination: Your doctor will ask about your symptoms and any incidents that could have caused the injury. They’ll examine your hip for pain, tenderness, and range of motion limitations.
Special Tests: Specific tests may be performed to provoke symptoms and identify the tear, involving various movements of the hip joint.
Imaging Studies:
- X-rays: These help rule out other conditions and assess the hip bones.
- MRI: This imaging technique provides detailed images of the soft tissues, including the labrum.
- Magnetic Resonance Arthrography (MRA): Involves injecting contrast dye into the hip joint before an MRI to enhance the visibility of the labrum.
- Ultrasound: Used if MRI is not an option, providing real-time images of the hip structures.
Diagnostic Injections: An injection of local anesthetic and corticosteroid can help determine if the pain originates from the hip joint.
Arthroscopy: A minimally invasive procedure where a camera is inserted into the hip joint to directly visualize the tear and possibly repair it.
Physical Therapy for Hip Labral Tears
Physical therapy can be a highly effective treatment for managing pain and improving function after a hip labral tear. A tailored physical therapy program may include:
- Stretches: To improve flexibility and reduce stiffness.
- Strengthening Exercises: Targeting the muscles around the hip to provide better support and stability.
- Manual Therapy: Techniques to improve joint mobility and reduce pain.
- Education: Guidance on activities to avoid and how to perform movements safely.
If you’re experiencing hip pain and suspect a labral tear, consulting a healthcare professional, such as the experts at HB BodyLab, can help you get a precise diagnosis and an effective treatment plan.
Have you experienced a hip dislocation?
You might still be dealing with residual issues like intense pain and muscle spasms, which can significantly impact your daily life.
Physical therapy can accelerate the healing process and reduce the risk of recurrence.
Read on to learn about the symptoms, treatments, and benefits of physical therapy for hip dislocation.
What Is Hip Dislocation?
A hip dislocation occurs when the ball joint of your hip is forcibly ejected from its socket. Given the stability of the hip joint, dislocations are rare and typically result from trauma or severe force. The hip can dislocate in either a posterior (backward) or anterior (forward) direction.
Hip dislocations are major medical emergencies. They cause intense pain and immobilize the leg until corrected. If not treated promptly, they can lead to secondary injuries and long-term damage.
What Is Partial Hip Dislocation (Subluxation)?
A partial hip dislocation, or subluxation, means the ball joint has only partially slipped out of its socket. This condition is more common in individuals with hip dysplasia or those who have had a hip replacement.
A subluxation can range from mild to severe:
- Milder cases:
- Often due to general wear and tear.
- May be chronic or recurring.
- Sometimes can be repositioned by the individual.
- Severe cases:
- Typically caused by an injury.
- Can be as painful and disabling as a full dislocation.
- Requires professional intervention to reset.
What Causes Hip Dislocation?
Most hip dislocations are posterior, occurring when a significant force impacts the leg while:
- The knee is bent
- The hip is bent
- The hip is adducted (moved toward the opposite leg)
- The hip is internally rotated (turned inward)
High-contact sports like football or rugby, where a player lands hard on a knee, often cause posterior hip dislocations. Motor vehicle accidents also account for many posterior dislocations, typically from the knee hitting the dashboard.
Anterior hip dislocations happen when a force impacts the leg while:
- The hip is bent
- The hip is abducted (moved away from the body)
- The hip is externally rotated (turned outward)
These dislocations can occur from awkward landings in jumping sports like skiing, gymnastics, or basketball.
Hip dislocation can also occur in individuals with hip dysplasia, a developmental condition where the hip joint doesn’t fit properly in the socket.
Hip Dislocation Symptoms
Hip dislocation causes severe, acute pain, which can radiate down the leg to the knee or into the back.
Other symptoms may include:
- Muscle spasms
- Inability to walk
- Inability to bear weight on the knee
- Swelling or discoloration around the hip joint
- Weakness in the hip joint
- Numbness or tingling in the leg
- Circulation issues
If you’re experiencing any of these symptoms, it’s crucial to seek medical attention immediately to ensure proper diagnosis and treatment. Physical therapy can be a vital part of your recovery, helping you regain mobility and strength while minimizing the risk of future dislocations.
Walking is painful. The slight unevenness in your legs makes you a tad self-conscious. You wake in the mornings feeling achy and uncomfortable around your hip.
Living with hip dysplasia can be frustrating. Simply doing normal daily tasks takes a little extra work, and managing your pain has become a job in itself.
Physical therapy for hip dysplasia is a great option for pain management and body awareness.
In this guide, learn how following a hip dysplasia physical therapy protocol can help you live a more enjoyable life.
What Is Hip Dysplasia?
Hip dysplasia occurs when the acetabulum, the socket of the hip joint, is too shallow to fully support the femoral head, the top part of the thigh bone. This misalignment can lead to discomfort and mobility issues.
Most common in women, hip dysplasia, also known as developmental dysplasia of the hip (DDH), often starts from birth. Females are more susceptible due to greater ligament laxity and softer hip joints during infancy, which can cause misalignment or dislocation of the hip joint.
What Causes Hip Dysplasia?
Many individuals are born with hip dysplasia but may not notice symptoms until adulthood. It can also develop within the first year of life. While adults can develop hip dysplasia, it usually goes undiagnosed in childhood due to a lack of early symptoms.
Develops in the Womb During fetal development, increased pressure on the hips due to positioning can lead to hip dysplasia, especially in female infants who have more flexible ligaments. Breech positions and certain syndromes like Down syndrome and Ehlers-Danlos syndrome also increase the risk.
Genetics Genetics can contribute to the likelihood of developing hip dysplasia, though it’s not a direct cause. Statistics show:
- If one child has DDH, there’s a 6% chance another child will.
- If a parent has DDH, there’s a 12% chance a child will.
- If both a parent and a child have DDH, the risk of more children having DDH is 36%.
Hip Dysplasia Symptoms
Symptoms of hip dysplasia can manifest both physically and internally. Understanding these symptoms can help determine if you or someone you know might have hip dysplasia.
Physical Symptoms
- Legs of different lengths
- An outward-turning leg
- Uneven skin folds on the groin or thigh
- Leaning to one side when standing
- Limited or lost range of motion in the hip
- Limping while walking
Internal Symptoms
- Pain when sleeping on the affected hip
- Groin pain that worsens with activity
- A sensation of popping, snapping, or catching in the hip
- A stiff hip joint
If you’re experiencing any of these symptoms, seeking evaluation and treatment from a healthcare provider, such as a physical therapist, can be a crucial step in managing hip dysplasia and improving your quality of life.
Popping, grinding, and occasional pain in your hip.
You’ve been noticing these symptoms for months, and your doctor recently diagnosed the issue as hip arthritis.
Is there anything you can do to ease the pain and get back to your normal activities?
The answer is yes!
This guide provides information about arthritis of the hip and how physical therapy for hip arthritis can help ease your pain and get you back on track with everyday life.
What Is Hip Arthritis?
Hip arthritis occurs when the cartilage of the hip joint deteriorates, particularly at the head of the thigh bone and the cup-shaped socket of the pelvis where the thigh bone fits into the joint.
Since this cartilage allows your hip bone to glide smoothly inside the socket as you move, its damage or deterioration causes bone to rub against bone, leading to pain and stiffness.
What Causes Hip Arthritis?
While there is no single cause of hip arthritis, several factors can increase your risk of developing the condition, including:
- Family history of arthritis
- Aging
- Previous injury to the hip joint
- Obesity
- Developmental dysplasia of the hip (improper formation of the hip joint at birth)
Even without these risk factors, it is still possible to develop arthritis.
Hip Arthritis Symptoms
The most common symptom of hip arthritis is pain. While sudden pain is possible, discomfort usually develops slowly and worsens over time.
Additional symptoms may include:
- Pain and stiffness that are worse in the morning or after sitting or resting.
- Pain in the groin or thigh that radiates to the knee or buttocks.
- Stiffness in the hip joint that makes it difficult to bend or walk.
- Pain that flares up with vigorous activity.
- “Locking” or “sticking” of the joint.
- Decreased range of motion in the hip that makes walking difficult and may cause a limp.
- Increased joint pain during rainy weather.
- A grinding noise when moving, caused by loose fragments of cartilage and tissue interfering with the smooth motion of the hip.
Understanding these symptoms can help you identify hip arthritis early and seek appropriate treatment, including physical therapy, to manage the condition and improve your quality of life.

Sacroiliac Joint
At HB BodyLab, we understand the importance of the sacroiliac joint (SI joint), where the sacrum (tailbone) and ilium (pelvic bones) meet. The SI joint is comprised of fibrous cartilage and is covered in ligamentous tissues that offer protection. This joint allows slight gliding movements of the ilium across the sacrum on both sides.
Although the ilium bones have limited movement around the sacrum, these slight motions provide shock absorption and comfort. The fibrous cartilage prevents bone-on-bone contact and reduces the risk of bone degeneration. Additionally, the SI joint is supported by strong muscles and ligamentous tissues that aid in movement. At HB BodyLab, treating issues related to the sacroiliac joint is common for us.
Common Ailments Treated at HB BodyLab:
You’re struggling with incontinence.
Laughing, coughing, and sneezing have all become stressful experiences for you.
You’ve stopped doing activities you love out of fear of an embarrassing moment.
There are treatments that can help you — and physical therapy for incontinence is one of them.
In this guide, we will discuss the signs and symptoms of incontinence and explore treatment options that might be right for you.
What Is Urinary Incontinence?
Urinary incontinence refers to the loss of bladder control. It can range from occasionally leaking urine when sneezing or coughing to having sudden, strong urges to urinate that result in not making it to the bathroom in time.
The pelvic floor muscles are largely responsible for urinary control. These muscles create a supportive structure that helps lift and stabilize the internal organs.
These muscles also:
- Stabilize the pelvic bones
- Provide lower back support
- Control the sphincter muscles
- Assist with sexual function
Urinary incontinence is more common in women than men. The different types include:
- Stress incontinence
- Urge incontinence
- Overflow incontinence
- Functional incontinence
- Frequency incontinence
- Mixed incontinence
What Causes Incontinence?
Urinary incontinence is a symptom rather than a disease, and it can be caused by various medical issues or daily habits. It can be temporary or long-term.
Temporary incontinence can be caused by:
- Certain drinks acting as diuretics, like carbonated drinks, caffeinated drinks, and alcohol.
- Certain foods acting as diuretics, like chili peppers, chocolate, artificial sweeteners, and foods high in spice, sugar, or acid.
- Medications such as blood pressure medication, heart medications, sedatives, and relaxants.
- Medical issues like constipation or a urinary tract infection.
- Large doses of vitamin C.
Long-term incontinence can result from:
- Diabetes
- Stroke
- Multiple Sclerosis
- Enlarged prostate or prostate cancer
- Childbirth or menopause
Incontinence Symptoms
Symptoms of incontinence vary depending on the type. It’s important to discuss symptoms with your doctor to rule out other medical issues.
Stress Incontinence
Stress incontinence occurs when pelvic muscles weaken and no longer properly support the bladder and urethra. Women are more likely to develop this type of incontinence. Actions like coughing, sneezing, laughing, lifting, and bending can cause leakage. Physical therapy can help strengthen the pelvic muscles to prevent leaks.
Overactive Bladder or Urgency Urinary Incontinence
Overactive bladder incontinence (OAB) is characterized by a strong urgency to urinate, often accompanied by frequent urination. If you can’t make it to the bathroom in time, it’s classified as urgency urinary incontinence (UUI).
Overflow Incontinence
Overflow incontinence occurs when the bladder doesn’t empty properly, causing overflow and leakage. Signs include frequent, small urinations and ongoing dribbling. This type is common in males with prostate problems.
Functional Incontinence
Functional incontinence is bladder leakage not linked to pelvic floor dysfunction. It often affects people with limited mobility who can’t reach the toilet in time. Causes can include obstacles blocking access, joint or muscle weakness, dementia, or depression.
Frequency Incontinence
Frequency incontinence is often caused by infections and involves frequent urination. It can also be triggered by sensitivity to certain drinks or foods.
Mixed Incontinence
Mixed incontinence involves having two or more types of incontinence. Consulting a doctor can help determine the cause and appropriate treatment.
Urinary Incontinence Diagnosis
Diagnosing urinary incontinence requires a thorough exam by a licensed physical therapist. You will be asked about your symptoms and daily experiences. The therapist will assess:
- Pain in your pelvic floor muscles
- Muscles in your hips and lower back
- Strength, flexibility, and coordination
You may be referred to a doctor for further testing, such as:
- Ultrasound or MRI
- Urodynamic testing
Once diagnosed, treatment, including physical therapy, can begin immediately to help manage and alleviate symptoms.
If you’ve ever had a baby, you know pregnancy and childbirth can significantly alter your body.
You might not feel or look the same, and it can seem like you’ll never get back to ‘normal.’
The truth is, some changes are lasting, but you can regain proper physical function.
Postpartum physical therapy can help retrain your body to function as it should and assist in putting everything back in place.
What is Postpartum?
Postpartum refers to the period after childbirth. For new moms, this is a time of adjusting to a new normal and reclaiming their bodies.
It can also be a period of:
- Pain
- Discomfort
- Dissatisfaction with how you feel
What Causes Postpartum Recovery Difficulties?
During the nine months of pregnancy, your body undergoes significant changes.
Some challenges women face during postpartum recovery include:
- Separated abdominal muscles
- Lower belly pooch
- Back pain
- Poor posture
- Incontinence
- Frequent need to urinate
- Constipation
- Neck and shoulder pain from breastfeeding
- Decreased sexual function
Many of these issues result from diastasis recti and pelvic floor dysfunction.
Diastasis Recti Causes
If you notice an unusual gap between your abdominal muscles, you might have diastasis recti. This condition occurs as your abdomen stretches to accommodate a growing baby, causing the muscles to separate. If this separation doesn’t repair itself after birth, it can lead to a protruding belly and affect pelvic floor muscles.
You’re at higher risk of developing diastasis recti if you:
- Have had multiple pregnancies
- Gave birth to multiples (twins, triplets, etc.)
- Had poor muscle tone before pregnancy
- Gave birth later in life
- Have a small frame
Pelvic Floor Dysfunction Causes
Delivering a baby requires significant muscle effort, which can weaken or damage the pelvic floor muscles. This dysfunction can result in various uncomfortable or embarrassing symptoms.
Postpartum physical therapy can help retrain and strengthen these muscles, aiding in recovery from childbirth.
Postpartum Symptoms
Most postpartum symptoms are linked to diastasis recti and pelvic floor disorders. From back pain to a persistent “baby belly,” these conditions cause significant discomfort.
Diastasis Recti Symptoms
During pregnancy, your abdominal muscles stretch to make room for your baby, causing them to separate. Symptoms of diastasis recti include:
- A noticeable gap down the middle of your abdominal muscles
- Protruding belly below the navel
- Weak pelvic floor muscles
- Lower back pain
While many women’s muscles return to normal within six months postpartum, more than one-third experience unresolved diastasis recti.
Pelvic Floor Dysfunction Symptoms
Weak or damaged pelvic floor muscles can cause symptoms like:
- Pain during intercourse
- Frequent urination
- Urine leakage when laughing, coughing, or exercising
- Difficulty emptying your bladder
- Constipation or other bowel issues
- Pelvic organ prolapse
While these symptoms are common post-birth, they should diminish within a few weeks or months. If they persist, or you want to ensure proper recovery, you’re not alone.
3 Options for Pelvic Floor Therapy Postpartum
Pelvic floor therapy postpartum can restore your muscles, reducing or eliminating symptoms. Here’s how you can help your body recover:
1. Time
Many postpartum issues, like diastasis recti and pelvic floor dysfunction, resolve on their own within a few weeks or months. Regular check-ups with your doctor are essential to monitor your recovery.
2. Therapeutic Exercise
Specific exercises can strengthen weak muscles. Kegels, for example, are designed to strengthen pelvic floor muscles before and after childbirth. Core exercises can also improve the strength and function of these muscles. Many women find success with postpartum physical therapy, starting at a time recommended by their healthcare provider.
3. Surgery
In severe cases, surgery may be needed to repair damaged muscles. Surgery can effectively repair abdominal muscle walls in diastasis recti patients, though it comes with potential complications like wound reopening, infection, and scarring. Your doctor can help determine if surgery is necessary for your situation.
You’ve been diagnosed with pelvic floor weakness and are seeking solutions.
This condition can be uncomfortable and embarrassing, but there are effective treatments available, such as pelvic floor physical therapy exercises.
In this guide, we’ll explore the causes and symptoms of pelvic floor weakness and review the best treatment options to help you regain strength and confidence.
What is Pelvic Floor Weakness?
The pelvic floor consists of muscles and soft tissues between your pubic bone and tailbone. When these muscles, ligaments, and tissues become stretched, injured, or weakened, it results in pelvic floor weakness.
What Causes Pelvic Floor Weakness?
Pelvic floor weakness can stem from various conditions. Here are some common causes:
Childbirth
Childbirth can significantly impact pelvic floor muscles. Many women experience soft tissue injuries during and after childbirth, especially those with multiple pregnancies or who carry twins. While many women recover naturally postpartum, some may need physical therapy to address lingering issues such as:
- Painful intercourse
- Incontinence
- Pain during exercise
Old Age
As people age, their muscles and ligaments can lose flexibility, contributing to pelvic floor weakness. Inactivity and prolonged sitting can exacerbate this condition in older adults.
Obesity
Excess weight can strain muscles and ligaments, leading to pelvic floor weakness.
Heavy Lifting
Improper lifting techniques, especially in weightlifting and bodybuilding, can cause pelvic floor weakness. For instance, lifting too much weight or using incorrect form can lead to hernias.
Symptoms of a Weak Pelvic Floor
Consult your doctor or therapist to properly diagnose pelvic floor weakness and rule out other issues. Symptoms of a weak pelvic floor may include:
Urinary Issues
Incontinence is a common symptom, manifesting as loss of bladder control when sneezing, coughing, laughing, or struggling to reach the toilet in time.
Lower Back Pain
Pelvic floor weakness can cause lower back pain, often due to overcompensation by the back muscles, leading to spasms or strain.
Pain in the Pelvic Region
Pain in the pelvic region might indicate an existing injury. It’s crucial to consult a doctor or therapist before attempting any exercises or treatments at home to avoid further injury.
Treatment Options for Pelvic Floor Weakness
Pelvic Floor Physical Therapy
Physical therapy can be highly effective in strengthening pelvic floor muscles. A professional therapist will guide you through exercises designed to restore muscle function and alleviate symptoms.
Exercises
Kegel exercises, which involve contracting and relaxing pelvic floor muscles, are commonly recommended to strengthen these muscles. Other core exercises can also improve pelvic floor function.
Lifestyle Changes
Maintaining a healthy weight, staying active, and avoiding heavy lifting or improper lifting techniques can help manage and prevent pelvic floor weakness.
Surgery
In severe cases, surgery may be necessary to repair damaged muscles or tissues. Discuss with your doctor if this option is suitable for your situation.
By following a tailored physical therapy program and making lifestyle adjustments, you can strengthen your pelvic floor and improve your quality of life. Always consult with a healthcare professional before starting any treatment regimen to ensure it’s appropriate for your specific condition.
Recovering from a fractured pelvis can feel like an uphill battle. The injury itself is painful, and navigating post-surgery is no small task.
Luckily, physical therapy can help you move past your pelvic fracture, reduce your pain, and help you restore strength, mobility, balance, and function.
Read on to learn about physical therapy for a fractured pelvis, treatment options, and the best exercises to get you moving comfortably again.
What Causes a Fractured Pelvis?
A fractured pelvis can result from either low-impact or high-impact events. Common causes include:
Motor Vehicle Accidents
High-impact trauma from car accidents is a frequent cause of pelvic fractures. The force involved in collisions can cause severe trauma to the pelvis, leading to different patterns of fractures, including stable, unstable, or complex fractures involving multiple pelvic bones. Prompt medical attention is crucial to manage these injuries and prevent complications and long-term disability.
Falls from Significant Heights
Falling from a considerable height generates impact forces that cause the pelvis to absorb a tremendous amount of energy, leading to fractures. These fractures can range from stable to highly unstable, often involving injuries to organs and blood vessels.
Sports-Related Injuries
Athletic activities, especially high-impact or contact sports like football, hockey, rugby, skiing, and horseback riding, can lead to pelvic fractures. These fractures may result from direct trauma to the pelvis or as stress fractures due to repetitive impact activities such as ballet or gymnastics. Factors like bone health, training, nutrition, and biomechanical issues can increase the risk of stress fractures.
Other less common causes include osteoporosis and medical conditions that weaken bones, making them more susceptible to fractures from minimal force.
Pelvic Fracture Classification
Pelvic fractures are often classified as either:
- Stable: One break point in the pelvic ring, limited bleeding, and bones remaining in place.
- Unstable: Two or more breaks in the pelvic ring with moderate to severe bleeding.
- Complex: Complete disruption of the posterior complex, rotationally and vertically unstable, often resulting from high impact and significant tissue disruption and bleeding.
Fractured Pelvis Symptoms
The most noticeable signs of a pelvic fracture are pain and difficulty walking or standing. Severe fractures may also cause difficulty urinating or bleeding from pelvic cavities due to the fracture’s proximity to major blood vessels.
Other symptoms include:
- Pain in the groin, hip, or lower back, worsening with movement
- Abdominal pain
- Numbness or tingling in the groin or legs
- Bleeding from the vagina, urethra, or rectum
- Difficulty urinating
- Difficulty walking or standing
Additionally, pelvic stress fractures from activities like jogging may cause pain in the thigh or rear.
Treatment Options for a Fractured Pelvis
Initial Treatment
Immediate medical attention is essential for managing pelvic fractures. Treatment may include:
- Immobilization of the pelvis
- Pain management
- Surgery, if necessary, to stabilize the bones and repair any damage
Physical Therapy
Physical therapy plays a crucial role in the recovery process, helping to:
- Reduce pain and inflammation
- Restore strength and mobility
- Improve balance and function
Exercises for Pelvic Fractures
Gentle Stretching
Stretching exercises help maintain flexibility and prevent stiffness. Your therapist may recommend gentle stretches for your lower back, hips, and legs.
Strengthening Exercises
Strengthening exercises focus on rebuilding the muscles around the pelvis, hips, and lower back. These may include:
- Leg lifts
- Bridging exercises
- Core strengthening routines
Balance and Coordination
Balance exercises help improve stability and prevent falls. Activities may include:
- Standing on one leg
- Using a balance board
- Tai Chi or similar low-impact exercises
Mobility Training
Your therapist will guide you through mobility training to help you regain your ability to walk and perform daily activities. This may involve:
- Gait training
- Use of assistive devices like crutches or walkers
- Gradual increase in activity levels
Pain Management
In addition to exercises, physical therapy may include techniques for managing pain, such as:
- Manual therapy
- Heat and cold therapy
- Electrical stimulation
By following a tailored physical therapy program, you can work towards a full recovery and regain your ability to perform everyday activities comfortably and confidently. Always consult with your healthcare provider to ensure that any exercise or treatment plan is suitable for your specific condition.

Knee
At HB BodyLab, the knee joint, where the thigh (femur) and lower leg (tibia and fibula) connect, is crucial for mobility. Supported by ligaments, tendons, and muscles, it enables essential movements like walking. The femur relies on the knee joint for support during activity.
We address common knee pain sources and components. Recurring knee pain often requires physical therapy, while managing acute pain can prevent complications. Physical therapy restores knee mechanics and strengthens muscles, ensuring stable, pain-free movement. At HB BodyLab, our programs help clients achieve pain-free activity/strength.
Common Ailments Treated at HB BodyLab:
The pain, swelling, and inflammation of an IT band injury can be life-altering. As an exercise enthusiast, you’re likely looking for ways to treat your IT band injury and return to your regular activities. While dealing with an IT band injury can be overwhelming, there is hope. With the right treatment, you can recover and prevent future IT band injuries.
In this guide, we’ll discuss everything you need to know about IT band injuries, the treatment options available, and exercises to aid in recovery.
What is an IT Band Injury?
The iliotibial band (IT band) is a thick band of fibrous connective tissue that runs along the outer length of your thigh. It connects the outside portion of your tibia (the shin bone) to just below the knee joint. Along with your thigh muscles (quadriceps), the IT band provides stability to the outer knee joint during movement.
When the IT band becomes too tight, it creates friction when you bend your knee, causing the IT band and the bursa in your knee to swell. This can lead to irritation, inflammation, and pain. Injuries to the IT band are often referred to as IT band syndrome.
What Causes IT Band Injuries?
The most common cause of IT band injuries and IT band syndrome is inflammation of the IT band. Long-distance runners and cyclists are particularly at risk due to the repetitive bending of the knee. Common causes of IT band injuries include:
- Repetitive exercises involving knee bending (e.g., running, cycling, swimming)
- Rapidly increasing exercise intensity or duration
- Faulty biomechanics (e.g., having bowed legs)
- Improper training techniques
- Excessive training without adequate rest
- Muscle tightness or lack of flexibility
Common IT Band Injury Cause #1: Incorrect Training Techniques
Improper training techniques are a frequent cause of IT band injuries. Examples of these mistakes include:
- Not stretching enough before exercising
- Overexerting during workouts
- Insufficient rest between workouts
- Training in worn-out sneakers
Common IT Band Injury Cause #2: Faulty Biomechanics
Genetics and body mechanics can also make you more susceptible to an IT band injury, such as:
- Bowed legs
- Having one leg longer than the other
- Inward rotation of the leg or foot when walking or running
- Knee arthritis
- Muscle weakness in the abs, hips, or glutes
- Knee valgus (knock knees)
IT Band Injury Symptoms
Mild IT band injuries may only present symptoms before and after a workout, particularly during activities like running or cycling. Common symptoms include:
- Clicking, popping, or snapping on the outside of the knee
- Tightness at the injury site
- Mild hip pain
- Lack of flexibility
- Sharp pain, typically on the outer knee, at or below the lateral femoral epicondyle
- Tenderness near the knee when standing or bending the knee at 30 degrees
- Warmth and redness around the knee
- Pain while running, especially downhill, often felt when the foot hits the ground
Treatment Options for IT Band Injuries
Rest and Activity Modification
One of the first steps in treating an IT band injury is to rest and avoid activities that exacerbate the pain. Modify your exercise routine to include low-impact activities like swimming or cycling with reduced intensity.
Physical Therapy
Physical therapy can be highly effective in treating IT band injuries. A physical therapist can help you with:
- Stretching exercises to improve flexibility
- Strengthening exercises for the hip, glutes, and core muscles
- Techniques to correct faulty biomechanics
- Soft tissue massage and foam rolling to reduce tightness
Medications
Over-the-counter pain relievers, such as ibuprofen or acetaminophen, can help reduce pain and inflammation. In more severe cases, your doctor may prescribe stronger medications.
Injection Therapy
For persistent pain and inflammation, corticosteroid injections may be recommended. These injections can provide relief by reducing inflammation around the IT band.
Exercises to Aid Recovery
Stretching Exercises
- IT Band Stretch: Stand with one leg crossed over the other and lean away from the affected side to stretch the outer thigh.
- Hip Flexor Stretch: Kneel on one knee and push your hips forward to stretch the front of the hip.
Strengthening Exercises
- Side-Lying Leg Raises: Lie on your side with your affected leg on top and lift it towards the ceiling.
- Clamshells: Lie on your side with your knees bent and lift your top knee while keeping your feet together.
Foam Rolling
Use a foam roller to massage the outer thigh and hip area. This can help release tightness and reduce inflammation.
By following these treatment options and incorporating the recommended exercises, you can recover from an IT band injury and prevent future occurrences. Always consult with a healthcare professional or physical therapist before starting any new exercise regimen to ensure it is appropriate for your specific condition.
You’re facing a knee replacement or perhaps you’ve already had the surgery. You know pain all too well and want to explore your options for relief and recovery. Regaining mobility and functionality in your knee is crucial, so understanding your treatment and recovery choices is essential.
This guide will cover knee replacement surgery and the various treatment options available to help you on your path to recovery.
What is Knee Replacement Surgery?
Also known as knee arthroplasty, knee replacement surgery involves replacing the damaged weight-bearing parts of your knee with artificial components. This procedure aims to alleviate severe joint pain and restore the knee’s function.
What Causes the Need for a Knee Replacement?
Several factors can lead to the need for knee replacement surgery, including:
- Arthritis: The most common cause, arthritis can severely damage the knee joint, making replacement necessary to relieve pain and improve quality of life.
- Injury: Major knee injuries, such as fractures or torn ligaments, can damage the knee so severely that replacement becomes the best option.
- Blood Disorders: Conditions like hemophilia or blood clots can cause bone death, necessitating knee replacement.
- Deformity: Genetic abnormalities, such as severe varus (bow-legged) or valgus (knock-kneed) deformities, can require surgery to correct knee alignment and function.
Knee Replacement: Symptoms After Surgery
Post-surgery, patients may experience a variety of symptoms. While each patient’s recovery is unique, common symptoms include:
- Pain: Often moderate to severe initially, pain typically decreases over time.
- Stiffness: Caused by swelling or lack of movement, stiffness can be managed with prescribed exercises and rehabilitation.
- Swelling: Elevating the knee and applying ice can help reduce swelling.
Knee Replacement: Treatment Options
Your doctor will provide a treatment plan tailored to your needs, often including physical therapy as a crucial component of rehabilitation.
Pain Management
Managing pain is vital to recovery. Your doctor may recommend:
- NSAIDs (e.g., ibuprofen)
- Over-the-counter pain relievers (e.g., acetaminophen)
- Opioid pain relievers (e.g., tramadol or oxycodone)
- Extended-release local anesthetic
- Physical therapy
Your pain management plan will be based on your individual circumstances and pain levels post-surgery.
RICE Treatment
RICE stands for rest, ice, compression, and elevation. This approach can help manage swelling and is often suggested by surgeons and physical therapists.
Physical Therapy
Physical therapy is a cornerstone of knee replacement recovery. It can lead to:
- Less pain
- Increased mobility
- Improved physical function
A physical therapist will guide you through exercises designed to strengthen your knee, improve flexibility, and restore function.
By understanding these aspects of knee replacement surgery and the available treatment options, you can take proactive steps toward a successful recovery and a return to your normal activities. Always consult with your healthcare provider to develop a plan tailored to your specific needs.
Is your teen experiencing intense leg pain, and you can’t seem to pinpoint the cause? You might suspect growing pains or jumper’s knee but aren’t sure how to alleviate their symptoms. You’re not alone.
Ten percent of adolescents go through this. The technical term for this condition is Osgood-Schlatter disease.
In this guide, we’ll explain Osgood-Schlatter disease and how to help your teen find relief.
What is Osgood-Schlatter Disease?
Osgood-Schlatter disease isn’t actually a disease but a common knee injury in adolescents. It occurs where the tendon from the kneecap (patellar tendon) attaches to the shinbone (tibia), known as the tibial tuberosity. This condition involves swelling, inflammation, and irritation of the area below the knee, sometimes resulting in a painful bump just under the kneecap.
What Causes Osgood-Schlatter Disease?
Osgood-Schlatter disease is caused by the continuous pulling of the tendons in the knee. Two of the most common causes are:
Growth Spurts
During adolescence, bones grow faster than muscles and tendons, causing them to become tight. As the body goes through growth spurts, the muscles, bones, and tendons shift and grow, putting more stress on the patellar tendon and growth plate, leading to pain and inflammation.
Sporting Activities
Athletic adolescents, especially boys aged 10 to 15, are most commonly affected. Sports that involve a lot of running and jumping — like basketball, soccer, track, and ballet — cause the leg muscles to pull on the patellar tendon, which in turn pulls on the growth plate. This repeated stress can lead to Osgood-Schlatter disease, often referred to as growing pains or jumper’s knee.
It’s important to note that Osgood-Schlatter disease can persist from childhood into adulthood, and treatment may vary for those who continue to experience symptoms.
Osgood-Schlatter Symptoms
The symptoms of Osgood-Schlatter disease typically affect the area just below the kneecap. Common symptoms include:
- Pain: Usually develops slowly over time but can occur suddenly.
- Redness, swelling, warmth, and tenderness at the top of the shin.
- Tightness in the quadriceps muscle.
- Loss of range-of-motion in the knee.
- Impaired balance.
- A bony bump that forms at the top of the shinbone.
- Discomfort when bending the knee during activities like squatting, sitting, or walking up and down stairs.
Symptoms usually occur in one knee but can affect both.
Understanding these symptoms and their causes can help you better manage your teen’s condition and explore appropriate treatment options, including rest, ice, compression, and elevation (RICE), along with physical therapy. Consult with a healthcare professional for a tailored treatment plan to ensure a smooth recovery.
Every step you take during your run or walk brings a clicking sound, a grinding sensation, and a dull ache that lingers for hours. Runner’s knee has been a persistent problem, slowing you down and making every workout a painful experience.
You don’t have to live with this discomfort. Understanding what causes runner’s knee and exploring treatment options can help you get back on track.
What Is Runner’s Knee?
Runner’s knee, or patellofemoral pain syndrome, is characterized by pain beneath your kneecap (patella). The main symptom is pain around or behind the kneecap, especially during activities like running, squatting, or sitting for long periods. It primarily affects those who frequently exercise, placing stress on the patellofemoral joint.
What Causes Runner’s Knee?
Several factors can contribute to runner’s knee, including:
- A high-riding kneecap within the joint
- Weak thigh muscles
- Tight hamstrings or Achilles tendons
- Poor foot support
The most common cause is excessive exercise that puts pressure on the knee joint. Activities like walking, running, squatting, and jumping can overwork the knees, leading to runner’s knee.
Some specific causes include:
Overtraining Exercise can be addictive, and pushing your body to run faster or more often without adequate rest can cause tissue breakdown. Without proper recovery, muscles can’t heal, leading to runner’s knee.
Poor Alignment of the Kneecap The kneecap sits in a groove formed by the femur and should glide smoothly when you bend and straighten your knee. If it moves incorrectly, it can cause friction, resulting in inflammation and pain.
Weak Leg Muscles Quadriceps and hip flexors help keep the kneecap in place. When these muscles are weak, the kneecap can move in multiple directions, scraping the surrounding cartilage and causing irritation.
Runner’s Knee Symptoms
Symptoms of runner’s knee include:
- Discomfort when walking up or down hills or stairs
- Pain during exercise
- Pain after sitting with a bent knee for a long time
- Pain when squatting
Additional symptoms may include:
Painful Kneecap Tenderness when touching the kneecap can be a sign of runner’s knee, although it might also indicate other injuries if pain is localized to the bones or the side of the patella.
Burning Pain Under the Kneecap A sharp, burning pain beneath the kneecap is the hallmark of runner’s knee. Pain on the side or top of the kneecap might suggest a different knee problem.
Knee Crepitus Clicking, grinding, and crunching sensations in the knee, known as knee crepitus, often accompany runner’s knee. These symptoms can worsen with specific movements or after resting for long periods.
If you suspect you have runner’s knee, consult with a healthcare professional who may perform an MRI to diagnose the condition and determine the best treatment plan. With proper care, including rest, targeted exercises, and physical therapy, you can overcome runner’s knee and return to your regular activities pain-free.
Arthroscopic knee surgery is the most frequently performed knee surgery, with nearly two million procedures annually in the U.S. This minimally invasive surgery addresses various knee issues such as ACL injuries, meniscal tears, patella injuries, fractures, and tendon tears.
Whether you’ve undergone arthroscopic knee surgery or are considering it, understanding the recovery process is essential. This guide will cover arthroscopic knee surgery and how physical therapy can aid in your recovery.
What Is Arthroscopic Knee Surgery?
Arthroscopic knee surgery is a common procedure that enables doctors to diagnose and treat a range of knee injuries using a tiny camera and specialized instruments. The surgery involves making small incisions to insert the camera, which projects images onto a monitor, allowing the surgeon to navigate and perform the necessary procedures. This approach results in less pain, reduced joint stiffness, and a shorter recovery time compared to traditional surgery.
What Causes the Need for Arthroscopic Knee Surgery?
Doctors may recommend arthroscopic knee surgery when knee pain does not improve with nonsurgical treatments like rest, ice, and non-steroidal anti-inflammatory drugs. Some common reasons for undergoing this procedure include:
ACL Reconstruction The anterior cruciate ligament (ACL) is crucial for knee stability. An ACL injury often causes the knee to give out. Many patients opt for arthroscopic ACL surgery to restore knee function.
Lateral Release Lateral release surgery realigns the kneecap (patella) when it becomes dislocated due to being pulled outside its groove, causing pain. The procedure loosens the ligaments pulling the kneecap outward, restoring proper alignment.
Meniscus Repair The meniscus is a C-shaped cartilage pad that acts as a shock absorber between the knee bones. Meniscus tears are common, especially among athletes. Arthroscopic meniscus repair can alleviate pain and restore normal knee function.
Symptoms of Knee Injuries That Might Benefit from Arthroscopic Surgery
Symptoms indicating the need for arthroscopic knee surgery include:
- Popping or crunching noises
- Weakness or instability
- Swelling and stiffness
- Redness and warmth to the touch
- Inability to fully straighten the knee
Benefits of Physical Therapy After Arthroscopic Knee Surgery
Restore Range of Motion After arthroscopic knee surgery, you may experience a loss of range of motion, leading to stiffness and difficulty performing daily activities. Physical therapy helps improve your ability to stand, walk, and bend your knee, maintaining your range of motion and preventing further injury.
Education Education is a crucial aspect of post-surgery physical therapy. A physical therapist will teach you how to maintain proper posture throughout the day, placing the correct amount of pressure on your knee. This includes guidance on sitting, standing, walking, climbing stairs, and performing your favorite activities.
By understanding the role of physical therapy in your recovery from arthroscopic knee surgery, you can take proactive steps to regain mobility and reduce pain, ultimately enhancing your quality of life.
Does a recent ACL injury have you feeling like you may never get back to normal? Has it disrupted your active lifestyle, making you wonder if you’ll ever be back in the game? There is hope.
With the right treatment, many people can recover from ACL injuries and return to an active lifestyle. In this guide, we’ll cover everything you need to know about ACL injuries and how exercise and rehabilitation can help you overcome them.
What is an ACL Injury?
The anterior cruciate ligament (ACL) is one of the major ligaments in your knee. This crucial band of tissue connects your shinbone (tibia) to your thigh bone (femur), providing stability to the knee by preventing the shin from sliding forward.
ACL injuries are common knee injuries that involve overstretching or tearing the ligament. These injuries occur when the knee extends beyond its normal range of motion or twists sharply, potentially leading to partial or complete tears. A torn ACL can cause your knee to “give out” during certain activities.
What Causes ACL Injuries?
ACL injuries typically occur during activities that place excessive stress on the knee, especially those involving frequent twisting motions and sharp movements, such as football, soccer, basketball, and gymnastics. These sports often require movements that cause the femur to pivot on the tibia.
High-impact sports, like football, can cause ACL injuries through direct hits to the knee, where the tibia is driven forward and the femur backward. Sometimes, a “pop” or “snap” can be heard at the time of injury.
ACL injuries also occur during automobile accidents, workouts, or certain jobs. Studies show that women are more likely to suffer ACL injuries than men.
Types of ACL Injuries
Healthcare professionals classify ACL injuries into three categories:
Grade One
This involves minimal to mild damage, where the ligament is stretched but still maintains knee joint stability. Grade one injuries are considered ACL sprains.
Grade Two
Rare and involving partial tears, grade two injuries occur when fibers in the ACL are partially torn and the ligament is stretched.
Grade Three
The most severe type, grade three injuries are complete tears where the ligament fibers are fully torn, providing no stability to the knee.
ACL Injury Symptoms
Symptoms of an ACL injury vary in severity but commonly include:
- A popping or snapping sound at the moment of injury
- Sudden sharp pain following the injury
- Swelling immediately after the injury or within 24 hours, lasting up to a week
- Aching pain in the knee that worsens with walking, running, or climbing stairs
- Instability or a feeling that the knee will “give out” during walking or pivoting
- Numbness down the affected leg (in serious cases)
- Tenderness around the knee joint
Unlike many injuries that heal on their own, ACL injuries rarely do. Without treatment, they can lead to long-term negative effects on your knee.
Treatment Options
Rest and Ice Initial treatment often involves resting the knee and applying ice to reduce swelling.
Physical Therapy A physical therapist will design a rehabilitation program to restore strength, stability, and range of motion to your knee.
Bracing A knee brace can provide additional support during recovery.
Surgery For severe ACL injuries, particularly grade three tears, surgery might be necessary to reconstruct the ligament.
Prevention Tips
To prevent ACL injuries, consider these tips:
- Strengthen your leg muscles, particularly the quadriceps and hamstrings.
- Practice proper technique during sports and exercise.
- Use appropriate footwear for your activities.
- Incorporate flexibility exercises into your routine.
- Avoid overtraining and allow time for rest and recovery.
By understanding the nature of ACL injuries and following a comprehensive treatment and rehabilitation plan, you can recover effectively and return to your active lifestyle.
Knee pain can significantly impact your daily life. If you have patellar tendonitis, even simple activities like walking or climbing stairs can become painful.
Patellar tendonitis, also known as Jumper’s Knee, is an injury that can be treated, providing relief from pain and discomfort. This guide will help you understand this condition and explore treatment options available to you.
What is Patellar Tendonitis?
Patellar tendonitis involves a strain on the tendon that connects the patella (kneecap) to the tibia (shinbone). This condition is characterized by pain and inflammation in the tendon between the kneecap and shinbone, resulting from stress or strain due to repeated high-impact activities. In severe cases, the tendon may develop tears, leading to further pain and inflammation.
What Causes Patellar Tendonitis?
Patellar tendonitis is often associated with sports-related activities, but you don’t need to be a professional athlete to experience it. Common causes include:
- Physical Activity: High-impact activities such as running, jumping, and weight lifting can place additional stress on the patellar tendon. Sports like basketball, volleyball, and tennis often lead to this condition due to the repetitive strain they cause on the knees.
- Tight Muscles: Tight hamstrings and quadriceps can increase the strain on the knee joint and tendons, leading to injuries like patellar tendonitis. Proper stretching and muscle conditioning are essential to prevent such injuries.
- Chronic Illness: Certain chronic illnesses can weaken tendons by disrupting blood flow, making them more susceptible to injuries. Conditions such as kidney failure, metabolic diseases (e.g., diabetes), and autoimmune disorders (e.g., lupus, rheumatoid arthritis) can contribute to the development of patellar tendonitis.
Patellar Tendonitis Symptoms
The primary symptoms of patellar tendonitis include:
- Pain: Pain is usually the first noticeable symptom, typically felt behind the bottom of the kneecap. It can range from mild discomfort to severe pain, depending on the extent of the injury. Pain may be experienced at the top of the tibia when the knee is bent and at the bottom of the knee when the knee is straight.
- Weakness: Weakness in the affected knee or leg is common. If the tendon has partially torn, the joint may become unstable, limiting your ability to perform certain activities.
- Swelling: While not the most common symptom, mild swelling can occur behind the patella where the knee and tibia meet. Significant swelling could indicate a more severe injury, warranting immediate medical attention.
Treatment Options for Patellar Tendonitis
There are several treatment options available for patellar tendonitis:
- Rest and Ice: Reducing activity and applying ice to the affected area can help manage pain and swelling.
- Physical Therapy: A physical therapist can design a rehabilitation program to strengthen the knee and surrounding muscles, improve flexibility, and reduce strain on the patellar tendon.
- Medications: Over-the-counter pain relievers and anti-inflammatory medications can help manage pain and inflammation.
- Supportive Devices: Using knee braces or supportive straps can help alleviate stress on the tendon during activities.
By understanding the causes, symptoms, and treatment options for patellar tendonitis, you can take steps to manage your condition and return to your normal activities with less pain and discomfort.
The dull ache keeps you awake at night. Descending stairs is excruciating, and the grinding sound when you straighten your leg is unbearable.
You want to get back to living a normal life but are unsure where to start in overcoming the pain of chondromalacia.
We’re here to help.
In this guide, we’ll discuss everything you need to know about chondromalacia patella, including treatment options, exercises, and more.
What Is Chondromalacia Patella? Your body is full of joints cushioned by articular cartilage, a rubbery, tough tissue that covers the ends of bones inside your joints. This cartilage cushions your bones and allows them to glide smoothly over one another as you move.
Over time, this cartilage can soften or deteriorate, leading to a condition called chondromalacia. As the cartilage continues to break down, the bones rub together, resulting in pain and decreased mobility.
Chondromalacia can affect any joint but most commonly affects the cartilage under your patella (kneecap), a condition known as chondromalacia patella.
What Causes Chondromalacia? Chondromalacia can occur for several reasons, with the most common causes being:
- Abnormal positioning of the kneecap
- Tightness or weakness of the muscles associated with the knee
- Excessive activity involving the knee
- Flat feet
- Knee injuries
- Improper knee alignment
Who Is at Risk for Chondromalacia? While athletes who put repeated stress on their knees are commonly diagnosed with chondromalacia, others at risk include:
- Young adults
- Women
- People with jobs requiring excessive knee bending
- Individuals with previous kneecap injuries, fractures, or dislocations
What Are the Symptoms of Chondromalacia? Pain is the primary symptom of chondromalacia. Similar to runner’s knee, individuals with chondromalacia may experience:
- Knee tenderness
- Swelling and inflammation around the kneecap
- Pain that increases after sitting for long periods
- Pain when walking up or down stairs or getting out of a chair
- A grinding or cracking sensation when straightening the knee
Pain can also occur after prolonged periods of activity that place extreme pressure on the knees.
If you suffer from knee pain or other symptoms of chondromalacia, contact your doctor. Early treatment may prevent further damage to the cartilage and ease your symptoms.
How Is Chondromalacia Patella Treated? Your physician will likely schedule an assessment to determine the right treatment plan for your symptoms.
In most cases, treatment begins with conservative methods. If these do not relieve symptoms, more serious treatment or surgery may be necessary.
Non-Surgical Treatment Physical therapy and activity modification are the most common treatments for chondromalacia. Treatments that may be combined with these include:
- Anti-inflammatory medications (e.g., ibuprofen)
- Bracing
- Orthotics
- Injection therapies, such as corticosteroids or viscosupplementation
If non-surgical treatments do not reduce pain or dysfunction, your physician may recommend surgical treatment.
Surgical Treatment Arthroscopy is the most common type of surgery for chondromalacia. Your physician may recommend arthroscopy to examine the cartilage around your kneecap. If the cartilage is softened or shredded, the surgeon will remove the damaged layers during surgery.
If realignment is necessary to reduce wear and tear on your knee cartilage, this may also be performed during surgery.
With the right treatment plan, you can manage chondromalacia and return to your normal activities with less pain and discomfort.
Knee stiffness, pain, and swelling have become a constant part of your life. You’ve had enough and want to get back to your everyday activities without discomfort.
You’re curious about the cause and how to alleviate the constant discomfort, but without a proper diagnosis, finding relief can be challenging.
We’re here to help.
In this guide, we’ll cover everything you need to know about knee arthritis, from types and symptoms to treatment options and everything in between.
What is Knee Arthritis?
The knee is the largest and strongest joint in the human body. It’s a hinge joint composed of bones, cartilage, ligaments, and tendons. The knee joint connects three bones:
- The femur (upper leg bone)
- The tibia (shin bone)
- The patella (kneecap)
To understand knee arthritis, it’s essential to understand these components:
- Articular Cartilage: Covers the ends of the bones inside the joint, allowing them to glide smoothly.
- Meniscus: Cartilage between the femur and tibia, acting as a shock absorber.
- Ligaments: Connect the bones and provide stability.
- Tendons: Connect muscles to bones, facilitating movement.
Knee arthritis occurs when any of these components are affected by inflammation, degeneration, or damage, depending on the type of arthritis you have.
What Causes Knee Arthritis?
The most common types of knee arthritis are:
- Osteoarthritis (OA): A degenerative disease affecting bones, cartilage, and synovium.
- Rheumatoid Arthritis (RA): An autoimmune disorder affecting multiple joints, including the knees.
Other less common types include post-traumatic arthritis, reactive arthritis, gout, and infectious arthritis. Causes, symptoms, and treatment options vary based on the type of arthritis.
Osteoarthritis in the Knee
OA is caused by the breakdown of joint cartilage. Over time, the changes in the cartilage cause changes in the bone, which develop slowly and worsen. Common causes include:
- Age: Decreased ability to heal cartilage with age.
- Gender: Women over 55 are more at risk.
- Repetitive Stress Injuries: Activities that involve lifting, squatting, or kneeling.
- Sports: Athletes in high-impact sports.
Rheumatoid Arthritis in the Knee
RA is an autoimmune disorder where the body attacks the joint lining and surrounding tissues. In the knees, this causes inflammation and swelling, damaging the cartilage and ligaments over time. RA gets worse over time and can affect multiple joints.
Knee Arthritis Symptoms
Common symptoms of knee arthritis include:
- Stiffness
- Pain
- Loss of function
- Swelling
Symptoms of Osteoarthritis in the Knee
- Scraping feeling when moving the knee
- Pain during or after activity
- Joint stiffness after resting
- Limited range of motion
- Clicking or cracking sounds
- Muscle weakness
- Instability or buckling
Symptoms of Rheumatoid Arthritis in the Knee
- Stiffness and swelling in both knees
- Weakness
- Warmth in the knee joints
- Difficulty walking or climbing stairs
- Fatigue after activities
Treating Knee Arthritis
Non-Surgical Treatment
Most cases of knee arthritis begin with non-surgical treatments, including:
- Physical Therapy: Helps maintain range of motion and strengthen the knee.
- Medication: Anti-inflammatory drugs to reduce pain and swelling.
- Bracing: Provides support and reduces strain.
- Orthotics: Improve alignment and relieve pain.
- Injection Therapies: Corticosteroids or viscosupplementation to reduce inflammation.
Surgical Treatment
If non-surgical treatments don’t provide relief, surgery may be necessary:
- Arthroscopy: A minimally invasive surgery to examine and treat joint damage.
- Knee Replacement: Replaces damaged parts of the knee with artificial components.
With the right treatment plan, you can manage knee arthritis and return to your normal activities with less pain and discomfort. If you’re experiencing symptoms, consult your doctor for a proper diagnosis and personalized treatment plan.
You’ve recently had knee surgery and now you’re dealing with pain and stiffness, making it difficult to regain full mobility. These symptoms could be due to contractures, which are common after knee surgery. We understand how frustrating this can be, and we’re here to help.
In this guide, we’ll cover everything you need to know about knee contractures, including their symptoms, causes, exercises, and more.
What Are Contractures After Knee Surgery?
Contractures occur when tendons, joints, muscles, or other tissues shorten or tighten, leading to stiffness or deformity. This happens because the knee flexors fail to lengthen alongside the bone, causing the knee capsule to become rigid and limiting its movement.
Contractures are also known as flexion deformities or arthrofibrosis of the knee. They result from the hardening and shortening of muscles and connective tissues.
What Causes Contractures After Knee Surgery?
Knee contractures typically result from excessive scar tissue forming within the knee’s joints and soft tissues. They are common after total knee arthroplasties (TKA) or anterior cruciate ligament reconstruction surgeries, making them one of the most frequent complications of total knee replacement.
Several factors can cause knee contractures after surgery:
- Insufficient pain control
- Poor motion prior to surgery
- Excessive scar formation
Certain risk factors may increase the likelihood of developing knee contractures.
Risk Factors for Knee Contractures
Factors that may increase the risk of knee contractures include:
- Inherited disorders (e.g., muscular dystrophy)
- Reduced mobility or lack of use
- Nerve damage
- Stroke
- Tenosynovitis
- Muscle or bone injuries
- Scarring from injuries or burns
Contractures occur as part of the body’s natural response to trauma, such as injury or surgery, by creating scar tissue. Sometimes, the body continues to produce scar tissue even after it should stop, causing dense, fibrous tissue to bind down joints and restrict knee movement.
Symptoms of Contractures After Knee Surgery
Common symptoms associated with contractures include:
- Pain
- Morning stiffness
- Decreased knee flexion
- Loss of knee extension
- Walking with a bent knee
- Weak quadriceps (the muscle at the front of the thigh that helps extend the leg)
Treatment for Contractures After Knee Surgery
Various treatment options are available for contractures after knee surgery, including:
- Physical therapy (PT)
- Manipulation under anesthesia
- Arthroscopic arthrolysis
- Open debridement
- Revision surgery
The appropriate treatment depends on the cause of the stiffness and the time elapsed since the knee surgery. Your doctor will recommend the best treatment for your situation.
Post-Total Knee Replacement Arthroscopic Arthrolysis
If you experience knee pain, swelling, redness, or loss of motion (contractures) that don’t improve over time, your surgeon might suggest arthroscopic arthrolysis. Using a small tool called an arthroscope, the surgeon will inspect the knee through a small incision and remove any dense fibrous tissue causing the contractures.
Manipulation Under Anesthesia
Manipulation under anesthesia is another effective treatment. Under general anesthesia, your doctor will move your knee in various directions to break up scar tissue and improve your range of motion.
Open Debridement
In open debridement, the surgeon removes dead or infected tissue contributing to the knee contractures.
Revision Knee Replacement
Revision surgery is a last resort when other treatments fail. The surgeon will adjust the bone cuts and the size of the new replacement to improve the knee’s range of motion.
By understanding knee contractures and the available treatment options, you can take steps toward reducing pain and regaining mobility. Always consult with your doctor to determine the best course of action for your specific condition.
You’re tired of dealing with pain caused by knee bursitis and want to explore all your treatment options. Fortunately, there are many ways to help ease your symptoms and aid in recovery, including physical therapy for knee bursitis.
In this guide, we will cover everything you need to know about knee bursitis and what type of treatment is right for you.
What is Knee Bursitis?
Near your knee joint, there are several small fluid-filled sacs called bursae. These sacs help reduce friction and pressure between your bones, muscles, tendons, and skin around your knee joints. The inflammation of one or more bursae is referred to as knee bursitis.
Knee bursitis most commonly occurs in two places:
- Over the kneecap
- Below the knee joint on the inner side of your knee
Knee bursitis can be painful and limit the mobility of your knee. Medical care may be required to help reduce inflammation and restore mobility to the knee joint.
What Causes Knee Bursitis?
The cause of knee bursitis can vary. Studies show that there is a high concentration of knee bursitis in workers exposed to heavy workloads and frequent kneeling.
Other causes of knee bursitis include:
- A direct injury to the knee
- Bacterial infections in bursae
- Complications due to osteoarthritis, gout, or rheumatoid arthritis in the knee
- Any form of activity that is strenuous to the knee joint
Knee Bursitis Symptoms
Symptoms of knee bursitis can depend on which bursa is inflamed and what is causing the inflammation. Typical symptoms of an inflamed bursa may include the affected area being:
- Warm to the touch
- Tender
- Swollen
Your pain can increase with movement and pressure and can also be felt at rest.
When knee bursitis is caused by overuse or strenuous activity, like frequent kneeling on hard surfaces, symptoms typically come on gradually and worsen over time. If knee bursitis is the result of a direct blow to the knee, symptoms will develop rapidly.
If you are experiencing symptoms and develop a fever, consult with a doctor immediately, as you may be experiencing a bacterial infection in one or more of your bursa. Your doctor will also need to rule out other potential knee injuries.
Treatment Options for Knee Bursitis
Treatment for knee bursitis can range from self-care practices to more intensive medical treatments, depending on the severity and cause of the inflammation.
Self-Care and Home Remedies
- Rest: Avoid activities that aggravate the knee bursitis.
- Ice: Apply ice packs to the knee to reduce swelling and pain.
- Compression: Use a knee brace or compression wrap to reduce swelling.
- Elevation: Keep your knee elevated above the level of your heart to reduce swelling.
Medical Treatments
- Medications: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or aspirin can help reduce pain and inflammation.
- Aspiration: In some cases, a doctor may drain the bursa fluid to reduce swelling and relieve pain.
- Corticosteroid Injections: These can reduce inflammation and pain quickly.
Physical Therapy
Physical therapy can play a crucial role in treating knee bursitis by improving strength, flexibility, and joint stability. A physical therapist can design a personalized exercise program that includes:
- Stretching Exercises: To improve flexibility and reduce tension around the knee joint.
- Strengthening Exercises: To build strength in the muscles around the knee, providing better support and reducing stress on the bursa.
- Activity Modification: Learning how to modify activities that may be causing or aggravating knee bursitis.
When to See a Doctor
If your symptoms persist despite home treatment, or if you experience a fever along with knee pain and swelling, consult a doctor. Early treatment can prevent complications and speed up recovery.
By understanding knee bursitis and the available treatment options, you can take proactive steps to reduce pain and restore your knee’s function. Always consult with your healthcare provider to determine the best treatment plan for your specific condition.
Is that fluid-filled lump behind your knee causing you constant pain? Maybe you’re finding it difficult to walk. You might have trouble squatting down. You’ve noticed your leg is swollen. These painful symptoms, plus many others, might mean you have a Baker’s cyst.
Luckily, there are many treatments for Baker’s cysts, including physical therapy.
Learn how a variety of physical therapy exercises can help to:
- Reduce your pain and swelling
- Increase your range of motion
- Strengthen your weak knee muscles
What Is a Baker’s Cyst?
Most commonly found behind the knee, a Baker’s cyst is a fluid-filled lump that results from a damaged joint. You might hear Baker’s cysts referred to as popliteal cysts or synovial cysts. When the knee joint is damaged or inflamed, extra synovial fluid is produced and becomes trapped in the joint, forming a cyst behind the knee.
What Causes Baker’s Cyst?
Swelling from damaged joints and structures in the knee causes fluid to create a soft lump at the back of the knee. Knee damage can happen for many reasons:
- Osteoarthritis
- Rheumatoid arthritis
- Meniscus or ligament tears
- Inflammation
- Gout
ARTHRITIS IN THE KNEE
All forms of arthritis can cause the fluid build-up that can become a Baker’s cyst, but most commonly Baker’s cysts come from rheumatoid arthritis or osteoarthritis. These degenerative forms of arthritis cause the body to respond with inflammation. Rheumatoid arthritis causes an increased production of synovial fluid from inflammation around the knee joints.
KNEE TEARS
Baker’s cysts are more frequent with meniscus tears than other knee tears, but any tearing and damage to knee ligaments can lead to a Baker’s cyst. Knee tears most often happen:
- From being hit in the side of the leg
- When falling directly on the knee
- When shifting the leg incorrectly
GOUT
An inflammatory form of arthritis, gout often presents itself as:
- Severe knee pain, often leading to Baker’s cyst
- Pain in other joints (ankles, elbows, wrists)
- Redness
- Reduced range of motion
- Swelling
The flare-ups from gout usually happen at night and can be increased by:
Diets high in:
- Alcohol
- Seafood
- Meat
- Fructose
People with:
- Obesity
- Kidney issues
- Hypertension
- Cardiovascular disease
Baker’s Cyst Symptoms
Many people realize they have a Baker’s cyst because it is clearly visible. As the cyst begins to fill with fluid, it grows. It might be as small as a marble or as large as a golf ball, depending on how quickly you notice it.
Besides the noticeable lump, other symptoms of a Baker’s cyst include:
- Painful flexion or extension of the knee
- Stiffness of the knee joint
- Swelling of the knee or leg
Although the obvious lump might leave you sure you’re suffering from a Baker’s cyst, only a doctor can properly diagnose you. They’ll likely first rule out a blood clot and order imaging to get a better look at the cyst.
KNEE PAIN
We know knee pain can happen for many reasons. Whether it be from arthritis, internal derangement, or inflammation, the damage to the knee joint can quickly lead to Baker’s cyst. If you’re having trouble bending or extending your knee or are experiencing pain in your knee joint, consult a doctor to rule out Baker’s cyst.
STIFFNESS AROUND THE KNEE
If you’re suffering from a Baker’s cyst, the increased fluid and growing sac can quickly cause stiffness around your knee joint, making it difficult to move your knee as easily, even if there is no pain.
SWELLING OF THE KNEE OR LEG
Excess fluid and inflammation that results from a Baker’s cyst can cause visible swelling to both the knee and the leg. If you notice any swelling, visit your doctor.
Treatment Options for Baker’s Cyst
Physical Therapy
Physical therapy can play a key role in treating Baker’s cysts by improving strength, flexibility, and joint stability. A physical therapist can design a personalized exercise program that includes:
- Stretching Exercises: To improve flexibility and reduce tension around the knee joint.
- Strengthening Exercises: To build strength in the muscles around the knee, providing better support and reducing stress on the bursa.
- Activity Modification: Learning how to modify activities that may be causing or aggravating the cyst.
Medical Treatments
- Medications: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or aspirin can help reduce pain and inflammation.
- Aspiration: In some cases, a doctor may drain the cyst fluid to reduce swelling and relieve pain.
- Corticosteroid Injections: These can reduce inflammation and pain quickly.
- Surgery: In rare cases, surgery may be required to remove the cyst.
When to See a Doctor
If your symptoms persist despite home treatment, or if you experience a fever along with knee pain and swelling, consult a doctor. Early treatment can prevent complications and speed up recovery. By understanding Baker’s cysts and the available treatment options, you can take proactive steps to reduce pain and restore your knee’s function. Always consult with your healthcare provider to determine the best treatment plan for your specific condition.
Something is up with your knee. You can hardly straighten it, and it hurts to even put pressure on it, let alone try to walk. You may be suffering from a painful MCL sprain.
We cover the details of all things MCL, including how physical therapy for an MCL sprain can help you find relief and get back on your feet.
What Is an MCL Sprain?
The MCL, or medial collateral ligament, is the ligament that keeps your tibia (shin bone) in place. An MCL sprain can occur when your MCL is stretched or torn and may result in a partial or complete tear of the ligament.
What Causes an MCL Sprain?
MCL sprains may be caused by a variety of things, such as:
- Direct impact to the outside of your knee
- Twisting or over-extending your knee
- Quickly changing directions when you’re walking or running
- Landing on your knee while it is bent
This type of injury is commonly seen in sports such as football, soccer, and skiing or following a car accident.
MCL Sprain Symptoms
The symptoms of an MCL sprain may include:
- Pain or difficulty when you are walking, sitting down, getting up from a chair, or climbing stairs
- Pain on the inside of your knee
- Swelling and bruising on the inside of your knee
- Swelling that spreads throughout your knee within 24–48 hours after the injury
- Stiffness in your knee
- Difficulty or pain when you try to bend or straighten your knee
- A feeling of instability in your knee
MCL Sprain Treatment
There are several treatments you may use to help find relief and healing from an MCL sprain, including:
- The R.I.C.E. method
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Bracing
- Physical therapy
R.I.C.E. Method
The R.I.C.E. method is often used to treat injuries such as MCL sprains. The components of the R.I.C.E. method include:
- Rest: Stay off of your injured knee to protect it from further injury.
- Ice: Apply an ice pack to the injured area several times each day for 15–20 minutes at a time to help reduce pain and swelling. Wrap ice in a towel or cloth and avoid applying it directly to your skin. Be sure not to apply ice for longer than 20 minutes at a time to prevent frostbite.
- Compression: Wrap your injured knee with an elastic bandage to help reduce swelling and provide support.
- Elevation: Keep your injured knee elevated above your heart to help reduce swelling.
The RICE method should be applied as soon as possible after the injury occurs and may be continued for the first 24–72 hours. If your pain increases or swelling persists for more than two days, consult your doctor or a physical therapist.
Non-Steroidal Anti-Inflammatory Drugs
After an MCL sprain, non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen (Advil, Motrin) and naproxen (Aleve) are often recommended to help relieve swelling.
Bracing
Your doctor may recommend a knee brace to help stabilize your knee through the healing process. Some MCL sprains may heal within a month or so. For more severe injuries, you may need to wear a hinged knee brace and limit the amount of weight you put on your leg.
Physical Therapy
Physical therapy is crucial for regaining full mobility and strength after an MCL sprain. A physical therapist will guide you through exercises and stretches designed to restore your knee’s function, reduce pain, and prevent further injury.
By understanding the causes, symptoms, and treatment options for MCL sprains, you can take proactive steps to manage your recovery effectively. Always consult with your healthcare provider to determine the best treatment plan for your specific condition.
Ankle + Foot
Ankle injuries are prevalent and can make walking or moving difficult. These injuries often stem from poor posture and improper limb placement during activities like walking, running, or playing sports. The way we lift and land our feet is crucial. Individuals with flat feet or low arches may experience soreness and pain without proper footwear. Discomfort in the ankle and foot can lead to compensatory issues higher up the body. At HB BodyLab, we aim to educate our clients on the proper mechanics of the ankle and foot to prevent and manage these injuries.
Common Ailments Treated at HB BodyLab:
Heel spurs are painful, and they can get in the way of your normal routine if you have discomfort while walking or exercising.
So, what’s the solution?
In this guide, you’ll learn all about heel spurs and your best treatment options.
What Are Heel Spurs?
A heel spur is a condition in which your heel bone develops a calcium deposit growth that can cause discomfort when you are walking or exercising.
What Causes Heel Spurs?
Heel spurs happen for many reasons.
Most commonly, a heel spur will develop when the muscles in your feet are constantly under strain.
Repetitive Exercise
Athletes who are constantly running or jumping put a lot of strain on their feet, and sometimes develop heel spurs.
If you are someone who likes to run long distances for fun, your physical therapist might suggest switching up your exercise routine occasionally.
Obesity
People who are overweight or obese can also put extra strain on their feet when they walk and are more prone to foot issues like heel spurs.
If you are overweight, your doctor or therapist can suggest ways to exercise without putting too much pressure on your feet.
Improper Footwear
Shoes can make a big difference in the health of your feet.
If you’re an avid hiker, for instance, make sure to wear high-quality, good-fitting hiking shoes. Wearing the wrong shoes for certain activities can put extra strain on your feet and lead to heel spurs.
Consistently wearing high-heeled shoes can also contribute to foot and ankle problems.
Heel Spurs Symptoms
There are many symptoms that can indicate heel spurs. To be sure if you have heel spurs, make sure to talk to your doctor.
Some common symptoms of a heel spur include:
- Sharp pain in your heel: You might have a heel spur if you experience a sharp pain in your heel, especially when you first wake up in the morning.
- A dull ache in your heel: Throughout the day as you use your feet, you might feel a dull ache in your heel.
- Inflammation and swelling: Sometimes when you have a heel spur, there will be inflammation and swelling around your heel.
Treatment Options for Heel Spurs
Rest and Ice
Resting your feet and applying ice packs can help reduce inflammation and pain. Avoid activities that put excessive strain on your heels.
Proper Footwear
Switch to supportive shoes that provide good arch support and cushioning for your heels. Avoid wearing high heels or worn-out shoes.
Orthotic Inserts
Custom or over-the-counter orthotic inserts can provide additional support and reduce pressure on the heel.
Stretching and Strengthening Exercises
Regular stretching and strengthening exercises can help alleviate tension in the foot muscles and improve overall foot health. A physical therapist can guide you through specific exercises tailored to your condition.
Anti-Inflammatory Medications
Over-the-counter anti-inflammatory medications like ibuprofen can help reduce pain and inflammation. Always consult your doctor before taking any medication.
Physical Therapy
Physical therapy can be highly effective in treating heel spurs. A therapist can use various techniques, including manual therapy, ultrasound, and specific exercises, to relieve pain and promote healing.
Corticosteroid Injections
In severe cases, corticosteroid injections may be recommended to reduce inflammation and pain. This treatment should be discussed with your doctor, as it may not be suitable for everyone.
Surgery
If conservative treatments do not provide relief, surgery may be considered as a last resort. Surgery involves removing the heel spur and addressing any associated issues, such as plantar fasciitis.
By understanding the causes, symptoms, and treatment options for heel spurs, you can take proactive steps to manage your condition and find relief from pain and discomfort. Always consult with your healthcare provider to determine the best treatment plan for your specific situation.
You just had an exhilarating workout session.
You managed to push your limits, running faster and longer than ever before.
Later, you begin to notice an aching sensation in the back of your ankle that lingers.
You could be experiencing Achilles tendonitis.
In this guide, we will explore the causes and symptoms of Achilles tendonitis, and discuss the treatment options available to help you recover.
What is Achilles Tendonitis?
Achilles tendonitis refers to the painful inflammation of the Achilles tendon.
The Achilles tendon is the largest tendon in your body, connecting your calf muscles to your heel bone.
This tendon allows your body to:
- Walk/run
- Jump
- Climb stairs
- Stand on your tiptoes
While this tendon can handle a lot of stress from these activities, overuse and degeneration of the Achilles tendon can result in Achilles tendonitis.
What Causes Achilles Tendonitis?
Any activity that puts repetitive stress on the Achilles tendon can cause Achilles tendonitis.
Certain risk factors can increase the chances of developing Achilles tendonitis.
Risk Factors for Achilles Tendonitis
There are several risk factors for Achilles tendonitis, including:
- Age: As you get older, the structure of the Achilles tendon begins to weaken, making you more susceptible to Achilles tendonitis.
- Sex: Studies show that males may be at a greater risk for developing Achilles tendonitis than females.
- Foot/calf problems: Having flat feet or chronically tight calf muscles can strain the Achilles tendon. Bone spurs can also rub against the Achilles tendon and cause Achilles tendonitis.
- Medical conditions: Conditions like obesity, high blood pressure, and diabetes can alter the structure and integrity of the Achilles tendon.
- Medications: Taking certain antibiotics, such as fluoroquinolones, is linked to a higher risk of developing Achilles tendonitis.
Achilles Tendonitis Symptoms
Achilles tendonitis pain is located along the Achilles tendon in the back of the heel or ankle area.
If you have Achilles tendonitis, you may experience some or all of the following symptoms:
- Pain: Especially after physical activity or exercise
- Tenderness to touch
- Stiffness
- Swelling
Always consult with your doctor about symptoms you are experiencing, as it is important to rule out other possible foot and ankle injuries.
Treatment for Achilles Tendonitis
There are various treatment options available for Achilles tendonitis. Your doctor will recommend the best approach based on the severity of your condition.
Rest and Ice Resting and applying ice to the affected area can help reduce pain and inflammation.
Stretching and Strengthening Exercises Your doctor or physical therapist can recommend specific exercises to help stretch and strengthen the Achilles tendon and surrounding muscles.
Orthotics Using orthotic devices, such as heel lifts or custom insoles, can help reduce stress on the Achilles tendon.
Medications Over-the-counter pain relievers, such as ibuprofen or naproxen, can help manage pain and reduce inflammation.
Physical Therapy A physical therapist can work with you to develop a personalized rehabilitation program to help you recover from Achilles tendonitis and prevent future injuries.
Surgery In severe cases, surgery may be necessary to repair the damaged Achilles tendon. This is usually considered a last resort when other treatment options have not been effective.
By understanding the causes, symptoms, and treatment options for Achilles tendonitis, you can take steps to manage your condition and get back to your normal activities.
If you are experiencing drop foot, you know how it can affect your daily life.
Difficulty walking, scraped toes from foot-dragging, and numbness in your foot can all be incredibly frustrating symptoms to handle on a day-to-day basis.
There are ways to help alleviate your symptoms and frustrations.
In this guide, we will discuss the causes and symptoms of drop foot, physical therapy options, and how other medical treatments can help.
What is Drop Foot?
Drop foot refers to the inability to lift the foot due to its weakened or paralyzed muscles.
Drop foot makes it difficult to walk, either resulting in:
- Dragging the foot along the ground; or
- Bending the knees to lift the foot higher above the ground than normal to avoid dragging it, which results in an abnormal gait
Drop foot can occur in either one or both of the feet and can be temporary or permanent.
3 Common Causes of Drop Foot
Drop foot is not a disease, but rather a symptom of a neurological, anatomical, or muscular problem.
Below are some common drop foot causes.
#1: Nerve Injury
Nerve injury can cause foot drop to occur, as certain nerves stimulate muscles to perform functions involving the foot.
Some common nerve injuries that cause foot drop include:
- Compression of the peroneal nerve, which is the nerve that controls the leg muscles responsible for lifting the foot. This is one of the most common causes of drop foot.
- Nerve root injury, which can also be referred to as a “pinched nerve” in the spine.
People with diabetes may be more at risk of developing drop foot due to their susceptibility to nerve disorders.
#2: Neurological or Muscular Disorders
Disorders that cause compression or damage to nerves or muscle weakness can cause drop foot.
Some neurological and muscular disorders that can cause drop foot include:
- Various forms of muscular dystrophy
- Polio
- Charcot-Marie-Tooth disease
#3: Brain and Spinal Cord Disorders
Disorders that affect the spinal cord or the brain can cause drop foot.
Some examples of disorders of the brain and spinal cord that can cause drop foot include:
- Stroke
- Multiple Sclerosis
- Amyotrophic lateral sclerosis (ALS)
Drop Foot Symptoms
You can experience drop foot symptoms in one or both of your feet.
Some symptoms of drop foot you experience may include:
- Inability to lift the foot
- Dragging your toes or top of the foot when walking
- Numbness in the top of your toes or foot from foot dragging
- Developing a foot drop gait in order to avoid foot dragging
It is important to always discuss your symptoms with your doctor in order to rule out other foot and ankle injuries.
Risk Factors for Drop Foot
You could be increasing your risk of developing drop foot from peroneal nerve compression without realizing it.
Here are some examples of behaviors that can increase your risk of developing drop foot:
- Crossing your legs — Frequently crossing your legs can cause peroneal nerve compression and lead to drop foot.
- Prolonged kneeling — Occupations that require you to kneel for long periods of time can increase your risk of developing drop foot.
- Wearing a leg cast — Plaster casts can compress the peroneal nerve when enclosing the ankle and ending just below the knee.
Physical Therapy for Drop Foot
Physical therapy can be an effective treatment for drop foot, helping to strengthen the muscles and improve mobility.
Exercises
- Stretching exercises: Stretching the calf muscles and Achilles tendon can help improve flexibility and range of motion.
- Strengthening exercises: Exercises that target the muscles of the lower leg and foot can help improve strength and stability.
- Gait training: Physical therapists can work with you to improve your walking pattern and reduce the risk of falls.
Other Treatments
- Bracing: Wearing an ankle-foot orthosis (AFO) can help support the foot and ankle, making it easier to walk.
- Electrical stimulation: This treatment uses electrical impulses to stimulate the muscles and improve strength and function.
- Surgery: In severe cases, surgery may be necessary to repair or decompress the affected nerve.
By understanding the causes, symptoms, and treatment options for drop foot, you can take steps to manage your condition and improve your quality of life. Always consult with your doctor or a physical therapist to determine the best course of action for your specific situation.
After a long day at work, you finally sit down to relax. But when you get up to move again, a sharp pain shoots through the bottom of your foot.
This pain could be a sign of plantar fasciitis.
In this guide, we’ll discuss the signs and symptoms of plantar fasciitis, as well as treatment options to help reduce your pain.
What is Plantar Fasciitis?
Plantar fasciitis refers to inflammation of the plantar fascia, a thick band of connective tissue on the bottom of your foot that connects your heel bone to your toes.
Plantar fasciitis pain typically occurs:
- During your first steps after resting
- After long periods of standing
- After sitting for an extended period
- Following physical activities such as walking or running
What Causes Plantar Fasciitis?
Plantar fasciitis occurs when too much tension and stress on the plantar fascia result in small tears in the tissue.
Some factors and activities that can increase your risk of plantar fasciitis include:
- Sports activities: Engaging in sports like tennis or basketball that require sudden movements and jumps can strain your feet.
- Age: With advancing age, the plantar fascia loses its elasticity, making individuals between 40 and 60 more vulnerable.
- Excess weight: Carrying extra pounds adds more stress to the plantar fascia, leading to inflammation and tears.
- Foot mechanics: Conditions such as flat feet, high arches, or abnormal walking patterns can put additional stress on the plantar fascia.
- Occupational hazards: Jobs that require prolonged periods of standing or walking, like teaching or working in retail, can increase the risk.
Plantar Fasciitis Symptoms
The main symptom of plantar fasciitis is sharp pain on the bottom of the foot, usually originating from the heel.
Pain is often more severe in the morning and after periods of inactivity but may improve slightly with movement.
Plantar Fasciitis Treatment
If you have plantar fasciitis pain, you’re likely looking for ways to alleviate it.
Here are some treatment options to consider:
- Medications: Anti-inflammatory medications like ibuprofen and naproxen can help reduce pain and inflammation.
- Therapies:
- Physical therapy: A physical therapist can introduce specific stretching exercises to help relieve pain.
- Night splints: These devices keep your calf and foot stretched overnight to alleviate morning pain.
- Orthotics: Custom-fitted arch supports or specialized shoes can reduce stress on the plantar fascia.
- Other treatments:
- Injections: Steroid injections can provide temporary pain relief, but repeated use can weaken the plantar fascia.
- Extracorporeal shock wave therapy: This treatment uses sound waves to stimulate healing in chronic cases.
- Ultrasonic tissue repair: This procedure involves using a needle-like probe to break up and remove damaged tissue.
- Surgery: As a last resort, surgery may be performed to detach the plantar fascia from the heel bone.
By understanding plantar fasciitis and exploring various treatment options, you can find the relief you need and return to your daily activities with less pain.
You were rushing down the stairs and missed the last step.
As you stumble, your ankle twists painfully, leaving you wincing in discomfort.
This searing pain could be a sign of an ankle sprain.
In this guide, we’ll discuss the causes and symptoms of ankle sprains and whether physical therapy might be the treatment you need.
What Is an Ankle Sprain?
A sprained ankle is a common injury that occurs when the ligaments supporting the ankle joint stretch beyond their normal range or tear due to sudden twisting or rolling.
These ligaments act like stabilizing bands, preventing excessive movement. When they are overstretched or torn, it can lead to varying degrees of pain and instability.
ANKLE SPRAIN GRADES
The severity of an ankle sprain is categorized into three grades:
- Grade 1: Mild stretching or a slight tear of the ligament with minimal pain, swelling, and difficulty walking.
- Grade 2: Moderate tearing of the ligament with noticeable pain, swelling, bruising, and difficulty bearing weight.
- Grade 3: Complete tear of the ligament, resulting in severe pain, swelling, bruising, and inability to walk without significant discomfort.
What Causes an Ankle Sprain?
An ankle sprain can occur whenever the ligaments in the ankle joint are overstressed. Here are four common causes:
REPETITIVE MOTION
Repetitive movements can increase the risk of an ankle sprain. You can minimize your risk by:
- Wearing appropriate footwear for activities
- Avoiding uneven surfaces during exercise
FALLING
A misstep or fall that causes the ankle to twist or roll can easily result in a sprain.
SPORTS
Athletes are particularly prone to ankle sprains, especially during activities involving sudden changes in direction or jumping.
TRAUMA
Traumatic events, such as an accident where the foot is trapped or impacted forcefully, can also cause ankle sprains.
Ankle Sprain Symptoms
Symptoms of an ankle sprain vary depending on the severity of the injury but may include:
- Tenderness to touch
- Pain: Especially when walking or bearing weight
- Bruising
- Swelling
- Loss of range of motion
- Ankle instability
- A popping sensation: Felt or heard at the time of injury
It is important to consult with your doctor to rule out other potential injuries and get a proper diagnosis.
By understanding the causes and symptoms of an ankle sprain, you can take steps to prevent it and seek appropriate treatment if it occurs.
You can barely stand the burning, tingling sensation in your feet.
Living with peripheral neuropathy symptoms can be incredibly challenging.
Fortunately, there are numerous treatment options available that can help alleviate your pain and symptoms.
In this guide, we’ll cover the signs and symptoms of peripheral neuropathy and the treatment plans available to you.
What is Peripheral Neuropathy?
Peripheral neuropathy occurs when there is damage to the peripheral nerves, which branch off from the spinal cord and extend to various parts of the body.
Peripheral neuropathy typically affects the hands and feet, causing pain, numbness, and weakness. It can also impact other parts of the body.
What Causes Peripheral Neuropathy?
Peripheral neuropathy results from damage to the peripheral nerves, which can be caused by various medical conditions.
Some examples of health conditions that cause peripheral neuropathy include:
- Diabetes: This is the most common cause of peripheral neuropathy. Studies show that nearly 50% of adults with diabetes develop peripheral neuropathy.
- Autoimmune diseases: Conditions such as Sjogren’s syndrome, lupus, rheumatoid arthritis, Guillain-Barre syndrome, chronic inflammatory demyelinating polyneuropathy, and vasculitis can increase your risk.
- Tumors: Malignant or benign growths can develop on the nerves or press against them, causing peripheral neuropathy. Some cancers related to the body’s immune response are known as paraneoplastic syndrome and can trigger peripheral neuropathy.
- Inherited disorders: Hereditary types of neuropathy, such as Charcot-Marie-Tooth disease, can result in peripheral neuropathy.
- Bone marrow disorders: Abnormal protein in the blood, bone marrow cancer, lymphoma, and amyloidosis can increase your risk.
- Infections: Certain infections that can result in peripheral neuropathy include Lyme disease, hepatitis B and C, shingles, Epstein-Barr virus, diphtheria, and HIV.
Other causes of peripheral neuropathy include:
- Alcoholism
- Exposure to toxins
- Certain medications like chemotherapy
- Trauma or nerve compression
- Vitamin deficiencies, such as B vitamins, vitamin E, and niacin
Peripheral Neuropathy Symptoms
Symptoms vary depending on the type of nerve affected. There are three classifications for peripheral nerves:
- Sensory nerves: Sense temperature, pain, vibration, or touch from the skin.
- Motor nerves: Control muscle movement.
- Autonomic nerves: Control blood pressure, heart rate, digestion, and the bladder.
Common symptoms of peripheral neuropathy include:
- Numbness and tingling in the feet or hands, which can spread up the legs or arms
- Stabbing or burning pain
- Extreme sensitivity to touch
- Abnormal pain from activities that should not cause pain, such as bearing weight on your feet
- Loss of coordination and increased falling risk
- Muscle weakness
- Paralysis if the motor nerves are affected
If autonomic nerves are affected, you may experience:
- Intolerance to heat
- Excessive sweating or inability to sweat
- Bladder, bowel, or digestive problems
- Dizziness or light-headedness caused by changes in blood pressure
Peripheral neuropathy can affect one nerve or multiple nerves simultaneously. Be sure to discuss your symptoms with your doctor to rule out other injuries and receive a proper diagnosis.
You’re finishing up a game of tennis when you suddenly feel a sharp pain in the back of your ankle.
Now, each time you step, the pain returns, making it hard to walk.
This could be a symptom of peroneal tendonitis.
In this guide, we will explore the signs and symptoms of peroneal tendonitis, as well as treatment options, including physical therapy.
What is Peroneal Tendonitis?
Peroneal tendonitis involves inflammation of the peroneal tendons, which are located on the outside of the ankle.
The peroneal tendons help:
- Support ankle joints and prevent sprains
- Turn the feet outward
- Stabilize the arch of your feet during movement
When these tendons are overused, they can become irritated and inflamed, leading to peroneal tendonitis.
What Causes Peroneal Tendonitis?
Peroneal tendonitis often occurs in athletes and active individuals who perform repetitive motions. Some common causes include:
- Sudden increase in physical activity: Rapidly intensifying your exercise routine or starting a new activity.
- Overuse: Repetitive strain from activities like running, hiking, or dancing.
- Improper footwear: Wearing shoes that lack proper support.
- Foot structure: Having high arches or other structural foot abnormalities.
- Weak or imbalanced muscles: Insufficient strength in the lower limb muscles or muscle imbalances.
- Incorrect technique: Poor form during physical activities.
Preventing Peroneal Tendonitis
To help prevent peroneal tendonitis, consider the following tips:
- Stretch regularly: Ensure you stretch your calves and peroneal muscles before engaging in physical activities.
- Choose supportive footwear: Invest in shoes that offer good support and cushioning.
- Gradual training: Increase the intensity and duration of your activities slowly to avoid overuse injuries.
- Maintain activity levels: Stay active year-round, even if your primary sport is seasonal, to keep muscles conditioned.
- Strengthen muscles: Work on strengthening the muscles in your legs and ankles to provide better support.
Symptoms of Peroneal Tendonitis
If you have peroneal tendonitis, you might experience:
- Swelling and pain along the back or outside of the ankle
- Increased pain during activities and relief during rest
- Discomfort when turning the foot outward
- Ankle instability or weakness
- Warmth and tenderness around the affected area
It’s crucial to consult with a doctor to confirm the diagnosis and rule out other potential injuries.
Treatment Options for Peroneal Tendonitis
Treatment for peroneal tendonitis typically involves a combination of rest, therapy, and supportive measures:
- Rest: Minimize activities that put strain on your ankle.
- Physical Therapy: Engage in exercises designed to strengthen the surrounding muscles and improve flexibility.
- Proper Footwear: Wear shoes that provide adequate support and cushioning.
- Orthotics: Custom orthotic devices can help support your feet and reduce strain on the tendons.
- Medication: Over-the-counter anti-inflammatory drugs can help reduce pain and swelling.
- Ice Therapy: Apply ice packs to the affected area to reduce inflammation and numb the pain.
By following an appropriate treatment plan, you can alleviate the symptoms of peroneal tendonitis and return to your regular activities.
You’ve sustained an ankle injury. After a period of hobbling around on crutches and sporting a cast, it’s time to embark on the road to recovery.
However, returning to your usual activities might not be as simple as tossing aside those crutches. Despite your bones having knitted back together, your ankle’s muscles, ligaments, and joints might need some assistance in regaining:
- Strength
- Flexibility
- Stability
Physical therapy post-ankle fracture is crucial for continuing your healing journey and reclaiming your normal routine.
This guide will shepherd you through your recovery process after an ankle fracture, one step at a time.
Understanding An Ankle Fracture
An ankle fracture, or commonly known as a broken ankle, occurs when one or more of the three bones in the ankle joint—tibia (shinbone), fibula (outer ankle bone), and talus (the bridge between leg and foot)—suffer fractures.
These fractures can be painful and temporarily incapacitating.
The severity of a broken ankle varies, ranging from tiny stress fissures to compound breaks that puncture the skin.
Causes of An Ankle Fracture
A broken ankle typically results from a twisting or rotational injury, although direct impacts can also lead to it.
Common triggers include:
- Missteps
- Tumbles
- Sports Mishaps
- Vehicle Collisions
Symptoms Following An Ankle Fracture
After fracturing your ankle, your physician will likely advise against putting any weight on the injured foot initially. Premature ankle use could impede proper bone healing.
The no-weight-bearing period usually spans 6 to 10 weeks, contingent on the fracture’s severity.
During this phase, you may require:
- A Splint
- A Sturdy Cast
- A Walking Boot
- Crutches
But what happens once the ankle fracture has mended?
Upon cast removal and receiving the green light to resume walking, a fresh chapter of recovery unfolds.
Diminished Muscle Strength
After bone healing, you might observe that your muscles have atrophied and weakened due to disuse.
Stiffened Ligaments and Restricted Range-of-Motion
Extended immobilization often leads to joint stiffness, persisting even after regaining mobility. You may encounter difficulty in moving your ankle as freely as before the injury.
You’re grappling with the discomfort of bunions.
Years of squeezing into tight shoes and enduring prolonged periods on your feet have taken their toll.
And now, you yearn for relief.
Your quest for bunion pain remedies led you to scour the internet. And lo and behold, you’ve stumbled upon us. Fortunately, we have the solutions you’ve been seeking.
In this guide, we’ll delve into everything you need to know about the origins and manifestations of bunions, along with treatments to grant you the respite you crave.
Unraveling Bunions
Bunions manifest as bony protrusions forming on the joint at the base of your big toe. These developments occur gradually over the years.
They arise when bones in the forepart of your foot shift out of alignment, pulling the tip of your big toe toward your smaller toes—thus causing the joint at the base of your big toe to protrude.
In Latin, bunions are dubbed as hallux valgus. “Hallux” denotes big toe, while “valgus” signifies turned away from the body’s midline.
Smaller variants, dubbed bunionettes, can also emerge on the joint of your little toe.
Bunions may be accompanied by calluses and hardened skin.
Triggers of Bunions
While snug, constrictive footwear is often blamed for bunions, Harvard Medical School suggests that this might not be the sole culprit.
Indeed, genetics may play a pivotal role.
What do we mean by that?
The structure of your foot is inheritable. If you possess low arches, flat feet, or lax joints, you might be predisposed to bunions.
Moreover, 35% of women aged 35 and above contend with bunions. Several factors make women more susceptible, including:
- Regularly donning tight shoes, especially high heels.
- Pregnancy, which induces hormonal changes loosening foot ligaments, thereby heightening the risk of bunions and other podiatric issues.
- Occupations that demand prolonged standing, such as ballet dancers, teachers, and nurses, elevate the likelihood of bunion formation due to recurrent foot stress.
Other bunion triggers encompass:
- Certain arthritis forms, like rheumatoid arthritis.
- Neurological and articular conditions like polio or Charcot-Marie-Tooth disease.
- Foot traumas such as sprains, fractures, or nerve impairments.
- Congenital abnormalities.
Signs and Symptoms of Bunions
Bunion symptoms typically manifest on the bunion’s side and worsen when wearing snug shoes or standing for extended durations.
Common indicators include:
- Swelling
- Deformity
- Tenderness
- Stiffness
- Pain or soreness
- Inflammation and redness
- Burning sensation
- Potential numbness
Over time, the affected region may become glossy and warm to the touch. Since bunions are progressive, they persist and usually exacerbate over time.
Though bunions cannot be reversed, treatment avenues exist to assuage symptoms.
You’ve grown weary of the discomfort and impediments to your daily routines caused by posterior tibial tendonitis.
Seeking respite from your symptoms, you’re on the lookout for comprehensive information.
Your quest ends here.
In this guide, we’re unraveling insights, exercises, and more to aid you in overcoming posterior tibial tendonitis, enabling you to resume your passions without distress.
Unveiling Posterior Tibial Tendonitis
Your posterior tibial tendon plays a crucial role as a major support structure in your foot, linking the calf muscle to the bones along the inner side of your foot.
Posterior tibial tendonitis (PTT) or posterior tibial tendon dysfunction (PTTD) is a prevalent foot and ankle condition. PTT arises from alterations in the tendon, leading to inadequate support for your foot’s arch.
It stands as the primary cause of flatfoot in adults, presenting as a progressive ailment that can curtail mobility, induce pain, and weaken your ankle and foot.
Triggers of Posterior Tibial Tendonitis
The foremost trigger for posterior tibial tendonitis is tendon overuse. PTT may also stem from traumatic impacts, such as falls or sports-related collisions.
Athletes, particularly dancers and gymnasts, and individuals with highly active lifestyles are at heightened risk of posterior tibial tendonitis.
Additionally, degenerative changes linked to arthritis or pre-existing flatfoot (pes planus) can contribute to PTT.
Risk Factors for Posterior Tibial Tendonitis
Certain demographics are predisposed to PTT, including:
- Women
- Individuals aged 40 and above
- Diabetics
- Young athletes
- Individuals with hypertension
- Rheumatoid arthritis sufferers
Other risk factors encompass:
- Obesity
- Steroid usage
- Previous ankle traumas
Symptoms of Posterior Tibial Tendonitis
Posterior tibial tendonitis typically manifests in one foot but can affect both. Common symptoms comprise:
- Pain along the inner arch, heel, or ankle
- Swelling
- Flattening of the foot arch
- Inward rolling of the ankle
- Redness
- Foot discomfort intensifying with running, jumping, climbing, or prolonged standing
- Outward rotation of the toes and foot
Symptoms typically arise following activities like running, walking, or stair climbing. As PTT advances, your pain’s localization may shift.
With the flattening of your foot and the displacement of the heel bone due to PTT, you might experience discomfort on the outer side of your foot and ankle, potentially culminating in arthritis in the affected areas.
Experiencing discomfort in your heels? It could be attributed to flat feet.
Feeling knee pain? It might be linked to your flat feet.
Suffering from backaches? Your flat feet could be the culprit.
Your body operates like a complex machine, and when your feet aren’t functioning optimally, it can reverberate throughout various areas. If you suspect that flat feet are the root cause of your discomfort, physical therapy offers a viable solution.
Unsure whether you have flat feet? This article serves to demystify flat feet and unveil strategies for finding relief.
Unraveling Flat Feet
Flat feet denote feet lacking a normal or absent arch, also referred to as fallen arches. This anatomical feature results in the entire soles of your feet making contact with the ground when standing.
Such a condition can precipitate over-pronation, characterized by the inward rolling of the foot. If you inspect your shoes from the rear, you’ll likely observe greater wear on the inside of the heels compared to the outer edges.
From infancy, we all begin with flat feet, with arches typically forming by age 6. Nonetheless, approximately one or two out of every ten children retain flat feet into adulthood.
The Two Types of Flat Feet
Flat feet can generally be categorized into two types:
- Flexible flat feet: Exhibiting a normal arch when non-weight bearing, yet becoming absent when standing or walking.
- Rigid flat feet: Characterized by a perpetual absence of arch, whether weight-bearing or at rest, earning the designation of “true” flatfootedness.
Causes of Flat Feet
Flat feet are prevalent among children and can arise from various factors:
- Genetics
- Tight Achilles tendons
- Ligament laxity
- Inadequate foot exercise
In adults, flat feet can manifest through diverse pathways, including:
- Hereditary factors
- Injuries and fractures
- Excessive strain and overuse
- Advancing age
- Arthritis
- Diabetes or obesity
- Tendon injuries or failures
- Achilles Equinus contracture
- Pregnancy
- Neurological or muscular disorders
Symptoms of Flat Feet
The arch of your foot serves as a natural shock absorber for your entire body. With flat feet, this arch is compromised or absent, impacting your overall bodily comfort.
Common symptoms associated with flat feet encompass:
- Heel, foot, and ankle pain
- Fatigue in the feet, arches, and legs
- Pain in the knees, hips, and lower back
- Inward rolling of the ankles
- Irregular walking patterns
- Shin splints
- Bunions
- Hammertoes
- Arthritis
- Plantar fasciitis
- Posterior tibial tendon dysfunction (PTTD)
You don’t have to be a top-tier athlete to encounter ankle impingement. While it’s more prevalent among gymnasts, runners, and dancers, individuals engaging in repetitive tasks like squatting or descending stairs are equally vulnerable.
If you’re grappling with anterior or posterior ankle discomfort, you might be pondering whether physical therapy for ankle impingement holds the key to relief. And if so, what does the process entail?
Fortunately, the adept physical therapists at In Motion O.C. have assisted numerous patients with ankle impingement. Here’s our guidance for you.
Understanding Ankle Impingement
Ankle impingement injuries typically manifest in two forms:
Anterior ankle impingement: Characterized by pain, inflammation, and swelling on the front side of your ankle. Left untreated, this condition may culminate in bone spurs.
Posterior ankle impingement: Involves pain at the back of your ankle, particularly when pointing your toes, stemming from compression of the bony tissue between the heel bone and the shin bone.
Triggers of Ankle Impingement
Anterior ankle impingement often results from repetitive activities such as jumping, squatting, or descending stairs. Ankle instability can also play a contributory role.
The laxity of the ankle joint, often stemming from recurrent ankle sprains, may lead to ligament damage, subsequent scarring, and increased joint space occupancy. Consequently, tissue compression ensues, provoking discomfort during toe-to-shin stretching maneuvers.
Posterior impingement may be induced by an additional bone at the rear of the ankle, promoting compression between the heel bone and the shin bone. Pain is often experienced when pointing the toes.
Excessive force exerted on the ankle can result in the fracturing of small bone fragments, causing compression upon toe movement downward, and subsequently instigating swelling and inflammation, culminating in pain.
Symptoms of Ankle Impingement
Anterior and posterior ankle impingement injuries present distinct causes and, consequently, disparate symptoms.
Anterior Ankle Impingement Symptoms
- Ankle instability
- Diminished range of motion when flexing toes toward the shin
- Pain localized on the outer and/or front aspect of the ankle joint
- Tenderness upon palpation of the front ankle area
- Pain at the end of toe-to-shin stretching maneuvers
Posterior Ankle Impingement Symptoms
- Restricted range of motion upon toe pointing
- Pain or tenderness at the back of the ankle upon touch
- Discomfort at the rear of the ankle during activities or when toe-pointing
If you’re an avid football, soccer, or rugby player, turf toe might not be unfamiliar territory.
The agony it brings can sideline you, keeping you off the field and on the bench.
In this guide, we’ll delve into the causes and symptoms of turf toe and explore whether physical therapy for turf toe can be your ticket back to the game.
Deciphering Turf Toe
Turf toe is the colloquial term for a sprained metatarsophalangeal (MTP) joint.
Your MTP joint resides at the juncture where your metatarsal—the first elongated, straight bone in your foot—joins with the phalanx, the initial short bone in your big toe.
These joints facilitate both upward and downward movements of your toe.
Your big toe is pivotal for walking and running. As you step, it’s the final joint your foot engages before propelling your body forward.
Injury to your MTP joint and the surrounding foot structures may involve:
- Ligaments
- Muscle tendons; or
- The sesamoid bones (small bones beneath your big toe)
Triggers of Turf Toe
Turf toe arises when your big toe is forcefully extended beyond its typical range of motion towards the top of your foot. Typically, the front of your foot is immobilized and thrust into the ground, causing excessive backward hyperextension of your big toe.
A turf toe injury may encompass:
- Subluxation: Occurs when one of the MTP joint bones slips out of alignment but returns to its original position; or
- Dislocation: Involves complete separation of the two MTP joint bones
This injury is most prevalent among athletes, particularly those engaged in football, soccer, or rugby, and any sport involving jumping.
Surgical intervention for turf toe is rarely necessary.
Symptoms of Turf Toe
Common turf toe symptoms include:
- Sensation of “popping” around or at the MTP joint
- Pain at the MTP joint
- Bruising
- Swelling
- Tenderness upon touch; and
- Arch cramping
In severe cases, MTP dislocation can occur, resulting in joint deformity.
Turf Toe Physical Therapy – Can PT Aid Recovery?
Absolutely!
Physical therapy for turf toe can expedite healing by offering:
- Range of motion exercises
- Muscle strengthening around the MTP joint
- Manual therapy to enhance range of motion; and
- Patient education on injury prevention

Why Choose Us
Reason For Choosing Us
Muti-Disciplinary
We take a comprehensive, integrated approach to wellness, combining a myriad of disciplines to address your unique needs and achieve optimal health.
1 on 1 Care
At HB BodyLab, you'll spend your entire session with the doctor, ensuring personalized attention and care without being handed off to an aide or assistant.
Transparent Billing
At HB BodyLab, we prioritize transparent billing, providing you with upfront treatment costs before starting, so you can confidently navigate your healthcare journey.